Here we outline the symptoms and common causes of common injuries causing foot pain based on the specific area or location of your pain.
Medically reviewed by Dr. Chaminda Goonetilleke, 20th Jan. 2022
Select the type or location of your foot pain:
- Heel
- Arch of the foot
- Top of the foot
- Forefoot/Ball of the foot
- Outside of the foot
- Inside of the foot
- Midfoot
- Toes
- Skin conditions
- Rehabilitation programs
Heel pain
The following are common causes of heel pain:
Plantar fasciitis – is probably the most common cause of pain under the heel. Symptoms develop gradually over time, are worse first thing in the morning, and may radiate into the arch of your foot.
Bruised heel – (fat pad contusion), also known as Policeman’s heel is an overuse injury. It also has symptoms of gradual onset pain under the heel, but will not radiate into the arch of the foot.
Sever’s disease – affects children, usually between the ages of 8 and 15. It causes pain at the back of the heel which gets worse the more active the child is.
If you are not sure then try our Symptom Checker.
- View all heel injuries.
Pain in the arch of the foot
The following are common causes of foot arch pain:
Plantar fasciitis – is the most common cause of pain in the arch of the foot. Pain under the heel develops gradually, is worse in the morning, and eases as your foot warms up.
Plantar fascia strain – is a tear to the arch ligament under your foot. It can occur suddenly or may develop over time through repetitive strain.
- View all foot arch injuries
Pain on top of the foot
The following are common causes of pain on top of the foot:
Extensor tendonitis – (also known as extensor tendinopathy is the most common cause of gradual onset pain over the top of the foot. It is inflammation or more likely degeneration of the extensor tendons which run along the top of your foot. Overuse is the most likely cause.
Metatarsal stress fracture – is a hairline fracture of one of the long metatarsal bones in the foot. Pain develops gradually over time and is located towards the middle or front of your foot.
Navicular stress fracture – is a stress fracture to the navicular bone. Caused by overuse, the navicular is one of the tarsal bones found in the middle of your foot. Symptoms include a vague aching pain in the midfoot which gets worse with exercise.
Midtarsal joint sprain – is a sprain or tear of a ligament that holds the tarsal bones together in the midfoot. Symptoms will depend on which ligament is sprained, but will usually consist of pain over the outside middle of your foot. Swelling over the top of your foot is also likely.
Lisfranc’s injury – is a dislocation or fracture in the midfoot area which is rare, but can cause serious long-term complications if it goes undiagnosed.
- View all top of the foot
Forefoot pain/Ball of the foot pain
The following are common causes of forefoot pain:
Bunion – (also called Hallux valgus) is a painful swelling of the tissue on the inside of the ball of your foot. It develops gradually over time. Eventually, a deformity occurs where your big toe points inwards.
Sesamoiditis – is inflammation of the Sesamoid bones under the ball of the foot. Pain develops gradually over time and is worse when weight-bearing.
Morton’s neuroma – is caused by compression of a nerve in the forefoot resulting in pain between the third and fourth toes.
Turf toe – is a sprain of the ligament under the base of the big toe. It is caused by a sudden bending or forcing the big toe upwards.
- View all forefoot pain
Pain on the outside of the foot
The following are common causes of outside foot pain:
Peroneus Brevis tendon injury – is a strain of the peroneal tendon at the point it inserts into the outside of the forefoot (the 5th metatarsal bone).
Midtarsal Joint Sprain – causes pain in the outside of the midfoot. The exact location of pain will depend on which particular ligament is torn. You may also see swelling over the point of injury.
Jones fracture – is a fracture of the 5th metatarsal bone on the outside of the foot. It is caused by overuse or may occur from an ankle sprain
Cuboid Syndrome – occurs gradually over time. It is caused by the peroneus
- View all outside foot pain
Pain on the inside of the foot
Common causes of outside foot pain:
Bunion – is painful swelling over the inside of the big toe. It is a common cause of pain and deformity on the inside of the foot.
Navicular Stress Fracture – has symptoms of a vague ache in the midfoot, which may radiate along the inside arch of the foot.
Tibialis posterior tendinopathy – is another overuse injury, causing pain on the inside of the ankle and under the foot.
- View all inside foot
Midfoot pain
Common causes of midfoot pain:
Midtarsal joint sprain – is a sprain to any of the ligaments which hold the tarsal bones together in the midfoot area.
Stress fracture of the navicular – is also common and should not be missed.
Lisfranc joint sprain – should be considered as long-term complications will result if this is missed.
Sprained ankle – may also cause pain in the midfoot as well as the ankle.
- View all midfoot injuries
Toe pain
The following are common causes of toe pain:
Broken toe – is a fracture, or break to any of the smaller phalanges bones which make up the toe.
Dislocated toe – is an even more severe toe injury where the bones are displaced, tearing ligaments and other soft tissue as well. It may occur at the same time as a toe fracture.
Black toenail – also known as a Subungual Hematoma occurs gradually through overuse. It is more common in long-distance runners or soldiers. Eventually, the nail may fall off completely.
Ingrown toenail – occurs when the sides of your toe grow downwards into the skin. The toe will be painful, sore, and inflamed.
Hallux rigidus (stiff big toe) – causes pain and stiffness of the joint at the base of the big toe. Pain is worse when walking or running. Your toe may also appear swollen.
Hammer toe – is a deformity of the smaller toes which curl up, or bend upwards at the joint. The top of your toe may rub on your shoe, possibly causing blisters or corns.
Blisters – cause foot pain when things rub against the skin causing friction. The best cure for a blister is to prevent it from occurring in the first place, but there are some things you can do to relieve pain.
Corns & Calluses – also commonly affect the toes of sportsmen and women.
- View all
toe pain
Skin conditions
Common skin conditions affecting the foot:
Athlete’s foot – commonly causes itching between the toes.
Corns & Calluses – develop where there is pressure or thickening of the skin.
Blisters – occur anywhere on the foot but are most common between the toes and at the back of the heel.
- View all skin conditions
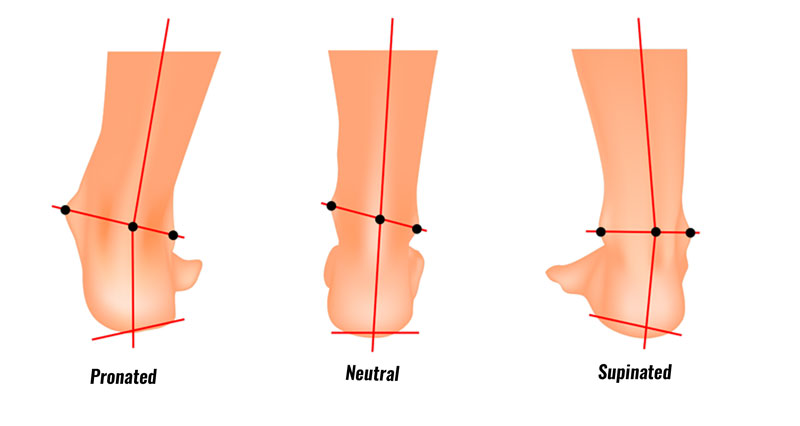
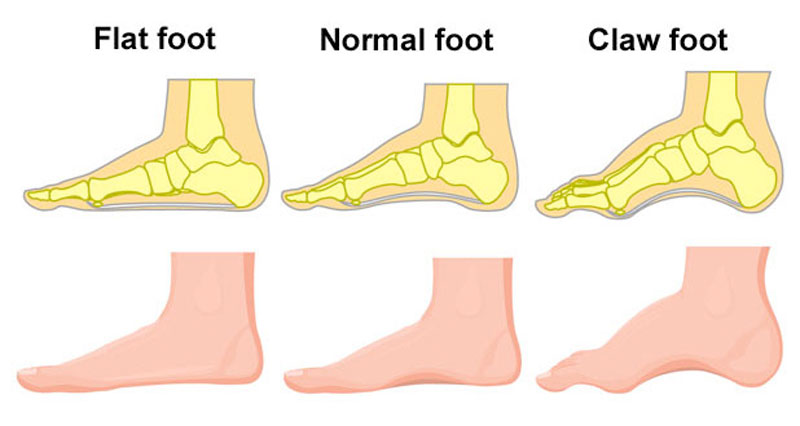
Foot biomechanics
- Overpronation – occurs when your foot rolls in or flattens too much.