Compartment syndrome occurs when the muscle swells up too big for the sheath that surrounds it. Compartment syndromes can be acute (sudden onset) or chronic (gradual onset). Here we explain the symptoms, causes and when to seek urgent medical advice.
Symptoms
An acute compartment syndrome can occur following a direct trauma or impact. Symptoms include:
- Pain in the lower leg, either in the calf muscle area or on the inside of the shin.
- You may have restricted movement at the ankle.
- If you suspect an acute compartment syndrome then seek medical attention immediately.
- This is especially true if your pain becomes gradually worse, as this can lead to long-term or permanent injury to the leg.
A chronic compartment syndrome, sometimes called a deep posterior compartment syndrome includes:
- Pain in the lower leg, specifically over the inside of the tibia (shin bone).
- It may feel similar to medial tibial stress syndrome (shin splints), or long-term, chronic calf pain.
- A chronic posterior compartment syndrome will cause deep aching pain in the lower leg.
- The pain usually comes on during a run and goes away with rest, only to return when training resumes.
- Patients often complain of a feeling of tightness or pressure.
- There may also be pain when pushing the foot and toes downwards (plantar flexing) against resistance, for example, when going up onto the toes.
- Sometimes foot drop occurs, with significant weakness in lifting the foot when walking.
Other signs
It is possible you will feel numbness or pins and needles under the foot, or lumps and bumps along the inside of the shin. This is where the muscle has begun to protrude through the sheath that surrounds it. There may be tenderness along the inside of the shin, although may not be as severe as medial tibial stress syndrome because the compartment is deeper.
Diagnosis & compartment pressure tests
To make an accurate diagnosis your doctor/physio will do compartment pressure tests for all lower leg compartments. If they suspect chronic compartment syndrome then they will perform pressure tests both before and after exercise.
The doctor inserts a needle (Stryker catheter) into the muscle compartment. It is important the patient exercises enough to bring on their symptoms. They then test compartment pressure immediately after exercise. This is to ensure the pressure testing is valid.
Approximately 10 minutes later, when symptoms have subsided your doctor will repeat the test.
What is normal compartment pressure?
Normal compartment pressures should be between 0 and 10 mmHg. One of the following indicates a chronic compartment syndrome:
- Maximum pressure of more than 25 mmHg during exercise.
- An increase in pressure of more than 10 mmHg
- Resting post-exercise pressure of more than 25 mmHg.
- The pressure should not normally take longer than 5 minutes to return to normal levels.
Often deep posterior compartment syndrome does not occur on its own. Therefore it might be missed, or confused with other shin pain causes. For instance, medial tibial stress syndrome, popliteal artery entrapment syndrome, vascular claudication, and stress fractures.
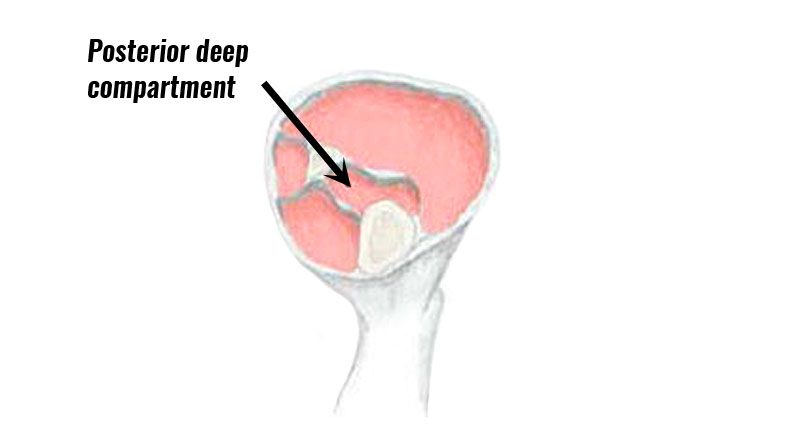
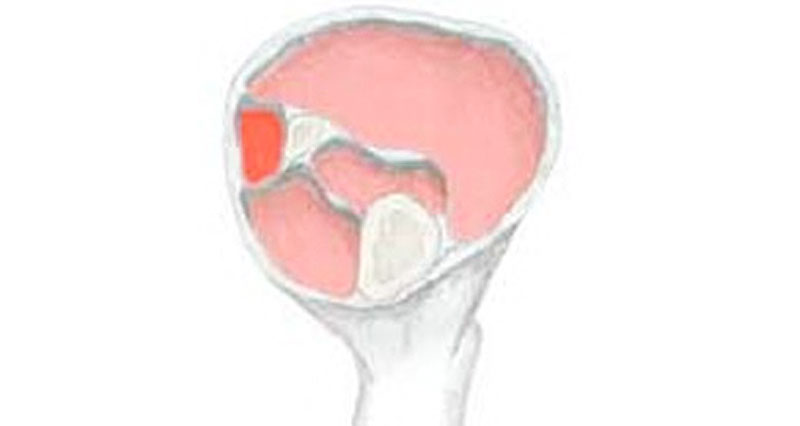
What is posterior compartment syndrome?
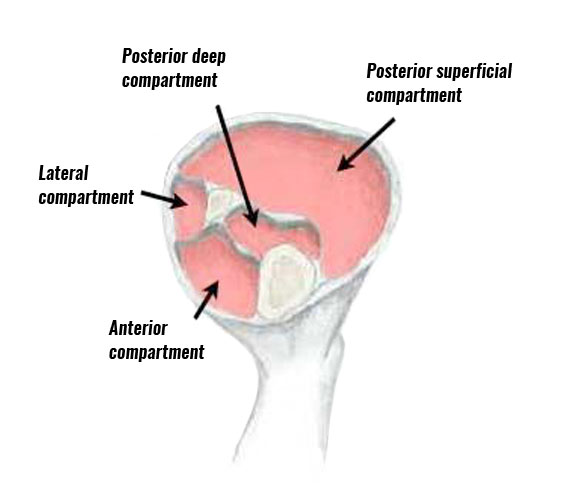
The posterior deep compartment of the lower leg is surrounded by a sheath and contains the flexor hallucis longus, the flexor digitorum longus and tibialis posterior muscles.
Occasionally in some people, an additional sheath surrounds the tibialis posterior muscle.
Acute compartment syndrome
Acute compartment syndrome is caused by impact or trauma which causes bleeding within the muscle compartment. The swelling increases pressure inside the compartment resulting in pain. A muscle strain can also bleed within a muscle compartment having the same effect.
Chronic compartment syndrome
Chronic compartment syndrome usually comes on over a longer period of time through overuse. The muscle grows too big for the compartment or sheath that surrounds it increasing pressure within the compartment and causing pain. Biomechanical factors, such as overpronation where the foot rolls in or flattens too much when running can abnormally increase the load on certain muscles making compartment syndrome more likely.
Treatment for posterior compartment syndrome
Acute injuries
Immediate medical attention should be sought for severe acute compartment syndrome as long-term damage to nerves and muscles can occur.
A doctor may prescribe anti-inflammatory medication e.g. Ibuprofen to help reduce pain and swelling and in more severe cases surgery may be indicated.
Always check with a doctor before taking medication.
Chronic compartment syndromes
Treatment for chronic compartment syndrome is rest. Simply reducing running mileage, or training load to 50% of normal may be enough.
However, switching to other forms of exercise such as cycling or swimming, or even complete rest may be needed.
Apply ice or cold therapy for up to 20 minutes at a time. Use a wet tea towel or commercially available cold packs to avoid skin burns.
Massage
Chronic compartment syndrome may respond to massage techniques which aim to stretch the sheath creating more space for the muscle.
This may include cross-friction massage techniques or myofascial release techniques which involve working the muscle along its length, whilst the foot moves into dorsiflexion (foot and toes upwards).
This should be done both passively (meaning the therapist moves the foot), and actively (meaning the patient lifts the foot).
The aim of massage is to stretch and reduce the thickness of the myofascial sheath.
Acupuncture, also known as dry needling may help reduce symptoms.
Gait analysis
Full gait analysis can be done to analyze running style and any biomechanical dysfunction of the foot, especially overpronation where the foot rolls in or flattens.
This causes the muscles of the lower leg to work harder than they might otherwise, leading to muscle growth (hypertrophy) and therefore a chronic compartment syndrome.
Overpronation can be corrected with orthotic inserts which are placed into the shoes to correct the motion of the foot, which in turn will reduce the load on certain muscles in the lower leg.
Surgery for posterior compartment syndrome
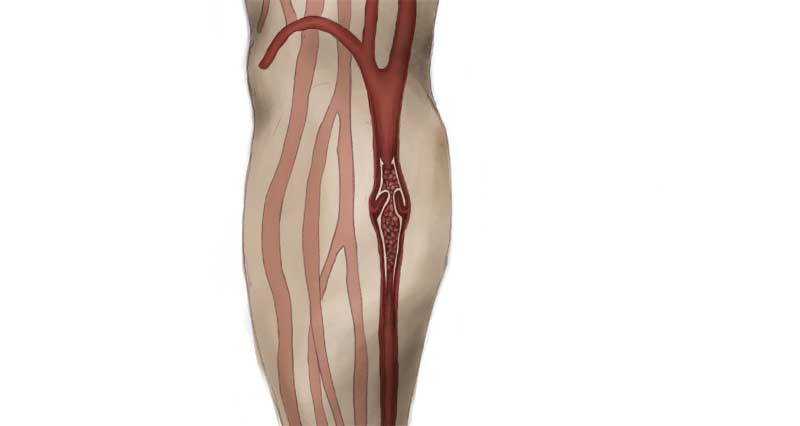
If conservative measures are unsuccessful then surgery may be required to release the pressure on the muscle. One or two small incisions are made and the sheath is cut along its length. Your surgeon will take great care not to cut the Saphenous vein which lies close to the muscle sheath as this may lead to post-surgery complications such as swelling or cellulitis.
Some surgeons may prefer to remove a part of the sheath to prevent it from reforming as it heals. Others feel the risk of further complications from removing part of the sheath means this approach is not advisable except for second operations where the first was unsuccessful. Whether other compartments in the lower leg have higher pressures will also be taken into account.
References
- Hislop M, Tierney P, Murray P et al. Chronic exertional compartment syndrome: the controversial “fifth” compartment of the leg. Am J Sports Med 2003;31(5):770-6
- Hutchinson M R, Bederka B, Kopplin M. Anatomic structures at risk during the minimal incision endoscopically assisted fascial compartment releases in the leg. Am J Sports Med 2003;31(5):764-9