Medical image methods explained, including MRI, X-rays, and Bones Scans.
Bone Scans
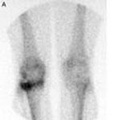
A bone scan is also known as a Radio Isotopic bone scan. A radioactive tracer is injected into the bloodstream. This passes through the bones and other tissues. As the tracer wears off it gives off radiation which is detected by a camera. A scan may be taken immediately or after 3-4 hours or both. Bones scans are helpful in diagnosing:
- Stress fractures.
- Osteochondral lesions.
- Identify bone tumours or cancers.
- Diagnose bone infections.
- Determine the cause of bone pain when no other cause has been found.
- Diagnose bone conditions such as Paget’s disease.
Read more on Bones scans.
EMG
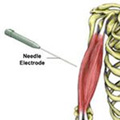
An electromyography (abbreviated to EMG) is a device used to measure and detect muscle conditions. It uses needle electrodes to discover information about the muscles.
What is EMG?
EMG is most commonly used to detect muscle conditions such as Muscular Dystrophy, diseases of the neuromuscular junction (between the nerve and muscle), and nerve or nerve root injuries.
In a very simplistic overview, information is sent along nerves as an electrical impulse. When the impulse reaches a muscle, this triggers an action potential that passes through the muscle, causing the fibres to contract. The muscle membrane potential is measured, as is the rate of motor unit firing. An EMG may be performed alongside a nerve conduction study to get a full picture of the muscle/nerve injury.
What happens when you go for an EMG?
The machine used for EMG is an electromyograph. The process involves inserting needle electrodes into the muscle and so, for this reason, the test can be a little uncomfortable, although is not usually painful. The muscle may also feel tender or bruised the next day.
The number of needles depends on the size of the muscle being tested. Once the needles are inserted the patient is asked to make some small movements to fire the nerve and contract the muscle(s) in question. The information picked up by the needles is transmitted to an amplifier which is connected to a device that produces a readout. This can then be printed or displayed on a computer screen.
The size and shape of the waves produced, provide the information required about the ability of the muscle and nerves involved.
There are very few risks involved with EMG so it is very safe to perform. The only risks are from minor internal bleeding due to the insertion of the needles, as well as an extremely low risk of infection (all needles are new, sterile, and sealed before the test and are discarded after use).
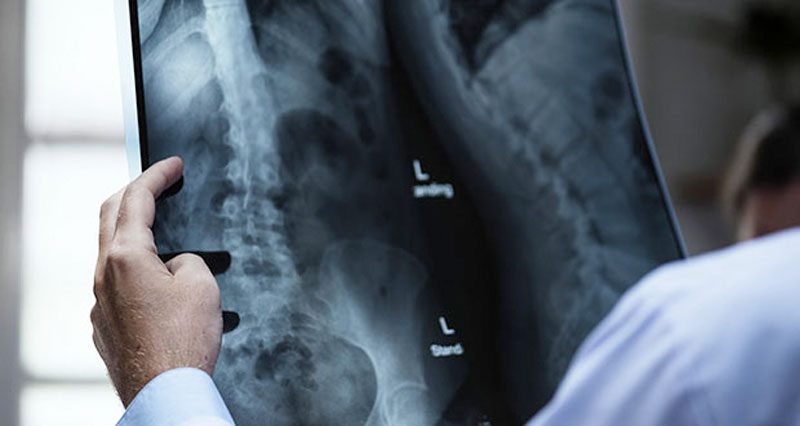
X-rays
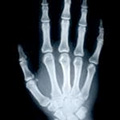
X-rays were first discovered in 1895 by a Physicist named Roentgen. X-rays are the same wave-like electromagnetic energy form as visible light rays, however, x-rays have a shorter wavelength which is not visible to the naked eye.
What are X-rays?
X-rays can be used to view structures within the body because of their ability to pass through our tissues. The more dense tissues such as bone appear white on an x-ray film because they block more of the rays. Soft tissues allow more rays to pass through and so appear darker. The lungs appear black as they are mostly air. When there is a break in a bone, more rays escape through the interruption in the bone, showing up as a darkened line. When x-raying for conditions, such as a lung tumour, this will appear as a lighter patch within the black lungs.
What happens when you go for an X-Ray?
Before having an x-ray the patient must remove all jewellery and other metal and females should be asked if they are pregnant as x-rays may harm the baby.
Most x-ray machines consist of an x-ray tube suspended over the table on which the patient lies. The x-ray film onto which the image is recorded is located under the table. Many x-ray machines are now digital and the images are stored directly onto a computer, rather than printed onto a film.
In order to protect you from radiation, a lead apron may be placed over areas that are not being scanned. The Radiologist will also wear one.
You will be asked to stay very still and may be given pillows to position yourself more easily to get the required view. The Radiologist will either leave the room or stand behind a screen whilst taking the x-rays. You may have two or more taken, in varying positions, to allow for a comprehensive view of the injury.
What are the risks?
X-rays are a very low-risk procedure, although not as low-risk as an MRI scan. Because of the radiation, there is always a very small chance of developing cancer from excessive exposure to x-rays. However, every single x-ray exposes the patient to 20 milliroentgens of radiation. Each year we are exposed to over 100 milliroentgens of radiation, mainly from the sun, so really the risk is minimal.
Electrocardiogram (ECG)
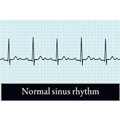
An Electrocardiogram (abbreviated to ECG) is a device used to measure the electrical activity of the heart. This can be useful in identifying heart problems.
What is an Electrocardiogram?
The heart contracts due to tiny electrical impulses spread throughout the heart muscle by the Sinoatrial (SA) node (the heart’s own, natural pacemaker).
An electrocardiogram detects and records these impulses. ECGs are used when a heart or circulatory system condition is suspected. Often it is one of the first tests to be conducted when a patient complains of chest pains or palpitations. An ECG may also be performed as a routine test before an operation, for example.
What Does an ECG Show?
Different conditions produce different abnormal patterns. Conditions that can be detected include:
- Coronary Heart Disease/Angina
- A heart attack. The scan can also indicate how long ago the attack was through the damage to the heart muscle and scar tissue present.
- Coronary Artery Disease
- An enlarged heart
- Abnormal heart rhythms
- The effectiveness of heart medications
What Happens During an ECG?
Adhesive electrodes are placed on the skin over the chest, arms, and even the legs. Up to 12 electrodes can be used and the skin may need to be shaved first to make sure the electrodes stick properly.
The actual test takes only around a minute to perform once all of the electrodes are in place. The results are then printed out for the Doctor to review.
In most cases, the ECG is performed at rest. In a few cases, it may be performed when the patient is exercising on a treadmill or stationary cycle. This is done when coronary artery disease is suspected and is known as an exercise stress test.
Is It Safe?
Yes! At rest, an ECG is completely safe and pain-free. An exercise stress test carries a slightly higher risk and the patient may suffer chest pain when exercising which should clear once they stop. A Doctor is always present alongside the ECG technicians and will stop the testing if there is significant chest pain or if the readings on the ECG change.
Echocardiogram
An Echocardiogram is a test used to look at the structure and function of the heart. It uses ultrasound waves to display a moving image of the heart, similar to that used to look at unborn babies.
The ultrasound waves emitted are of a very high frequency and cannot be heard by human ears. The waves are bounced back to the machine by the structures they come into contact with. Denser structures (such as the heart valves) echo more waves back than less dense materials and fluids. This helps to build up a picture of the heart. It is also possible to see the heart moving as the image is constantly updated.
Echocardiograms are used to look at the heart to check the way it is working and that it is not damaged. It can be used to look at the heart’s muscle tissue, the chambers of the heart, and also the valves which control the blood flow into and out of the heart.
An ‘Echo’ may be used after a heart attack to see how much damage has occurred, and also if a heart condition is suspected.
Echocardiograms can be used in adults, children, and babies. They can also be performed on unborn babies. This is called a fetal echocardiogram.
What Happens During An Echocardiogram?
Echocardiograms take place in a hospital. You will not need to do anything special to prepare for your echo.
In the appointment, the patient is asked to undress down to their waist. Lubricating jelly is used on the chest so that the ultrasound probe glides smoothly and makes good contact with the skin. The probe is attached via a wire to the ultrasound machine and the waves are passed down and fed back to the machine this way.
The test will take up to half an hour and is completely painless and carries no risks to the patient.
In a few cases, the consultant may wish to look at the heart during exercise. This is known as a stress echocardiogram. If a very detailed view of the heart is required, then a Transoesophageal echocardiogram may be used. This involves the patient swallowing a small probe attached to a long wire so that the heart can be viewed from within the oesophagus.
Bone Density Tests
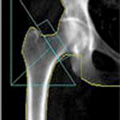
Bone density testing is used to diagnose Osteoporosis. It is also called Bone Densitometry or Dual-Energy X-ray Absorptiometry (DXA).
What is bone density testing?
Bone density scanning is a special form of X-ray which is used to measure bone loss. It can be used to diagnose Osteoporosis, but also to measure the effectiveness of subsequent treatments in delaying the progression of the disease.
Bone density tests are usually carried out on the lower spine, pelvis, or thigh bones. It is recommended that women over the age of 50 (who are not taking Oestrogen) go for a bone density scan. This is especially important if you have a family history of Osteoporosis. Other medical conditions or medications may also increase your risk:
- Diabetes (especially type 1 – juvenile/insulin-dependent diabetes)
- Liver or kidney disease.
- Thyroid conditions.
- Prolonged use of Corticosteroids.
- Anti-seizure medication.
How does bone density testing work?
The DXA machine transmits an invisible low-dose X-ray beam with two clear energy peaks through the bones being tested. One of the peaks is absorbed by soft tissues whilst the other is absorbed by bone.
The amount absorbed by soft tissue can be subtracted from the total, with the remainder being the patient’s bone mineral density. The measurements are computed and displayed on a monitor.
DXA machines can either be large stationary objects in a hospital or can be small, portable boxes. Those in a hospital consist of a couch with a moveable arm that scans the body area. The portable versions are used for smaller body parts that can be placed inside the device.
Results
The results are interpreted by a radiologist who will usually send a report to your Doctor.
The readings are given 2 scores, a T score, and a Z score. The T score compares your readings to that of someone of the same sex with optimal bone density. If your score is -1 or less then this is considered normal. Scores between -1 & -2.5 are classed as Osteopenia low bone mass). A diagnosis of Osteoporosis is given if the results are greater than -2.5.
The Z score compares your results to those of a person of the same sex and age who has normal bone density. A very high or low score may require further investigation.
CT Scan
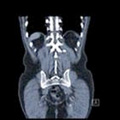
A CT scan (or cat scan) is an abbreviation of Computerised Tomography. CT scans show cross-sectional images of soft tissues (muscles, tendons, ligaments, cartilage, etc) as well as bone and calcific deposits.
What is a CT scan?
A CT scanner is a special type of X-ray that uses multiple beams, rather than just the singular one seen in X-rays. The scanner rotates around the patient to give a clearer view of what is happening internally. The beam passes through the body part being scanned and the strength of the beam on the other side is measured. In dense tissue such as bone, the strength of the beam received is less and so it appears white on the film. Less tense tissue (soft tissues) appears less clearly, as a pale shadow.
CT scans are far more detailed than X-rays. Whilst a 2D image is produced by older machines, newer technology has allowed for 3D images.
What is a CT Scan used for?
CT scanners were originally used for imaging the brain, but now they are used for just about any part of the body. They are especially good at picking up tumours, bleeding in the brain, aneurysms, lung disease, and internal injuries such as lacerations of the kidneys or spleen.
They are also used for bony injuries, especially in the spine. You may be offered a CT scan for suspected small fractures in complex regions such as the ankle, foot, or pelvis.
What happens during a scan?
If the scan is of the abdomen, you may be asked not to eat anything for 6 hours. You may also be given a special drink that contains an X-ray dye to help make your intestines clearer on the scan. For other areas, you may be injected with a dye.
The CT scanner looks like a round tunnel. The patient (or just the body part being scanned) is moved backwards and forwards within the tunnel until all necessary pictures and angles are taken.
Whilst a CT scan is safe and the patient is not at any risk, the multiple X-rays and exposure to radiation, mean that a CT scan should only be requested for good reason and should not be undertaken repeatedly.
MRI Scans
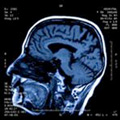
MRI stands for Magnetic Resonance Imaging. MRI scans were introduced in the 1980s and are now used frequently in the diagnosis of soft tissue injuries and other medical conditions.
What are MRI scans?
Unlike X-rays which only show bone, MRI scans show all tissues within the body, including bones, muscles, cartilage, and fatty tissue. They are especially useful for viewing soft tissue which is enclosed or surrounded by bone, such as the brain and spinal cord. MRIs produce far more detailed pictures than x-rays or CT scans and so they are often used for detecting conditions such as brain tumours, strokes, and heart defects. Sports injuries such as meniscus tears, ACL ruptures, and labrum tears are often scanned by MRI to confirm the diagnosis prior to surgery.
What happens when you go for your scan?
MRI scans are performed in hospitals, usually on an outpatient basis. When you arrive, all of the necessary paperwork must be completed and your radiographer should explain the procedure to you. You will then be asked to change into a hospital gown and remove all jewellery hearing aids and make-up etc.
Depending on the reason for your scan, a dye may be required to highlight some tissues. This will be injected into a vein in your arm or hand and will be safely removed from your system via your urine over the next 24 hours.
The scanner itself is a cylindrical-shaped, open-ended machine, which you lay on your back. The machine itself is quite noisy whilst the scan is being taken and so you may be asked to wear earplugs or headphones. The radiographer will be in a separate room, but will always be able to see you inside the scanner. You will be given an alarm which you can press at any time throughout the scan if you need assistance.
Throughout the scan, you will be asked to stay as still as possible and breathe very gently. It can take several minutes to take even one image and so the time your scan takes depends upon the number of images to be taken.
After the scan, you can normally go straight home and the results will be sent to the Doctor who requested them on your behalf.
How do they actually work?
MRIs use magnetic fields and radio waves to produce an image of your body. These are not harmful, unlike X-rays. Passing these strong waves through the body affects the atoms within the body. The nuclei within each atom are forced into a different position, and when it returns to its normal position this produces a second radio wave. The machine picks this up and translates the information into an image. The image produced is due to the position and strength of these radio waves.
All of the tissues within our bodies contain water (H20) and water contains Hydrogen (H2). The Hydrogen atoms have a large part to play in how the image appears. Those structures with a high proportion of hydrogen atoms appear much brighter than those with a lower proportion. For this reason, fatty tissue appears much brighter than bone.
Nerve Conduction Studies
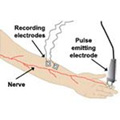
Nerve conduction studies are often run at the same time as an EMG.
What are nerve conduction studies?
A nerve conduction test gives doctors information about any potential problems with your peripheral nervous system (i.e. the nerves outside of the brain and spinal cord).
The brain sends an electrical impulse down the spinal cord and then along the peripheral nerves. This electrical impulse then either causes a muscle to contract (motor nerves) or is used to detect things like pressure and heat (sensory nerves). If a nerve is damaged, then the electrical impulse may travel slower down the nerve and the signal may not be as strong.
What are they used for?
Nerve conduction studies are used when nerve damage is suspected. This may be due to:
- Injury (such as fractures or lacerations).
- Conditions such as Diabetes.
- Trapped nerves (e.g. this is common in the neck or conditions such as carpal tunnel syndrome).
- Neuropathies.
Nerve conduction studies can differentiate between damage to the myelin sheath of the nerve (surrounding fatty coating) or damage to the axon (central portion) of the nerve. This is due to the myelin sheath being an insulator of the impulse and so damage to this part of the nerve causes a significant decrease in the nerve conduction velocity. If an impulse is considerably slower than normal, damage to the myelin sheath is present. If the nerve’s response is decreased but at a normal speed, then damage to the nerve axon is present.
What happens during the test?
Electrodes are attached to the skin using tape, velcro, or a special paste. One of these is a pulse-emitting electrode that is positioned directly over the nerve which is being tested. Recording electrodes are then positioned over the muscle(s) that the nerve supplies.
A series of electrical impulses stimulate the nerve (from the pulse-emitting electrode). The time between these impulses and muscle contracting is recorded. The strength of the contraction is also registered by the recording electrodes over the muscle. If a sensory nerve is being tested, the recording electrode is placed on the nerve and records the time for the impulse to be returned back towards the brain.
The electrical impulses are not painful but feel like tiny shock-like tapping sensations which may be uncomfortable. Testing may take just a few minutes if only one nerve is being tested. For a lot of nerves, the tests may take a lot longer. For comparison purposes, the same nerves may be tested on the other side of the body.
Diagnostic Ultrasound Scan
An ultrasound scan is a way of looking at soft tissues within the body, using sound waves rather than radiation and so it is thought to be safer than other imaging methods.
What is ultrasound?
The sound waves used are at an extremely high frequency and so they cannot be heard. The waves are passed into the tissues and travel through soft tissues. When they hit something denser (such as bone), the waves are reflected back. The strength and frequency of the waves being ‘echoed’ back determine the density of the underlying tissue.
The sound waves are transmitted into an image that is shown on a computer screen. This is different from therapeutic ultrasound where no image is produced and the main aim of the procedure is for therapy purposes.
What happens during an ultrasound scan?
There are not normally any special instructions to be followed before an ultrasound scan unless it is of the abdomen or pelvis, in which case you may be asked not to eat for 8-12 hours, or to ensure you have a full bladder for your appointment.
An ultrasound transmission gel is applied to the area being scanned to ensure good contact. A wand or probe (usually with a circular head) is then moved over the area, through which the sound waves are emitted. The sound waves are bounced back through the wand, down the wire, and transmitted on the computer monitor.
The picture displayed is continually changing so images of the valves of heart-opening and closing can be seen. Dynamic ultrasound (where the body part is moved during the scan) is particularly useful in some cases, for example, shoulder impingement syndromes.
What are they used for?
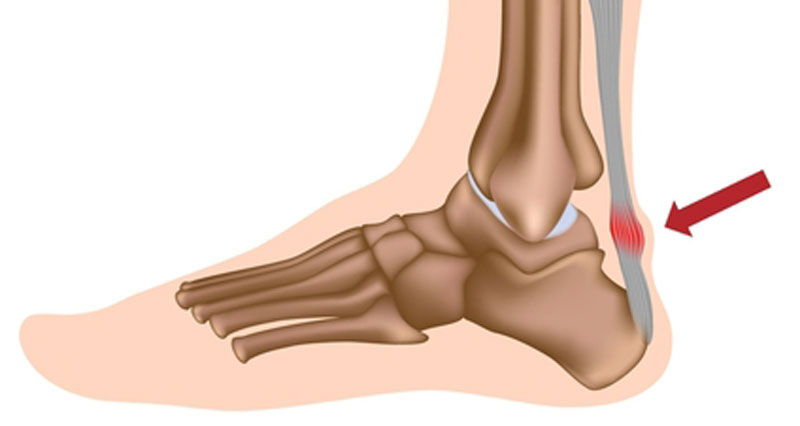
Ultrasound scans are used to look at soft tissues, to determine their size, shape, consistency, and any abnormalities. They are particularly useful for tendon injuries, especially tendinopathy (tendonitis) of the Achilles tendon and Patella tendons. And of course, used to look at unborn babies.