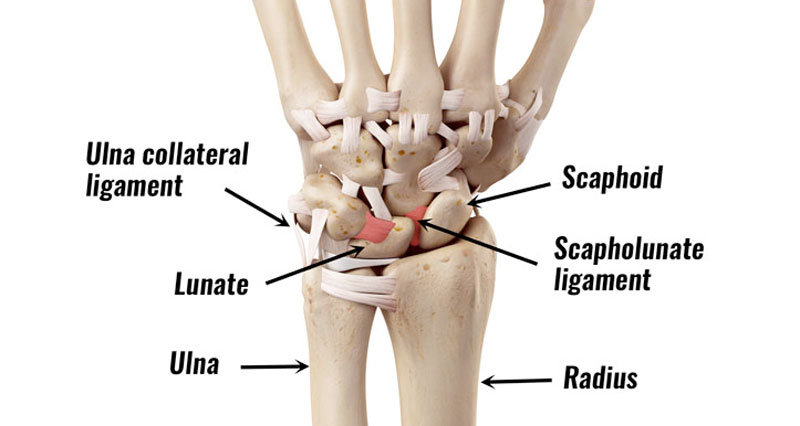
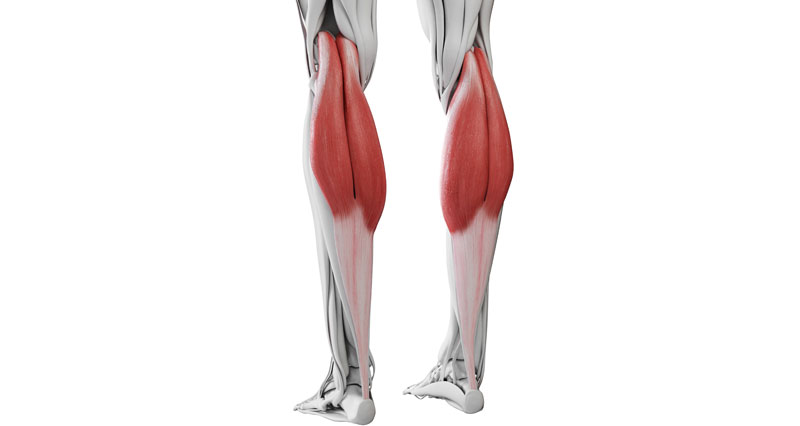
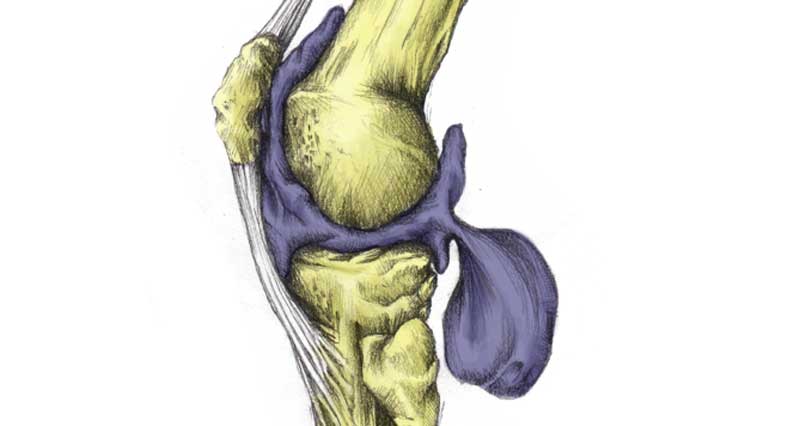
Tennis leg is a general term used to describe pain in the leg caused by a tear of the inner head of the big calf muscle, the plantaris muscle or sometimes both.
Tennis leg symptoms
Typical symptoms of tennis leg are a sudden onset of pain in the back of the knee or calf muscle. The ability to move the ankle will be affected. The athlete may experience pain and weakness when trying to stand on tiptoes. Bruising and swelling at the back of the leg are common. This injury can sometimes be mistaken for a deep vein thrombosis
What is tennis leg?
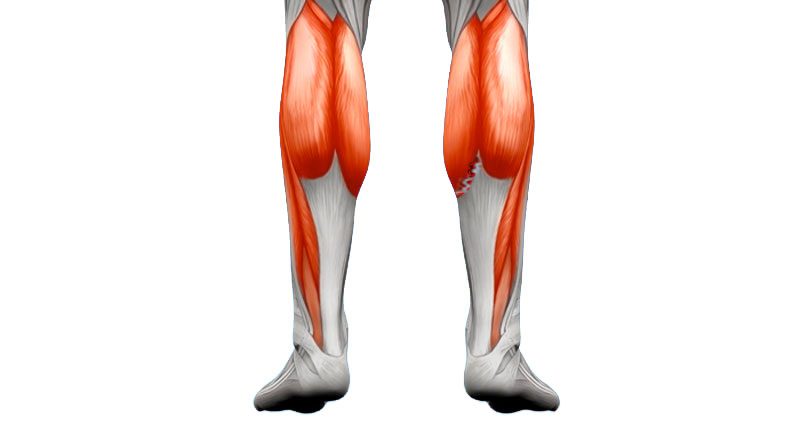
Tennis leg is a tear or rupture of the plantaris muscle and possibly the medial head or inside of the gastrocnemius muscle which is the larger of the two calf muscles.
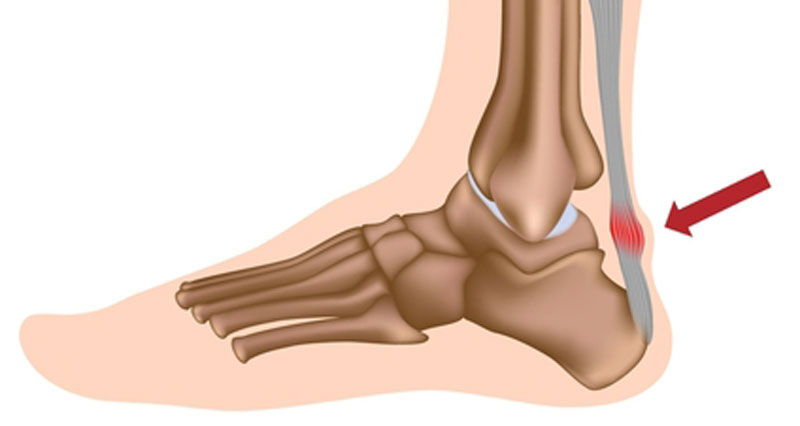
The Plantaris muscle is a thin muscle in the back of the lower leg, which attaches just above the knee on the outside, passes down the back of the calf and inserts on to the heel bone. Its function is to assist the larger calf muscles in plantar flexing the ankle or pointing the foot down. This muscle is actually absent in up to 15% of the population.
The injury most frequently occurs due to a force or trauma to the leg whilst the knee is straight. Movements such as jumping or pushing off may also cause tennis leg. Both movements are frequent in tennis, hence the development of the term tennis leg to describe this injury.
Buy Knee Braces
Treatment for tennis leg
Treatment of a tennis leg injury should be the same as for any muscle strain with the principles of PRICE or protection, rest, ice, compression and elevation being followed.
Ice should be applied as soon as possible after the injury and continued for 10 to 15 minutes every hour initially during the acute stage which is likely to be the first 24 to 48 hours. Frequency can be reduced as symptoms lessen and any swelling goes down. Compression in the form of an elastic support bandage or knee support with protect the joint and help reduce swelling.

Buy Kinesiology Tape
If it is painful to walk then crutches may be beneficial as partial weight bearing is recommended. Full weight bearing and walking normally should be done as soon as pain allows.

Mobility exercises and gentle calf stretching may be performed after the first day or two provided they can be done pain-free. As soon as normal walking is pain-free then strengthening exercises should begin. Initially resistance band plantar flexion exercises should be done to very gradually introduce some load onto the calf and plantaris muscles. As strength improves calf raise exercises can be introduced until single leg calf raise exercises and more functional sports specific rehab exercises can be performed.