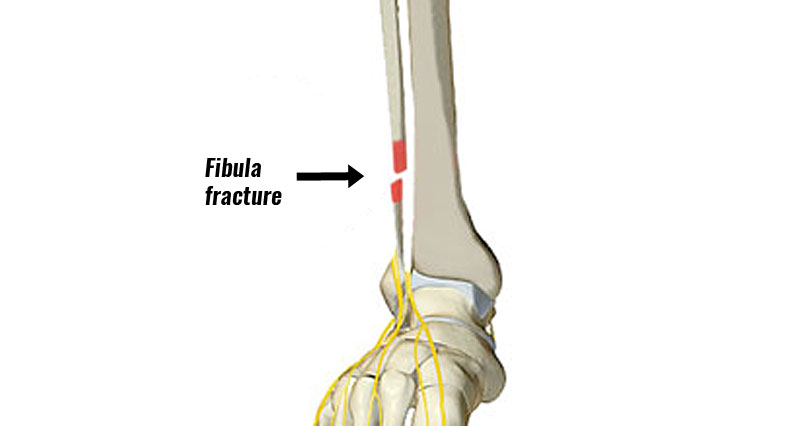
A fibula stress fracture is a small fracture or hairline crack in the bone. It is not as common as a stress fracture of the tibia. Here we explain the symptoms, causes, treatment, and rehabilitation of a stress fracture of the fibula.
Symptoms of a fibula stress fracture
- Symptoms consist of pain in the calf area with local tenderness at a point on the fibula.
- Pain will usually have developed gradually over time, rather than at a specific point in time that the athlete can recognise as when the injury occurred.
- There will be pain in the lower leg on weight-bearing although this is not as painful as a stress fracture of the tibia.
- The pain may ease off after a period of rest but get gradually worse with exercise.
Imaging
Stress fractures are unlikely to show up on an X-ray until two or three weeks into the healing process. However, a bone scan or MRI may give more information.
What is a fibula stress fracture?
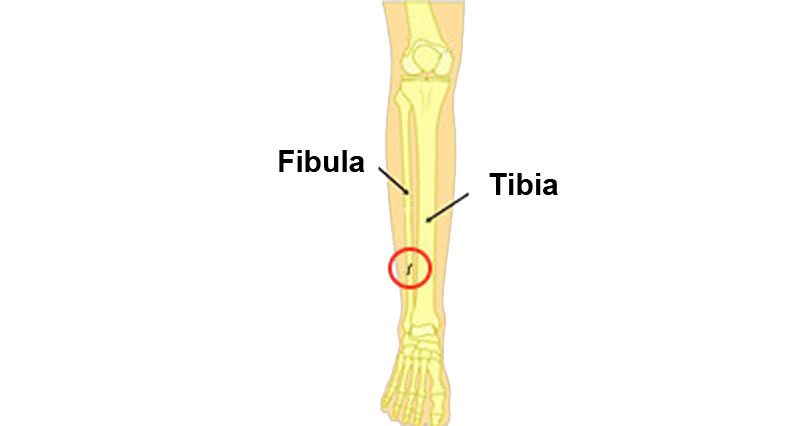
A stress fracture of the fibula is a hairline fracture in the fibula bone.
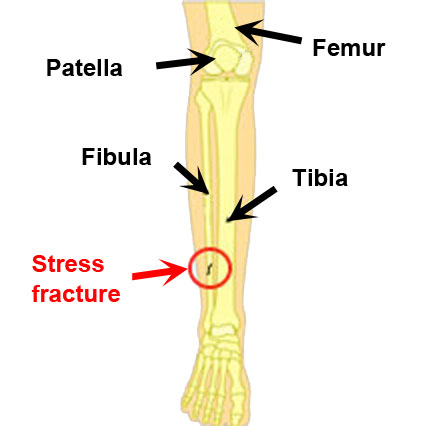
The long bones of the lower leg are the tibia and fibula. The main function of the fibula bone is as a point of attachment for many of the muscles of the lower leg.
The tibia is the thicker, weight-bearing bone of the two whereas the fibula has much of its surface for muscle attachment. This results in traction and twisting forces placed on the fibula bone from the surrounding muscles, which over time cause a stress fracture.

What causes a Fibula stress fracture?
It is primarily an overuse injury. However, there are a number of factors that can increase the likelihood of sustaining one.
- Athletes with excessive pronation (rolling in of the feet) when running are more susceptible because the peroneal muscles must work harder for longer during toe-off in the running gait cycle.
- As the arch of the foot flattens the ankle rolls inwards, twisting the lower leg and knee. The bones in the foot are not able to take the loads as efficiently as they might which places more strain on the muscles of the lower leg, many of which attach to the fibula bone.
- Overpronation and other biomechanical dysfunctions of the foot can be corrected with orthotic inserts which are placed in the patient’s shoes. They control the position of the heel and so enable normal foot biomechanics.
Treatment for a fibula stress fracture
Rest
Rest from training and competition for at least 6 weeks, or until bone tenderness has gone. Anything that works your calf muscles is unlikely to allow sufficient rest to enable healing to take place.
After the rest period, your doctor will take a further X-ray, at which point a stress fracture may show up. This is because new bone tissue has grown.
Substitute running for swimming or focus on the upper body.
Calf supports
Wear a heat retainer calf support to protect the muscles of the lower leg. This helps reduce the load on the fibula bone.
Exercises
Stretching and strengthening exercises for the lower leg should form part of a full rehabilitation program. This ensures your muscles are in good condition, strong enough, and flexible enough to cope with the demands of your sport.
Foot biomechanics
Overpronation is when your foot rolls in or flattens too much. As a result, this creates additional stress on your lower leg. Orthotic shoe inserts can correct any biomechanical dysfunction.
Training errors
Look at training methods to determine if overtraining, increasing workload too soon, or poor shoe selection is a factor. Running shoes should be good for around 400 miles or six months. After that, midsole quality deteriorates. Therefore, cushioning and support reduce.
Massage
A professional therapist may apply sports massage techniques to the muscles of the lower leg. This helps restore the condition of the muscles making them flexible and supple.
Fibula stress fracture exercises
Stretching exercises are more important than strengthening for recovering from a fibula stress fracture. The injury is primarily overused so exercising the calf muscles, especially during the rest phase is not advised.
The calf muscles consist of the larger gastrocnemius muscle and the soleus muscle which is located deeper and lower down the leg. To effectively stretch both these muscles exercises should be done with the knee bent as well as straight.
Gastrocnemius stretch

To stretch the big gastrocnemius muscle the back leg must be kept straight. Stand with the leg to be stretched at the back and hands on a wall at shoulder height. Bend the front knee and lean forward, keeping the back knee straight and pushing the heel down to the floor.
When you can feel a stretch, hold for 20 seconds. If the stretch eases, lean further forwards until you can feel it again. But do not push too far in the early stages. Perform 3 repetitions and repeat this 3-5 times a day.
Soleus stretch

To stretch the deeper soleus muscle the knee of the leg to be stretched needs to be bent. This is because the soleus muscle attaches below the knee and bending the knee allows the gastrocnemius muscle to relax leaving the soleus on the stretch.
Lean against a wall with the leg to be stretched at the back. Bend the knee keeping the heel in contact with the ground until a stretch is felt. Hold for 15 to 20 seconds and repeat three times. If a stretch is not felt then another method is to place the ball of the foot against the wall and bend the front knee until a stretch is felt.
Stretching on a step
As flexibility increases or if you have particularly flexible calf muscles it may be better to stretch using a step. Lower the heel off the step dropping down until a stretch is felt.
Hold for 15 to 20 seconds for 3 repetitions and repeat 3 to 5 times a day. The soleus muscle can be stretched similarly but with the knee of the leg to be stretched and kept bent.