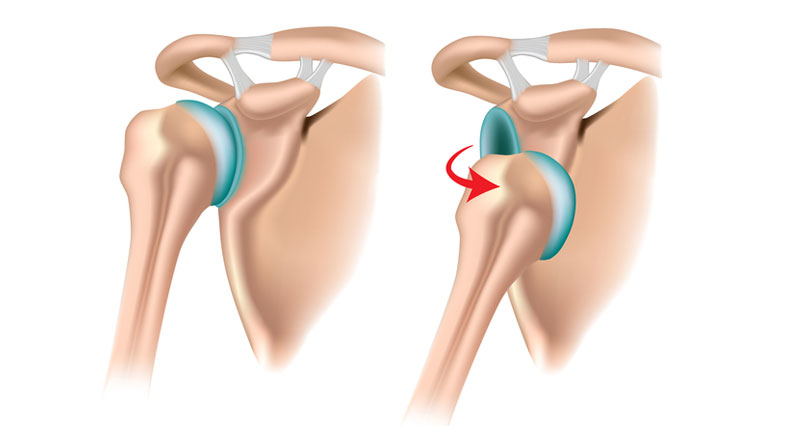
Our shoulder dislocation rehab program is created by professional sports physiotherapist Paul Tanner. It is based on what he does with his elite players but adapted for use by anyone.
Download the App to access our step-by-step Dislocated Shoulder Rehab Program created by professional Sports Physiotherapist Paul Tanner: iPhone & Android
Who is this shoulder dislocation rehab program suitable for?
This program is suitable for anyone who has suffered a shoulder dislocation or partial dislocation (subluxation). If you have had surgery then always follow your orthopaedic consultant’s recommendations. It consists of 5 phases. You only progress to the next phase when you reach specific exit criteria for each phase.
Phase 1: Dislocated shoulder rehab
Phase 1 is the acute management phase and begins as soon as possible after injury. The aim is to reduce pain and inflammation and protect your shoulder. If you have suffered a shoulder dislocation then you should seek professional advice immediately. Do not attempt to put it back in yourself.
During this phase, it is important to avoid abduction and external rotation of your shoulder. In other words, avoid lifting your arm out sideways and rotating it backwards. Treatment methods include immobilisation in a sling and applying cold therapy.

Phase 2: Dislocated shoulder rehab
This is the early rehabilitation phase. The aim is to begin to increase range of movement whilst still protecting the joint. Treatment methods consist of cold therapy, light massage and taping. Phase 2 comprises:
- 4 mobility, including pendulum exercises
- 6 strengthening exercises
- 1 proprioception exercise
- Stationary cycling
Phase 3: Dislocated shoulder rehab
This is the mid-rehabilitation stage. The aim here is to increase the strength and endurance of your rotator cuff muscles and upper limbs in general. In particular, not just in a safe range, but through the full range of movement. Treatment methods continue with taping to protect the joint along with introducing foam roller exercises for the upper back and arms. Phase 3 exercises consist of:
- 4 x stretching
- 1 x active mobility
- 14 x strengthening exercises
- 2 x functional exercises
- Return to running
Download the App to access our step-by-step Dislocated Shoulder Rehab Program created by professional Sports Physiotherapist Paul Tanner: iPhone & Android
Phase 4: Dislocated shoulder rehab
This is the late-stage rehabilitation and starts to get a little more interesting. The aim is to increase the function of your shoulder and it’s ability to cope with external forces. In other words, the shoulder’s capacity to generate and absorb force. Treatment can continue with massage if available. Exercises also include gentle stretching for the front of your shoulder.
- 4 x stretching
- 1 x active range of motion
- 15 x strengthening
- 4 x force absorption exercises
- 2 x functional
- Running progressions
Phase 5: Maintenance
By now we are expecting normal activity as well as continuing with rehab exercises. By now your shoulder should feel strong and you should have a full range of movement. However, the chance of recurrence is high, especially if you just stop doing all shoulder exercises. Therefore, this is a maintenance phase to try and mitigate the risk of future injuries. There are 24 exercises in this final maintenance phase.
About the author
Paul Tanner
Paul is head of Medical Services at Millwall Football Club, dealing with all aspects of match and training day sports physiotherapy and medical cover. His career also includes First Team Physio at Norwich City Football Club and Senior physiotherapist to London Wasps Rugby first-team squad.