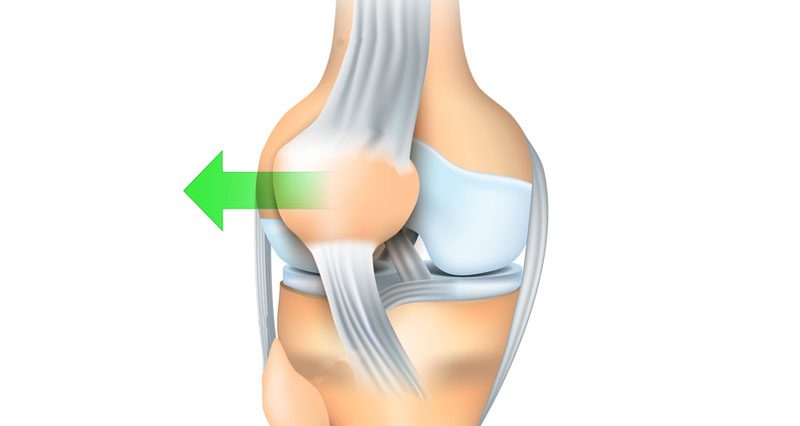
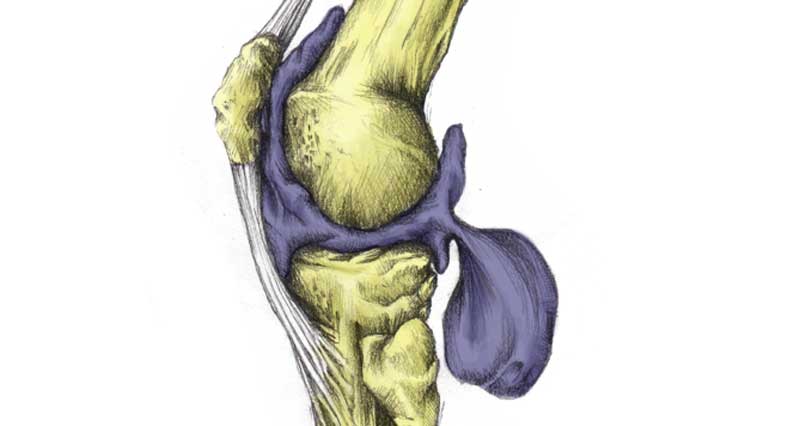
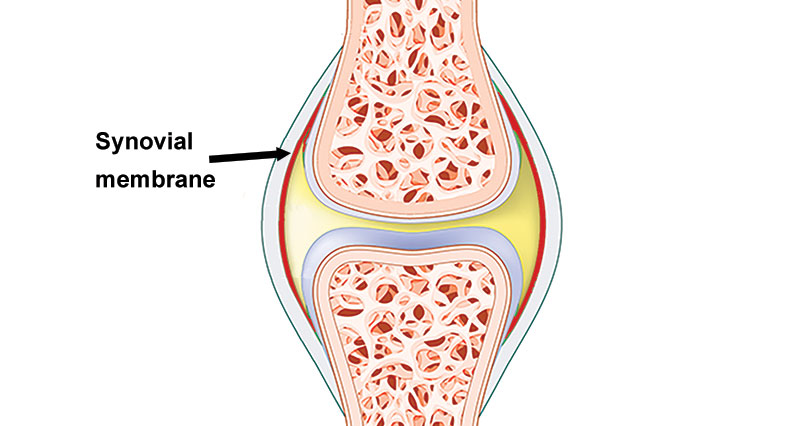
Patella dislocation occurs when the kneecap dislocates outside of its normal position. This is usually around the outside of the knee. It can also partially dislocate, called a subluxation. The patella will sometimes go back to its original position, although this will be very painful.
Medically reviewed by Dr Chaminda Goonetilleke, 2nd Jan. 2022
Symptoms of patella dislocation
Signs and symptoms of a dislocated patella include:
- Pain at the time of injury is often severe.
- Swelling in the knee joint
- An obvious displacement of the patella (kneecap).
Often the kneecap briefly dislocates and then returns to its normal position. If this happens then pain and swelling are usually also present.
Imaging
An X-ray and/or arthroscopy will help evaluate the extent of the injury.
Patellar dislocations sometimes have similar symptoms to anterior cruciate ligament injuries. This is due to an audible crack or pop and the feeling of the knee giving way.
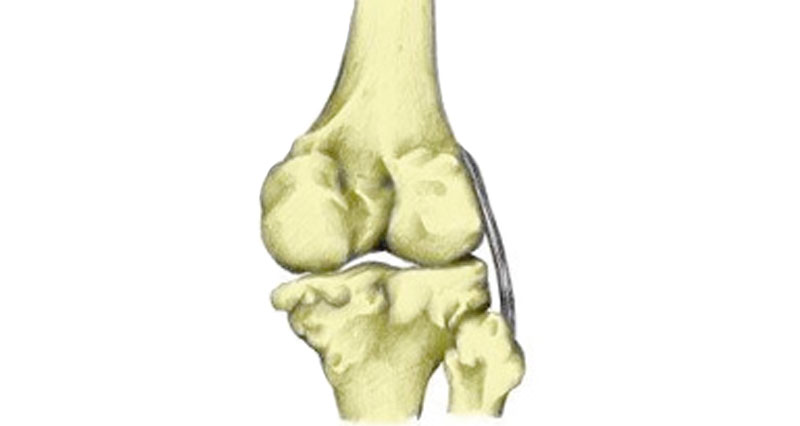
What is a Patella dislocation?
A dislocated patella occurs when the patella displaces outside of its normal position. This usually happens laterally (to the outside).
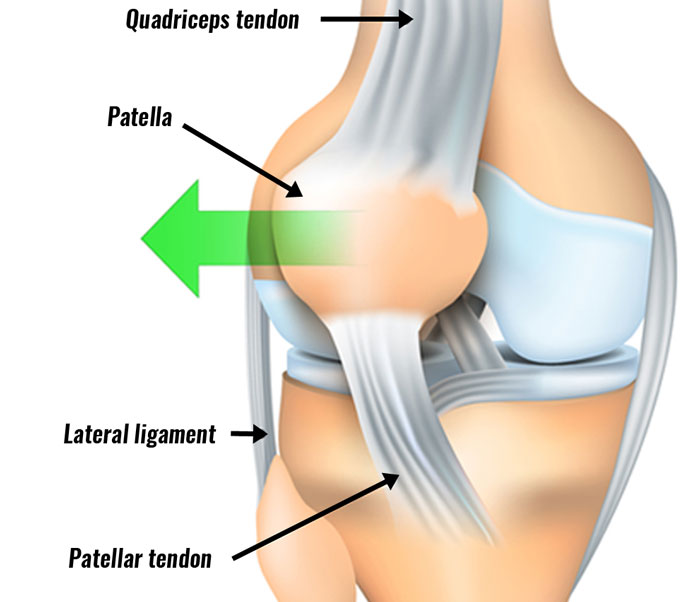
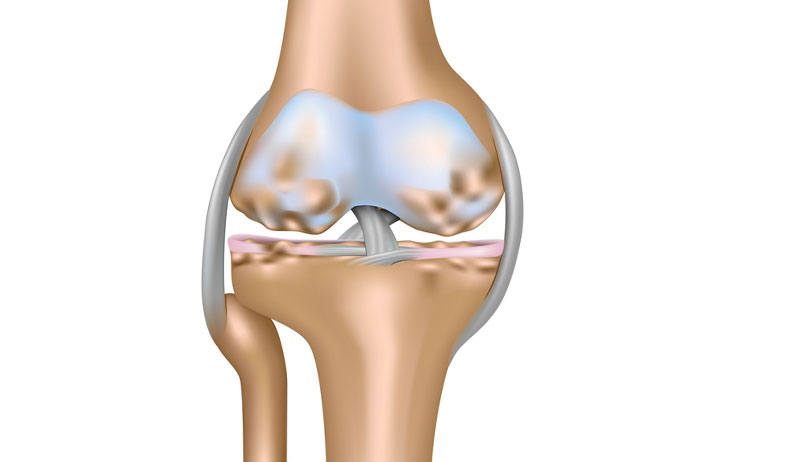
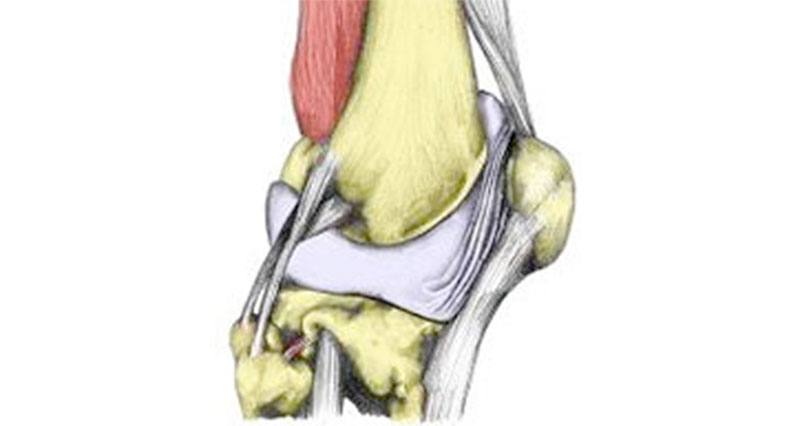
The patella or kneecap lies in front of the knee joint. It glides up and down a groove called the patellofemoral groove as the knee bends.
The patella attaches to the quadriceps muscle via the quadriceps tendon. It acts as a lever system when straightening the knee. Therefore, increasing the force the quadriceps exert.
Partial dislocation
The patella may also partially dislocate rather than fully dislocate. In other words, it moves partially out of position and then pops back in. This is known as subluxation or patellofemoral instability.
Patella dislocation is not the same as a dislocated knee, which is a much more severe traumatic injury.
Causes
It is usually a result of an acute blow or twisting action of the knee. In most cases, the patella relocates to the patellofemoral groove when you straighten the knee. However, this is usually extremely painful.
Patella dislocation is more likely with:
Weak vastus medialis oblique (VMO) muscle
The vastus medialis oblique muscle or VMO for short is the quad muscle on the inside of the thigh. It is responsible for maintaining the stability of the patella towards the inside of the knee.
If you have a weak VMO muscle then patella dislocation is more likely.
Overpronation of the feet.
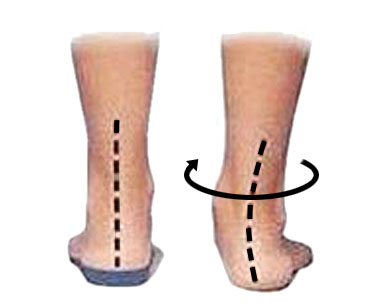
Overpronation of the feet is where the feet roll in or flatten too much when running. This causes the leg to turn inwards which leaves the patella susceptible to moving outwards as the quadriceps contract.
Increased Q angle of the knee.
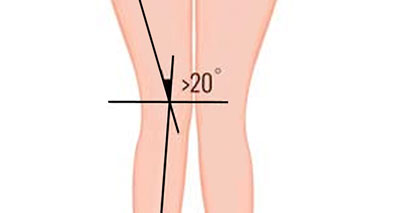
The Q-angle of the knee relates the angle of the lower leg to the knee. People with an increased Q angle appear ‘knock-kneed’. When they straighten their leg, it forces the patella to the outside of the knee, potentially resulting in patella dislocation.
Treatment of patella dislocation
Immediate first aid is to apply the PRICE principles of protection, rest, ice, compression, and elevation.
A healthcare professional may need to reduce the dislocation if it has not fallen back in place and this may be done under sedation or anaesthesia.
Cold therapy
Apply ice or cold therapy for 10 to 15 minutes every hour initially. Reduce frequency to 2 or 3 times a day as swelling and symptoms reduce.
Do not apply ice directly to the skin as it may burn. Wrap it in a wet tea towel. Or, even better, use a cold therapy wrap that applies compression as well.
Rest
Rest from any sporting activities and seek medical advice. If you have had one episode of patella dislocation you are often susceptible to another.
Avoid any activity which involves bending your knees.
Knee supports/braces
A knee support can provide protection for the joint. Patella stabilizing braces provide additional support for the kneecap.
Taping
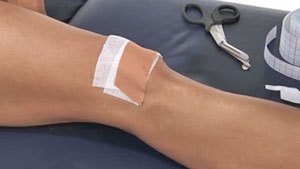
Patella taping supports the patella, helping to prevent it from moving or displacing sideways. Neither taping nor bracing completely eliminates the risk of future injury. They are both much less effective if you bend your knee.
- Read more on patella taping.
Exercises
When acute symptoms settle down and pain allows, begin a full knee rehabilitation program. This helps to reduce the risk of future injury. Specifically, exercises for the vastus medialis muscle on the inside of the quadriceps are important.
- Read more on VMO strengthening.
Medication
Your doctor may prescribe NSAIDs or anti-inflammatory medication such as Ibuprofen to reduce pain, inflammation, and swelling.
Surgery
Surgery may be necessary if there are loose fragments of bone or other major structural damage.