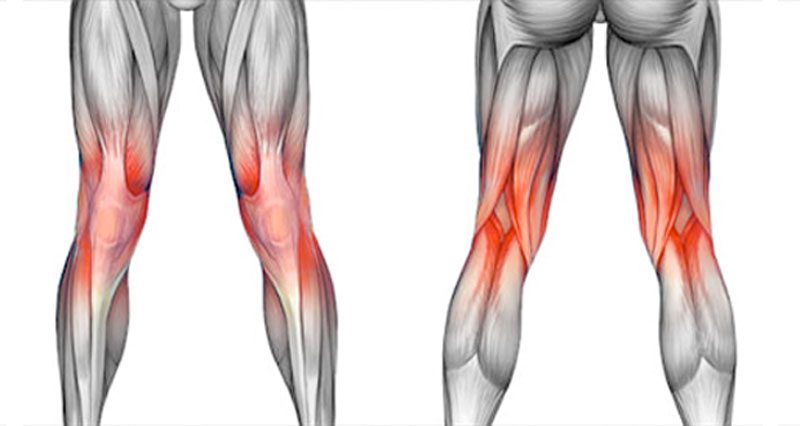
Knee pain is usually either acute or chronic. Acute knee injuries occur suddenly from direct impact or twisting and include sprains, strains and fractures. Chronic knee pain develops gradually over time, often through overuse. Common causes of gradual onset knee pain include tendinopathy (Patellar tendonitis & ITB syndrome), Patellofemoral pain, bursitis and Osgood Schlatter disease.
Medically reviewed by Dr Chaminda Goonetilleke, 10th Dec. 2021
Select the type or location of your knee pain:
- Acute knee injuries
- Outside of the knee
- Inside of the knee
- Back of the knee
- Front of the knee
- Knee rehabilitation programs
Acute knee injuries (sudden onset)
Sudden onset knee injuries involve injury to various structures of the knee, including ligaments, tendons, cartilage, and bone. Some chronic knee injuries can flare up and become acute. Here we explain the common causes of acute knee pain:
ACL sprain – a tear or rupture of the anterior cruciate ligament. It is common in contact sports and caused either by twisting or direct trauma to the knee.
MCL sprain – a tear or rupture of the medial collateral ligament on the inside of the knee.
PCL sprain – a tear or rupture of the posterior cruciate ligament in the middle of the knee.
LCL sprain – a tear or rupture of the lateral collateral ligament on the outside of the joint. Often caused by direct trauma to the inside of the knee.
Cartilage meniscus tear – injury to the semi-circular cartilage meniscus in the knee joint. Can be an acute injury, or develop through wear and tear.
Articular/hyaline cartilage injury – damage to the hard articular cartilage which protects the ends of bones.
Patella tendon rupture – a tear of the patella tendon at the front of the knee, resulting in pain just below the patella (kneecap).
Tibial plateau fracture – a fracture of the top surface of the tibia (shin) bone.
View all acute knee injuries
Lateral knee pain (outside)
Lateral knee pain refers to pain on the outside of the knee. It usually, but not always, develops gradually through overuse. The most common causes are:
LCL sprain – injury to the lateral collateral ligament on the outside of the knee. Usually, an acute knee sprain but may occur gradually over time from overuse.
Lateral cartilage meniscus tear – wear and tear or degeneration of the cartilage meniscus on the outside of the knee joint.
Iliotibial band friction syndrome – sometimes known as runner’s knee, is an overuse injury caused by repetitive friction of the tendon over the knee.
Osteoarthritis – degeneration, wear and tear of the articular cartilage and often the actual bones themselves.
View all Lateral knee pain
Medial knee pain
Pain on the inside of the knee which develops gradually over time is known as chronic knee pain. It usually results from overuse, leading to wear and tear in the joint. Alternatively, sudden onset knee injuries are caused by twisting the knee, or direct trauma. These are known as acute knee injuries.
The most common causes include:
Osteoarthritis – A major cause of medial knee pain, particularly in older athletes, is Osteoarthritis. This is degeneration or wear and tear within the joint.
Synovial plica irritation – inflammation resulting from a fold in the synovial membrane in the knee joint, often misdiagnosed as Patellofemoral pain.
Pes anserine bursitis – inflammation of a small sac of fluid called a bursa on the inside of the knee joint.
MCL sprain – injury to the medial collateral ligament on the inside of the knee. Usually an acute knee injury, but can also occur over time from overuse resulting in wear and tear.
Medial meniscus tear – degeneration of the medial cartilage meniscus on the inside of the knee.
View all medial knee pain
Posterior knee pain (back)
Some of the most common causes of gradual onset chronic pain at the back of the knee include:
Biceps femoris tendinopathy – inflammation, or more likely degeneration of the Biceps femoris tendon at the back of the knee.
Baker’s cyst – a local swelling that protrudes from the back of the knee.
Popliteus injury – is a strain of the small Popliteus muscle located at the back of the knee joint.
Hamstring tendon strain – This is a tear of one of the hamstring tendons which insert at the back of the knee (usually the Biceps femoris).
Biceps femoris avulsion – this occurs when the tendon tears pulling a small piece of bone with it.
Anterior knee (front)
This refers to the front of the knee. Injuries often involve the patella (kneecap) or the patellar tendon which connects the patella to the tibia (shin bone). The most common causes include:
Patellofemoral pain – occurs when the patella (kneecap) repeatedly rubs on the femur bone underneath.
Osgood Schlatter disease – causes pain at the front of the knee in children between the ages of 10 and 15 years old. Specifically over the bone protrusion at the top of the tibia bone.
Fat pad impingement – occurs when the infrapatellar fat pad, also sometimes known as Hoffa’s pad becomes pinched or impinged.
Patella tendonitis (Jumpers knee) – is an overuse injury causing inflammation or degeneration of the patella tendon which links the kneecap to the tibia bone.
Quadriceps tendinopathy – inflammation or degeneration of the quadriceps muscle tendon where it attaches along the top of the patella.
Knee bursitis (Housemaid’s knee) – inflammation of a small sac of fluid, called a bursa, resulting in a local swelling over the front of the patella.
View all anterior knee
Knee rehabilitation & exercises
We have the following rehabilitation programs available:
References & further reading
- Eck C, Bekerom M, Fu F et al. Methods to diagnose acute anterior cruciate ligament rupture: a meta-analysis of physical examinations with and without anaesthesia. Knee Surg Sports Traumatol Arthrosc 2013;21(8):1895–903.