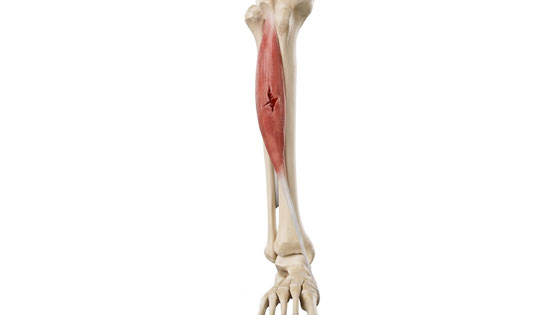
Shin Pain
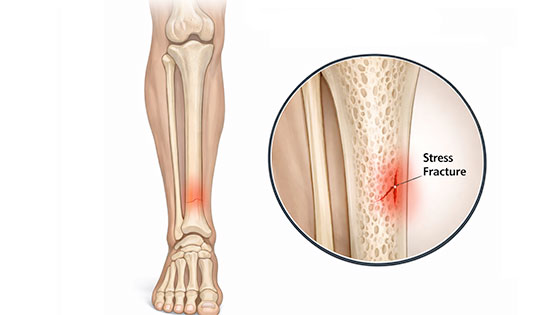
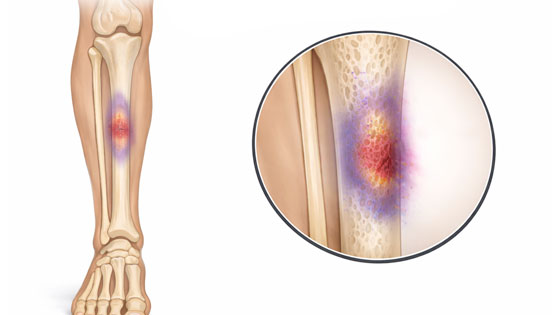
Shin pain usually (but not always) develops gradually over time and often through overuse. Shin splints is not a specific injury, but a term used to describe shin pain, of which there are many causes. These include medial tibial stress syndrome, tibial stress fracture and compartment syndromes.
Click where it hurts
Click on the lower leg go directly to specific injuries.
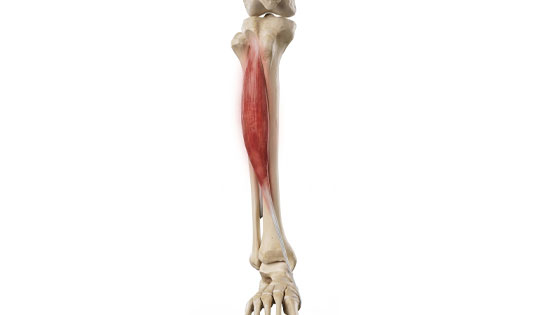
Inside of the shin (Medial Shin Pain)
Browse the most common causes of pain on the inside of the shin. The term shin splints often refers to Medial Tibial Stress Syndrome.
Outside Shin Pain
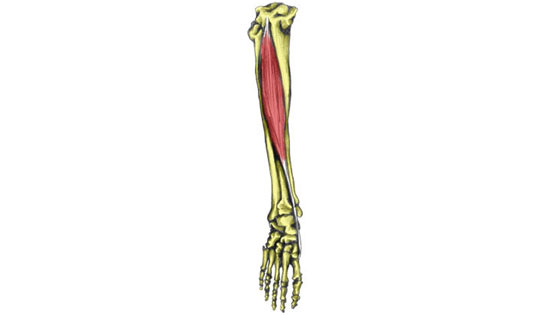
Sports injuries causing pain on the outside of the shin.
WHen SHould I See A Doctor?
It is rare that shin pain needs to be assessed by a doctor. However, an acute compartment syndrome is a medical emergency and you should seek professional advice immediately if you susect one. Or any of the following:
- Very severe pain following a direct blow or high-impact injury to the shin
- Pain that is worsening or not improving, especially if it becomes constant
- Localized, pinpoint pain on the bone, particularly if it hurts at rest or at night (possible stress fracture)
- Severe swelling, tightness, or increasing pain during exercise (possible compartment syndrome)
- Altered sensation, such as numbness, tingling, or weakness in the foot
- Difficulty walking or weight-bearing
- Long-term or recurring symptoms that do not settle with rest

Less common causes of shin pain
The following are less common causes of shin pain, but important not to miss.
Deep Vein Thrombosis
DVT (Deep Vein Thrombosis) is a blood clot in a vein, commonly seen in the calf muscle are. It is more common following surgery or long-haul flights. The main symptom is constant pain and tenderness at a point deep in the muscle. However, it is important not to miss as It is essential that a DVT is correctly diagnosed because if the blood clot comes loose, then it could find its way into the heart causing serious injury or death.
Popliteal artery entrapment
Popliteal artery entrapment is also more likely to appear as calf pain. However, pain may be felt on the outside of the shin in the anterior compartment or the big muscle on the outside of the shin.
Referred pain
This is where a problem or injury elsewhere causes pain in the shin. For example from the spine, the ankle joint, from a cyst on the knee cartilage, or from a Baker’s cyst. A Bakers cyst is a swelling behind the knee and, although this can cause symptoms, it is not particularly common.
Osgood Schlatter disease
Osgood Schlatter disease is a painful injury of the knee affecting children between the ages of 8 and 15 years old. Pain is felt on the bumpy bit at the top of the shin but may radiate down.
Pes anserine bursitis
Pes anserine bursitis is inflammation of a bursa or sack of fluid on the inside of the knee. Pain is more usually felt on the inside of the knee rather than the shin.
Other less common causes of shin pain in the athlete include:
- Femoral endarteritis
- Atherosclerotic disease
- Proximal tibiofibular subluxation
- Cramp
Important – do not miss
The following conditions rarely cause shin pain, however, a doctor or professional practitioner should be aware of them, particularly if your shin pain is persistent or not responding to conventional treatments.
- Syphilis
- Sickle-cell anemia
- Hyperparathyroidism
- Sarcoidosis
- Rickets
- Paget’s disease of the bone
- Erythema nodosum
- Infections such as osteomyelitis or cellulitis may cause pain.
Tumours of bone and soft tissue are rare, but most likely occur in athletes in their 20s and 30s. Osteosarcomata can occur at the ends of the long bones, particularly of the lower leg causing joint pain.
Immediate first aid for shin pain
Immediate treatment is to apply the P.R.I.C.E. principle (protection, rest, ice, compression & elevation).
- Protection – Prevent the shin from suffering from further damage. Stop training or playing immediately and apply cold therapy and a compression wrap.
- Rest – This is important and vital for recovery. Try to reduce the demands of your daily activity and stop doing any sports that exacerbate the pain. An athlete must know when to stop training and allow the injured area to heal otherwise repetitive minor injuries can often result in a more severe injury that keeps the athlete out for much longer.
- Ice – Apply ice or cold therapy to the painful area of the shin to help reduce the symptoms of pain and any inflammation. Apply for 10 minutes every hour initially for the first 24 to 48 hours, reducing frequency to 3 or 4 times a day as symptoms improve. Do not apply ice directly to the skin as it may burn. Either wrap ice in a wet tea towel or use a commercially available cold pack.
- Compression – The use of compression support or compression bandages on the lower leg can help reduce swelling.
- Elevation – Elevating the lower leg above heart level whenever possible to help reduce swelling due to the effects of gravity. Read more on PRICE principles
Shin Injury Rehabilitation Programs
Step-by-step thigh injury rehab programs for the following: