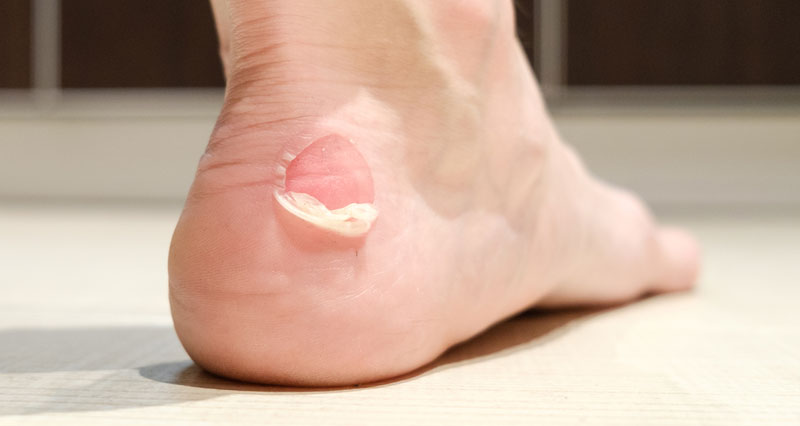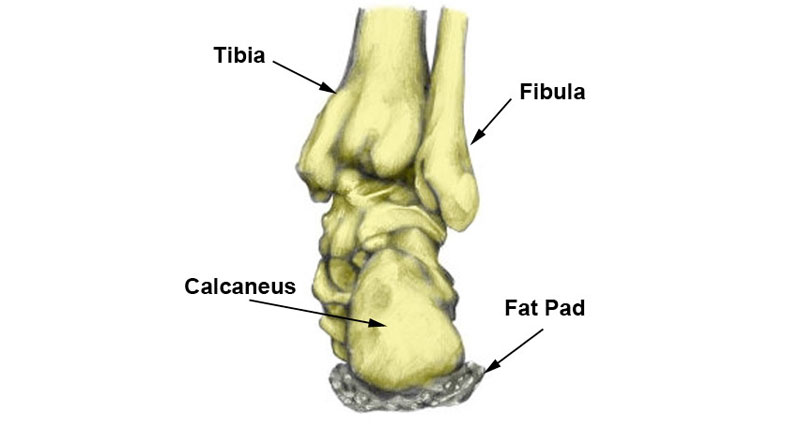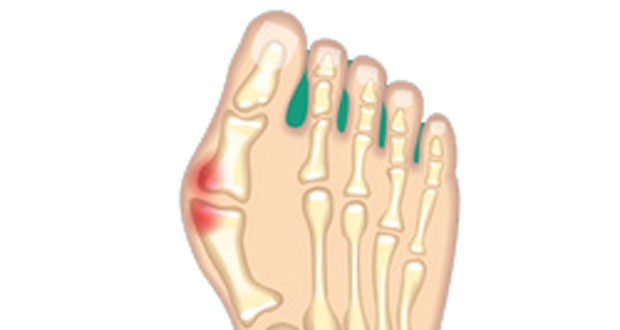
A bunion (also known as hallux valgus) is a painful swelling on the inside of the big toe. It develops gradually over time. Often the big toe looks bent inwards, towards the other toes.
Medically reviewed by Dr Chaminda Goonetilleke, 20th Jan. 2022
Bunion symptoms
Signs and symptoms of Bunions include:
- Forefoot pain develops gradually over time, becoming progressively worse.
- In particular, the inside of the base of your big toe is painful.
- Gradually deformity occurs on the inside of the forefoot.
- Specifically, you will experience pain in and around the base of the big toe, particularly on the inside.
- Wearing soft, wide-fitting shoes, or removing them completely relieves symptoms.
- Your big toe appears to bend inwards towards the other toes. In some cases, it can overlap the adjacent toe.
An X-ray may be done to determine the extent of the deformity, as well as any wear and tear of the joint.
What is a bunion?
A bunion (Hallux Valgus), is a painful swelling on the inside of the big toe. It occurs to some extent in almost a quarter of adults aged between 18 and 651. It is more common in women and older people. However, teenagers can also develop condition2.
Bony exostosis (small growths of bone) form around the joint at the base of the big toe, known as the first MTP joint. Eventually, deformity develops. Sometimes there is also inflammation of the bursa or a small sack of fluid that lubricates between tendon and bone.
In more severe cases the deformity can make it difficult to wear certain types of shoes. This is due to the pressure on the joint, or from bone rubbing against the shoe.
What causes a bunion?
Pressure
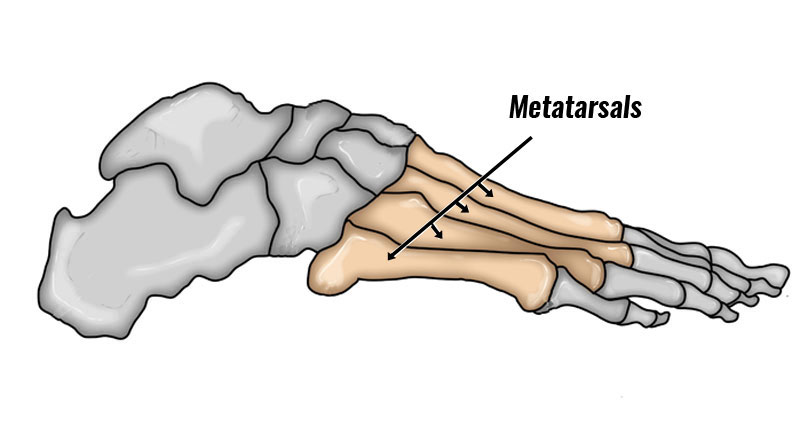
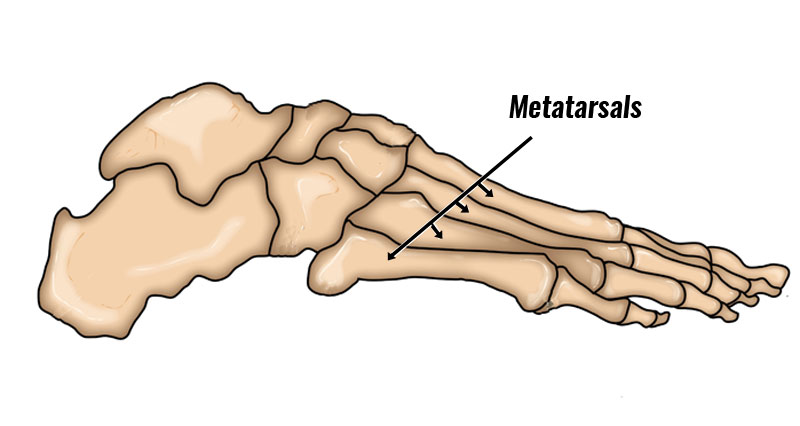
Pressure on the inside of the forefoot. As a result, the 1st metatarsal bone in the foot moves outwards.
Footwear
Wearing tight or poorly fitting shoes increases pressure on your forefoot.
Wearing high-heeled shoes regularly also increases the risk of developing the condition. This is because they increase the pressure on the forefoot.
Foot biomechanics
Biomechanical factors can contribute to the development of Hallux Valgus. For example, if you overpronate where the foot rolls in or flattens excessively which causes the inside of the foot to rub against the shoe.
Increased length of the first metatarsal bone in the foot3.
Age
Age is also a factor as the ligaments lose strength as you get older.
Other causes
Direct trauma or impact to the ligaments on the inside of the foot, or to the sesamoid bones.
Other causes include Achilles tendon shortening, degeneration of the joint, neuromuscular disorders, and collagen deficient diseases.
Treatment
Initial treatment for bunions is based on reducing pain and correcting any biomechanical problems of the foot. Later or in more severe cases surgery will be required.
Orthotic shoe inserts
If your foot rolls in (or overpronates) then this causes the arch of the foot to flatten. As a result, pressure increases on the base of the big toe, where the bunion forms.
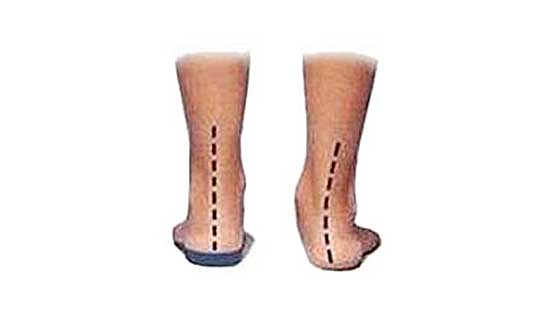
A podiatrist is a therapist who specializes in feet can do a full gait analysis and make orthotic inserts to correct biomechanical foot problems.
Off-the-shelf orthotic insoles are also available and suitable for most patients.
Taping
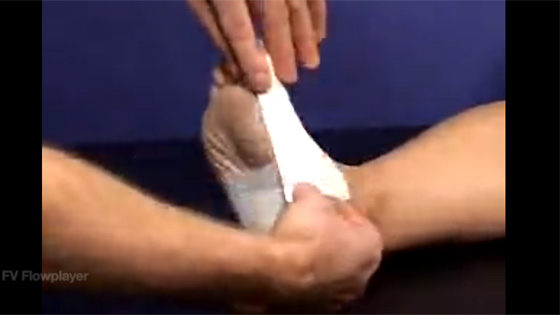
A simple taping technique can help align the toe joint and relieve symptoms.
Anchor strips are attached to either side of the bunion and then support strips help re-align the joint.
- More on Bunion taping
Bunion surgery
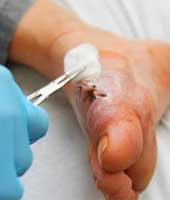
Severe cases may require surgery to realign the joint into a better position, but this is the last resort if conservative treatment has failed or just walking is painful.
Surgery is usually done as an outpatient procedure so the patient does not have to stay in a hospital overnight although it is usually performed under a general anesthetic.
The procedure involves the surgeon making a cut on the inside of the big toe joint and removing excess bone whilst also repositioning ligaments and tendons.
The joint is fixed with screws or wires which either dissolve or are removed later. In some cases, they remain in the foot permanently.
After the operation, the foot will be immobilized, often in a cast for 4 to 8 weeks to keep the bones in alignment. Crutches will usually be issued to help the patient get around.
After this period, the foot will be assessed to check the bones have healed correctly. At which point full weight bearing may be gradually introduced.
References & further reading
- Nix S, Smith M, Vicenzino B. Prevalence of hallux valgus in the general population: a systematic review and meta-analysis. J Foot Ankle Res 2010;3:21.
- Shine J, Weil L, Weil LS et al. Scarf osteotomy for the correction of adolescent hallux valgus. Foot Ankle Spec 2010;3:10–4.
- Munuera PV, Polo J, Rebollo J. Length of the first metatarsal and hallux in hallux valgus in the initial stage. Internat Orth (SICOT) 2008;32:489–95.