Eye injuries in sports are caused either by trauma or a foreign body in the eye, or infection. As with any head injury, it is advisable to seek medical advice with any injury to the eyes, especially if vision is impaired.
Black eye
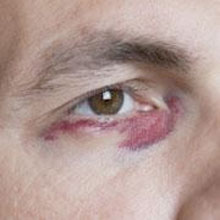
A black eye is bruising of the soft tissues surrounding the eye. Also known as an eye contusion, it usually happens following an impact or trauma to the eye.
Symptoms of a black eye include:
- Bruising and swelling around the eye
- It will be painful and tender
- It may not be possible to fully open the eye
- Vision could be impaired
Read more on Black eye.
Detached retina
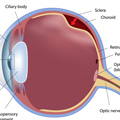
A detached retina occurs when the lining at the back of the eye starts to pull away from the blood vessels at the back of the eye. This can lead to blindness so should be treated quickly.
Symptoms include:
- The appearance of floaters within the vision
- These are dark spots which appear to drift or float in front of the eye
- Vision may be blurred
- A patient may see flashes of light in the eye or a shadow across their field of vision
Read more on Detached retina.
Corneal abrasion
A cornea abrasion is an eye injury involving scratches on the cornea of the eye. This might be from a finger, a twig or small pieces of paper or gravel blown up in the wind.
Symptoms include:
- Pain in the eye with a gritty feeling when blinking
- The patient may have the feeling of something stuck in the eye
- Watering eyes
- Visual disturbances
- Dislike of bright light is also a symptom of a cornea abrasion
Read more on Corneal abrasion.
Sty (Hordeolum)
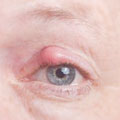
A sty which is sometimes called a hordeolum on the eye occurs when a gland on the eyelid becomes infected. This can occur on the inside or outside of the eyelid and looks like a spot or a pimple.
Symptoms of a sty
Symptoms include:
- Tenderness on the eyelid with redness and swelling
- A small head may appear on the swelling like a spot or a pimple
- Usually, appear at the base of the eyelashes
- There may be some minor visual impairment
- Styes on the inside of the eyelid feel like there is something stuck in the eye
Causes
A sty is an infection of an oil gland caused by staphylococcal bacteria. The infection usually occurs from rubbing the nose and then the eye. The bacteria involved are most often found inside the nose.
Treatment
In most cases, a sty will heal on its own within a week. Don’t ever try to squeeze a sty. They may just disappear on their own, or they may rupture and then clear. Stys on the inside of the eyelid may not heal or may be irritating in which case an ophthalmologist (eye specialist) may drain the sty for you.
Conjunctivitis
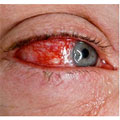
Conjunctivitis or pink eye is an inflammation of the membrane covering the white of the eyes and the underside of the eyelids. There are numerous causes of the condition which is relatively common, although not usually serious.
Symptoms include:
- The eye will have a bloodshot appearance.
- It may irritate or feel like a burning pain in the eye.
- The eyelids may be swollen and the patient could feel as if they have grit in the eye.
- Vision is likely to be impaired and a sticky discharge from the eye.
Read more on Conjunctivitis.
Foreign body in the eye
A foreign body in the eye is a small object which enters and gets stuck in the eye. This may be something which sticks to the front of the eye or gets trapped under the eyelids without actually entering the eye.
Symptoms
Symptoms of a foreign body in the eye will include:
- Pain and a gritty feeling of something stuck in the eye
- The eye will water considerably and vision is likely to be impaired
Causes
It is very common to get a small piece of grit, sand, dust or even an eyelash stuck in the eye. This happens when something is blown into the eye, for example on a windy day, or when something falls into the eye when we are looking upwards.
Objects which actually enter the eye are less common. They occur when people are hammering at something such as wood or metal and a small chip flies off and into the eye. In many cases, whilst this is a more serious injury it is not as painful.
Treatment
Rinse the eye with warm water to try to rinse out the object. Don’t stick anything (like a cotton bud etc) into the eye as this could cause further damage. If this doesn’t work or if you continue to get symptoms, consult a doctor. If you suspect that something entered your eye, seek medical attention as soon as possible.
Hyphema eye injury
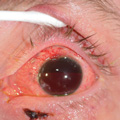
Hyphema is bleeding within the front chamber of the eye, between the iris and cornea. This is usually caused by a direct impact on the eye from a blunt object.
Symptoms of a hyphema
- Blood may be seen in the front of the eye.
- The patient will have partially, or sometimes fully, impaired vision with pain which increases as the pressure from bleeding increases
Causes
A hyphema is usually caused by an impact on the eye from a blunt object. Examples include punches to the eye, falls or being hit with a ball or other flying object.
Treatment
Seek medical attention asap. In most cases, the blood will be reabsorbed, however, to achieve this the following guidelines may be recommended by your Doctor. Rest with the head elevated and try to move as little as possible. Avoid medicines containing aspirin as this thins the blood and may increase bleeding.
Your doctor may prescribe Atropine or steroid drops. Wear an eye patch to protect the eye. The doctor will regularly check the eye for progress. You will need regular check-ups for several weeks and annual check-ups for glaucoma.