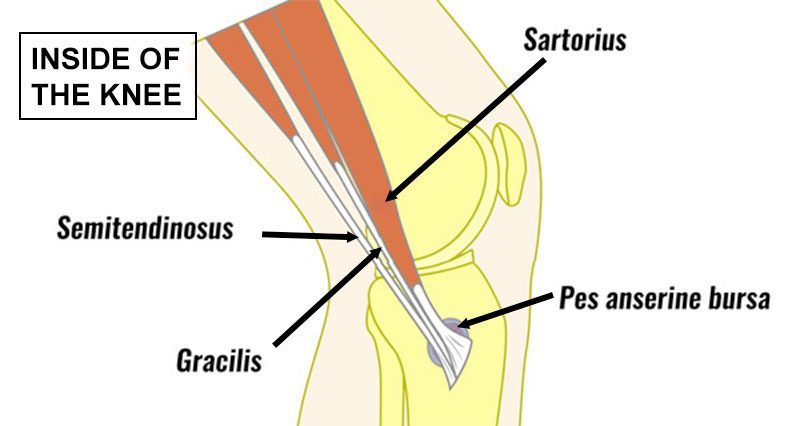
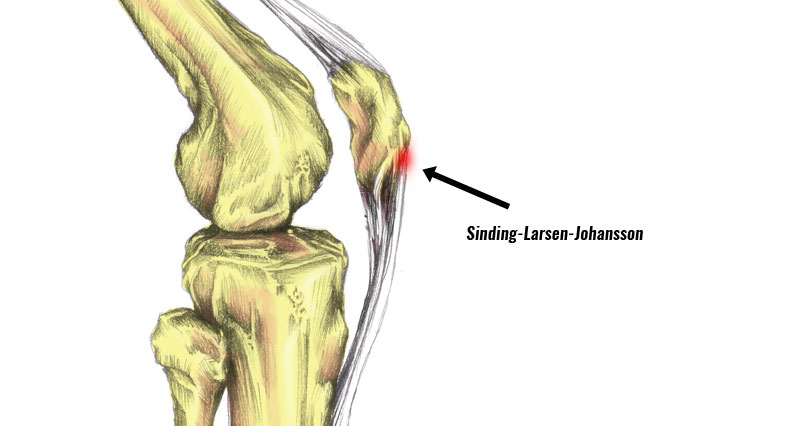
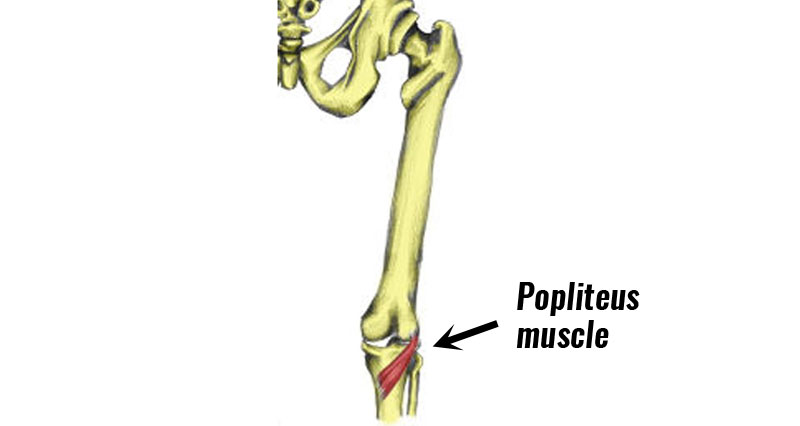
Pes anserine bursitis/tendinopathy is a less common cause of pain on the inside of the knee. A bursa is a small fluid sac that sits under the tendon. Either the tendon, bursa, or both may become inflamed.
Medically reviewed by Dr Chaminda Goonetilleke, 21st Dec. 2021
Symptoms of pes anserine bursitis/tendinopathy
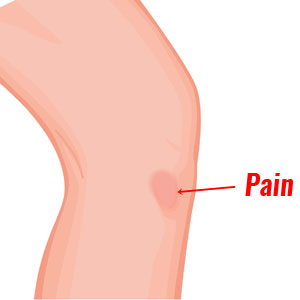
Both pes anserine bursitis and tendinopathy have symptoms very similar to a medial ligament injury and include:
- Pain over the inside of your knee, particularly the lower part.
- Symptoms are usually located specifically at a point three fingers below the joint line on the inside of the knee.
- You may feel pain climbing stairs.
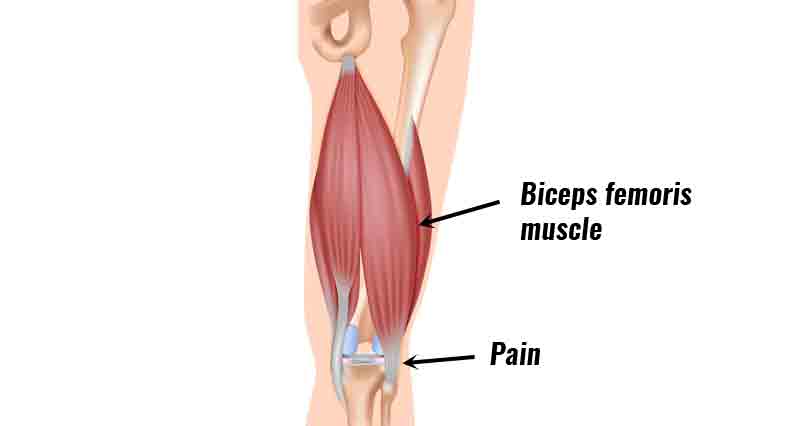
- Stretching the hamstring muscles, or attempting to contract them against resistance may also reproduce pain.
Other injuries with similar symptoms include:
Medial ligament sprain – this is a tear to the ligament on the inside of the knee.
Medial cartilage meniscus injury – this is damage to the semi-circular-shaped cartilage which provides support and cushioning to the knee joint.
Stress fracture of the tibia – a hairline crack in the tibia bone at the knee caused by repetitive strain and overuse.
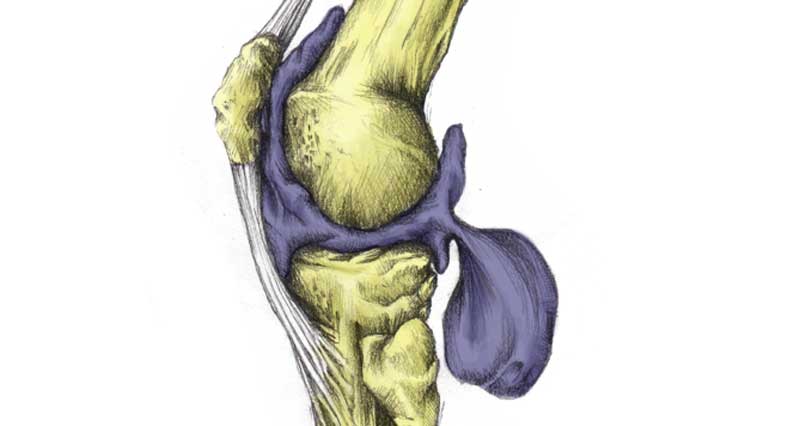
Pes anserine bursitis causes & anatomy
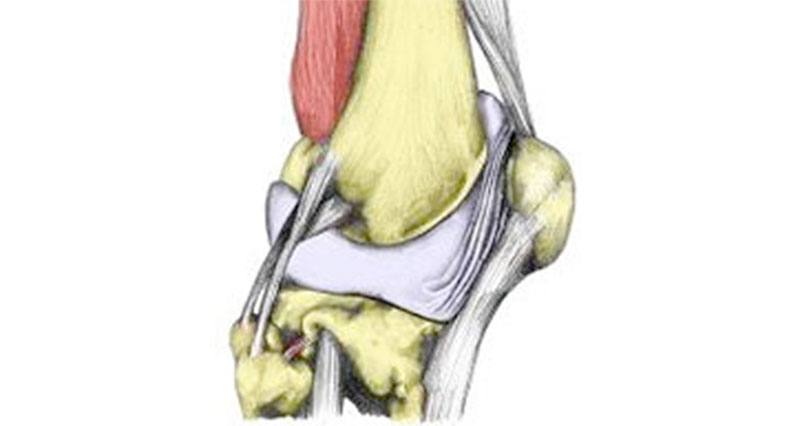
The Pes Anserine, also known as pes anserinus or the goose’s foot is the combined tendon of the semitendinosus muscle (one of the hamstrings), Sartorius and gracilis.
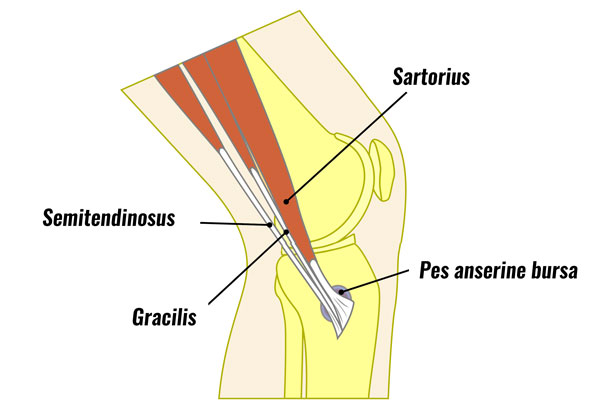
Each of the three muscles is supplied by a different nerve:
- Sartorius = femoral nerve
- Gracilis = obturator nerve
- Semitendinosus = tibial nerve.
They all attach together to the tibia (shin bone) on the inner part of the lower knee. The main function of the three muscles is to assist in flexing (bending) your knee. However, they also help stabilise the knee by helping the medical ligament resist valgus (sideways) forces.
Bursitis
In this area, there is also a bursa, called the anserine bursa. It lies between the combined tendon and the Tibia. The bursa becomes inflamed due to repetitive friction. It is more common in sports such as cycling, running, and swimming, especially breaststroke.
This results in bursitis and/or tendinopathy (sometimes called tendonitis). Any sport or activity which puts repeated stress on the inside of the knee puts you at risk of pes anserine bursitis or tendon injury.
Tendonitis or tendinopathy?
The word tendinopathy is probably a more accurate term as it describes the degeneration of the tendon rather than specific acute inflammation. Tendonitis refers to acute inflammation (itis means inflammation).
With long-term, overuse injuries, it is more likely to be degeneration. This is because studies have shown that acute inflammatory cells are not usually present.
Treatment of pes anserine tendinopathy
The aim of treatment is to treat the symptoms of pain and inflammation, as well as identify and correct any potential causes of the tendon or bursa inflammation.
What can the athlete do?
Rest and apply the PRICE principles of rest, ice, compression, and elevation. Rest from any aggravating activities. Apply ice or cold therapy to reduce pain and inflammation.
Ice can be applied for 10 minutes every hour initially for the first 24 to 48 hours reducing to 3 or 4 times a day as required.
What can a sports injury professional do?
A doctor may prescribe anti-inflammatory medication such as ibuprofen which may help reduce pain and inflammation. Stretching the surrounding muscles such as the quadriceps, hamstrings, and adductor muscles may help.
A therapist may apply electrotherapy such as ultrasound and if treatment is not successful then corticosteroid injections have been shown to be effective.
Identifying causes of pes anserine bursitis
The second phase of treatment should be to consider what may have caused the injury and to correct the problem. It may be something as simple as having tight hamstring muscles and in which case these should be stretched regularly and sports massage applied to improve elasticity.
Other common causes include obesity and overpronation of the foot where the foot flattens or rolls in too much when running. This, in turn, causes the lower leg to rotate inwards which may also increase the valgus forces on the inside of the knee causing a valgus knee deformity where the knee falls or bows inwards.
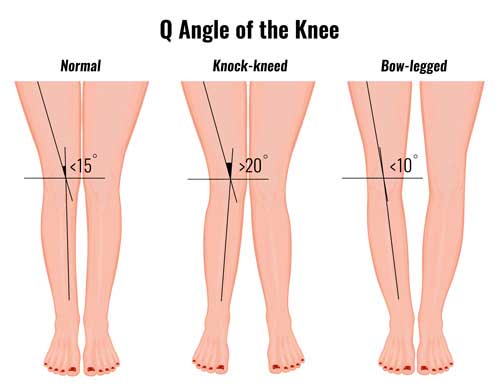
The Q angle of the knee is a measurement of valgus knee deformity.
Wearing a knee brace or support with additional protection at the sides may help. A hinged knee brace has solid metal down the sides and provides the most support. A stabilized brace has flat springs inserted into the sides to provide additional support but may allow more movement than a hinged knee brace.
References
- Rennie WJ, Saifuddin A. Pes anserine bursitis: incidence in symptomatic knees and clinical presentation. Skeletal Radiol 2005;34(7):395–8.
- Alvarez-Nemegyei J. Risk factors for pes anserinus tendinitis/ bursitis syndrome: a case-control study. J Clin Rheumatol 2007;13(2):63-5.