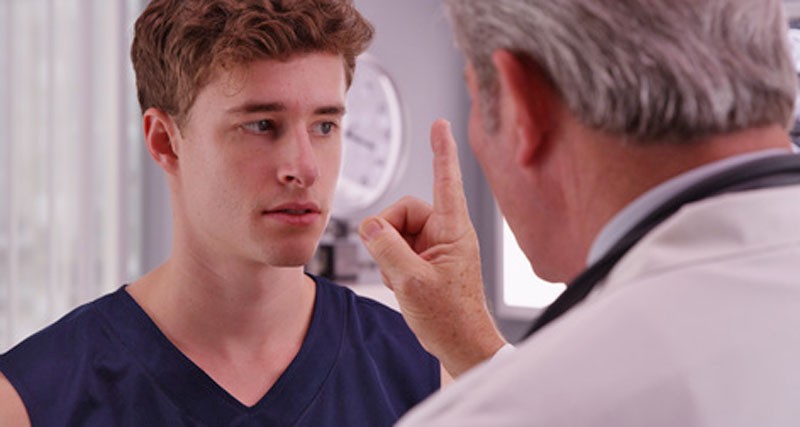
Every time a player sustains a head injury they may be at risk of more serious brain injury. If concussion is not correctly diagnosed and treated, more serious complications can occur. Here we explain first aid for concussion and how to treat a suspected head injury or concussion during a match.
First aid for concussion
First aid for concussion is to remove the player from the field of play and carry out an assessment. It is not always possible to carry out a full assessment at the time. Players are often confused and difficult to examine.
You must treat any play you suspect had a blow to the head as if they have concussion. This means stopping physical activity immediately and, if safe to do so, removing them immediately from the field of play.
Serious head injuries
If any of the following apply then suspect a more serious brain injury:
- The player had a high-speed impact or trauma to the head
- If the head makes contact with a hard surface or body part such as the knee
- Symptoms worsen over a short period of time, e.g. nausea or headaches.
- The patient lost consciousness immediately after the impact (however short the time was), or they have fallen unconscious since
- The patient has a seizure or fit
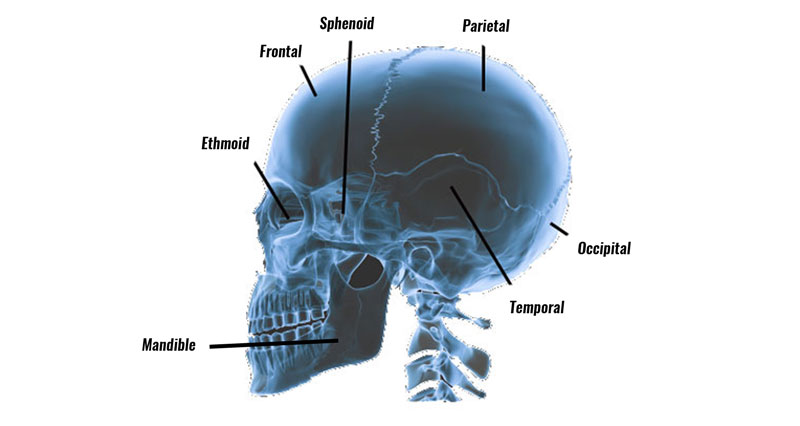
- Bleeding or fluid leaking from the nose or ear which could be evidence of a skull fracture
- A doctor detects a focal neurological deficit (see below)
Focal neurological deficit
A focal neurological deficit means that the brain does not function normally. As a result, and this may affect sensation or muscular movements anywhere in the body. It can also refer to memory loss and emotional changes.
If you suspect a player has concussion a doctor must assess them as soon as possible. If they lost consciousness at any point you must take them to hospital for a full assessment. The doctor may decide to refer for a brain scan to check for bleeding within the s
Immediate first aid for Concussion
The priorities when managing a suspected concussion injury pitchside are based on the principles of DR ABC. Only carry out this assessment if you have completed an Emergency Aid training course.
DR ABC stands for:
D for danger
Ensure the player and any staff assisting are not in further danger for example from any gameplay still occurring
R for a response
Is the player responding? Can they talk? Are they conscious?
A is for Airway
Remove any objects such as mouth guards from the mouth and ensure the airway is clear and in the optimized position
B is for breathing
Ensure the patient is able to breathe sufficiently
C is for Circulation
Assess by feeling for a pulse, but if the patient is not breathing normally or not at all, then start CPR immediately
Once you have assessed these stages, the next priority is to remove the player from the field. But first check for neck or spinal cord injury. This may appear as tenderness in the neck, deformity, change in sensation in the arms or legs, or if the patient complains of neck pain.
If you suspect a neck injury then do not move the player until you immobilise them in a brace. If the patient loses consciousness at any stage, then suspect a neck injury until you know otherwise.
Many
Examination
If there is a doctor present pitch side and there is no neck injury suspected, then a full neurological examination will be carried out, usually back in the changing rooms where it is quiet. It is possible the patient may be disorientated, uncooperative, or convulsing (fits).
If a suitably qualified person is not present, then the patient should always be taken to the hospital or an ambulance called. It is vital to establish an accurate diagnosis, as the consequences of missing concussion or associated brain injury could be fatal (see SIS).
Doctors use the SCAT5 assessment tool for concussion. Once a concussion is fully assessed, then the patient is continually monitored right up until full recovery (see treatment and return to play).