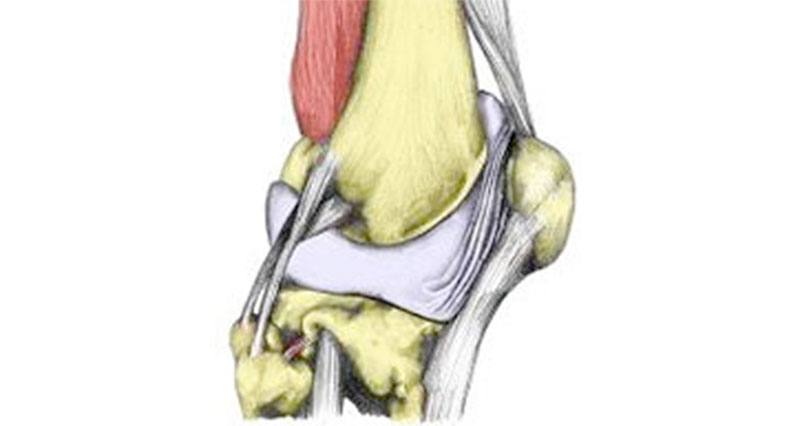
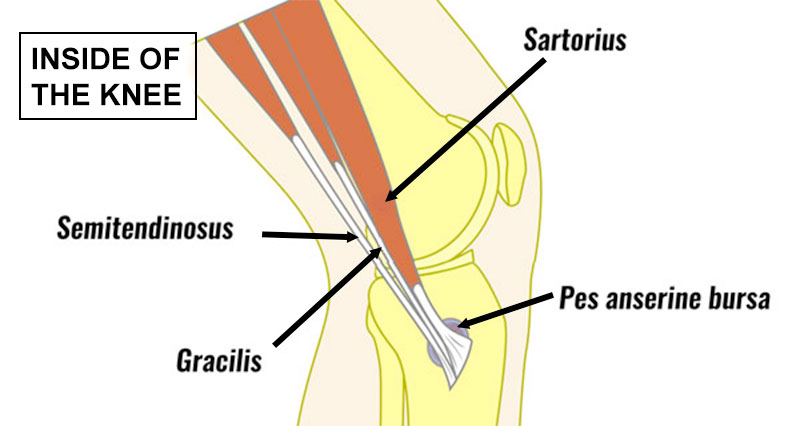
Knee bursitis is the inflammation of a small sac of fluid called a bursa. There is a number in the knee joint and their function is to lubricate movement between tendons and bone. The most common is prepatellar bursitis, also known as Housemaid’s knee.
Medically reviewed by Dr Chaminda Goonetilleke, 21st Dec. 2021
Symptoms of prepatellar bursitis
Symptoms of Housemaid’s knee include:
- Pain and tenderness at the front of the patella (kneecap) and just below it.
- Swelling over the patella.
- The swelling may feel warm to the touch.
- Kneeling is painful, hence the term housemaids knee (carpet layers knee might be more appropriate these days).
- A visible abscess or lump over the patella.
If your injury becomes chronic then there may be a tender lump floating underneath the skin on the kneecap.
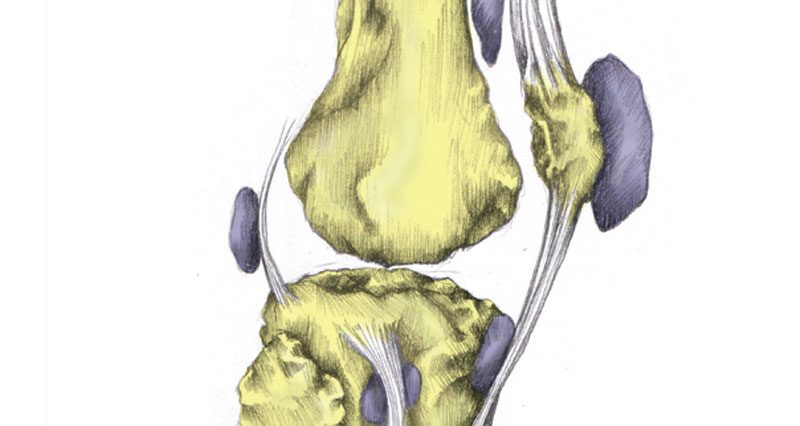
What is knee bursitis?
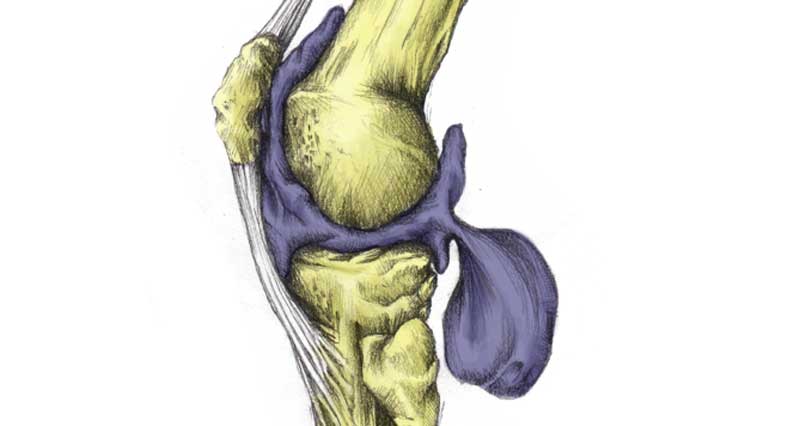
Housemaid’s Knee also known as prepatellar bursitis or knee bursitis is a swelling of the bursa or small sack of fluid at the front of the patella (kneecap). It can be acute (sudden onset) or chronic, where it occurs gradually over time.
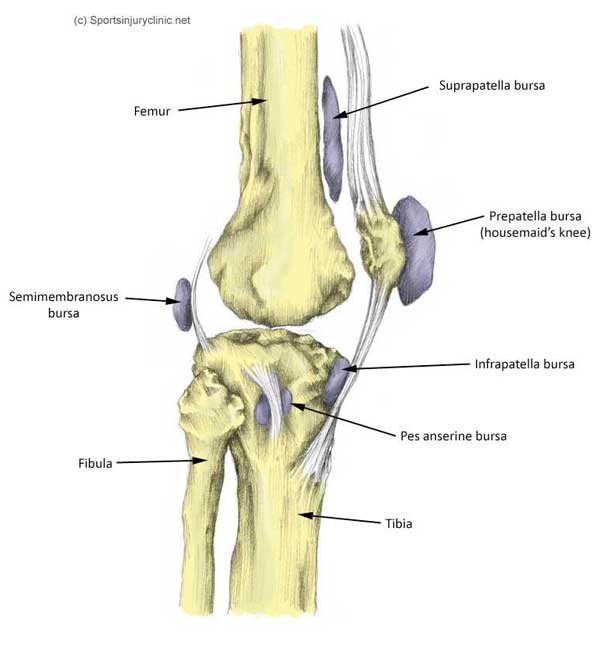
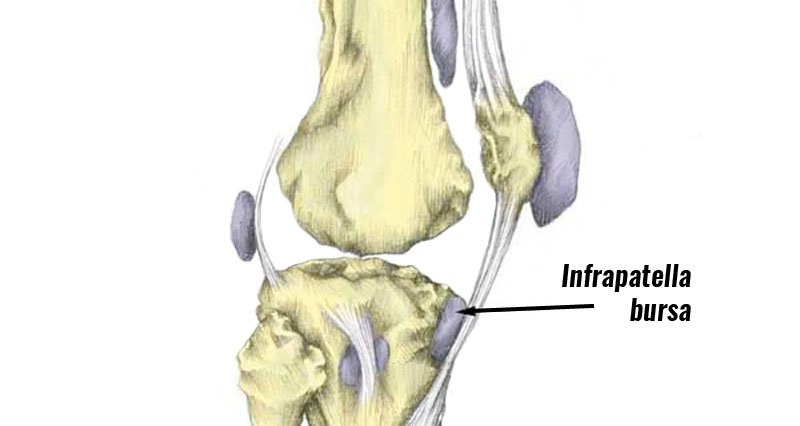
There are a number of bursas in the knee joint alone. Their function is to aid movement by lubricating movement between the tendon and bone.
Prepatellar bursitis (also known as housemaid’s knee), and Infrapatella bursitis are the most common forms of bursitis in the knee.
Causes
Bursitis can be acute (sudden onset) or chronic:
Acute knee bursitis
Acute prepatellar bursitis results from a direct blow to the knee. Or from falling on the knee. This ruptures blood vessels that bleed into the bursa, causing swelling and triggering an inflammation reaction in the walls of the bursa.
Subsequently, the walls may then thicken, causing tenderness that may remain even after the swelling has reduced.
Infection also triggers Acute knee bursitis. For example, a skin wound over the patella. In this case, bacteria spreads into the fluid within the pre-patellar bursa causing infection.
Chronic knee bursitis
Chronic bursitis is a longer-term problem that may recur over a period of time. Repeated damage to the knee, for example, from kneeling or work that involves a lot of pressure on the kneecap thickens the walls of the bursa causing irritation.
Treatment
Acute injuries
- Treat Acute prepatellar bursitis as soon as possible. Rest and apply ice or cold therapy.
- Apply ice for 10 minutes every couple of hours for the first 24 to 48 hours, especially if it is painful.
- Avoid kneeling down or applying any pressure to the knee.
- A doctor may prescribe NSAIDs or anti-inflammatory medication such as Ibuprofen. Always check with a doctor before taking medication.
Chronic injuries
- If acute bursitis does not respond to treatment or has been present for a number of days or weeks, then as with an acute case avoid any aggravating movements such as kneeling.
- Wear knee pads or padded knee supports to protect your knee.
- If the swelling persists then a medical professional may aspirate some of the fluid within the bursa. This involves sucking the fluid out with a needle and syringe.
- In cases where the bursa has become infected then antibiotics may be prescribed.
- In more serious cases then surgery may be indicated to completely remove the bursa.