A herniated disc is sometimes also known as a slipped disc or prolapsed disc. It can occur anywhere in the spine although is most common in the lower back. Here we explain the symptoms, causes and treatment of prolapsed spinal discs.
What is a Slipped disc?
A slipped disc is a general term used to describe what is actually a prolapsed disc in the spine. Of course, it doesn’t actually slip out.
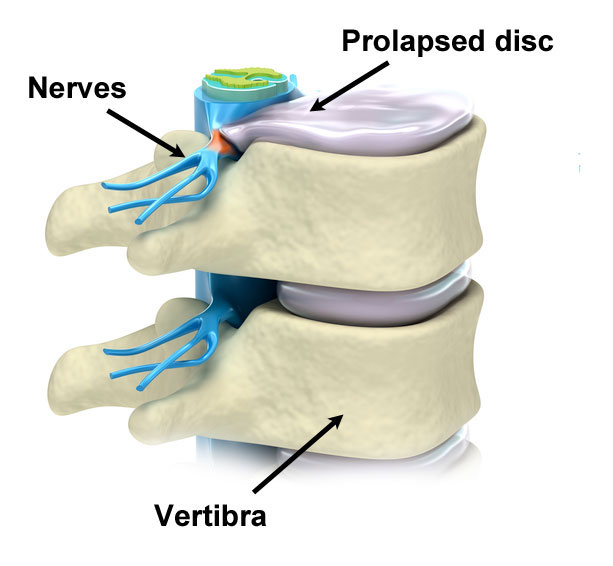
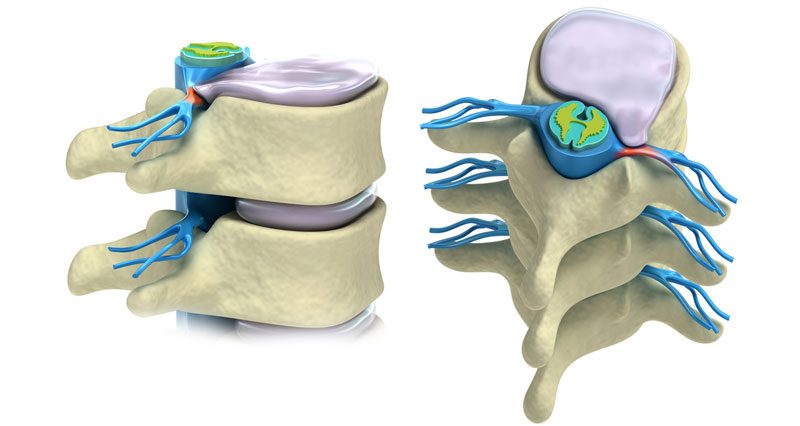
The intervertebral discs are roughly round pads of cartilage that sit between each spinal vertebra (bone). Their job is to provide shock absorption and to allow the movements of the spine. The spine has a huge range of movement, bending forwards, backward, sideways, and rotating. Whilst lumbar disc herniations can occur at any point in the spine, they are most common in the lumbar (lower back).
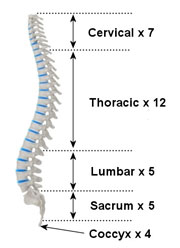
Here there are 5 lumbar vertebrae, separated by 5 intervertebral discs. Each vertebra has a body (a large circular area at the front) and three bony processes which protrude out the back. These are the two transverse processes and the central spinous process. Between the body and these processes is a circular hole, which together with the vertebrae above and below, forms a column through which the spinal cord passes.
The intervertebral disc is made up of three parts. The vertebral endplates, the annulus fibrosus, and in the centre, the nucleus pulposus. It is this central part that may herniate, through a weakened, degenerated wall (annulus fibrosus).
If the disk herniates far enough it can put pressure on the spinal column where it passes behind the discs and vertebral bodies. It is this pressure on the spinal cord which refers to pain and other symptoms in the legs.
What are the Symptoms?
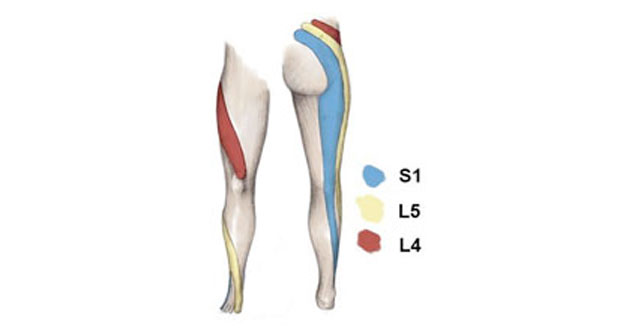
Symptoms will depend on which disc is injured. They include back pain, leg pain, neural symptoms as well as bowel and bladder problems. Most (90%) of lumbar spine herniations occur at either L4/L5 or L5/S1. Where the herniation and so spinal cord compression occurs, dictates the symptoms the individual will feel. In most cases, some degree of lower back pain will be felt and this may be accompanied by:
Leg pain
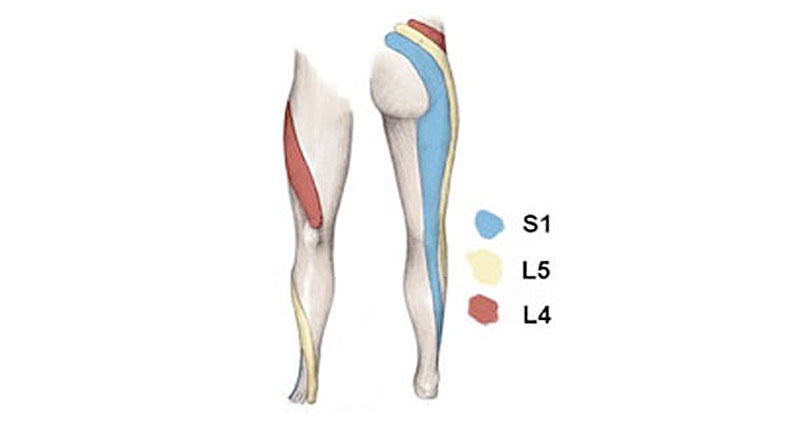
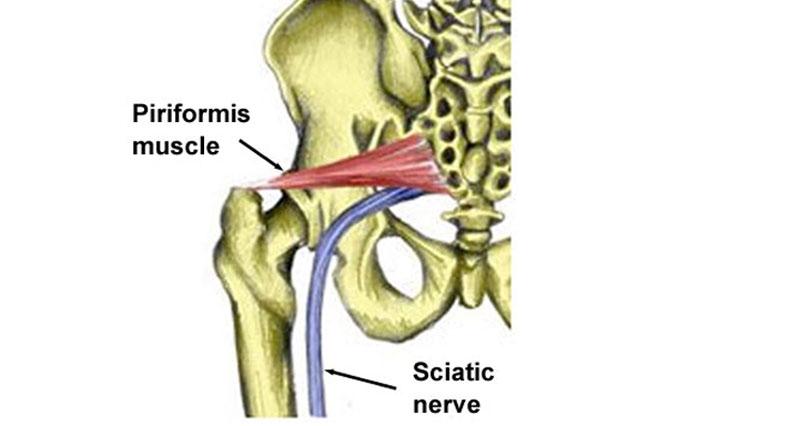
- In the L5/S1 disc herniation, the pain is often felt down the back of the leg, often as far as the foot (see sciatica).
- With L4/L5 herniations the pain may be felt more on the outside of the leg and down into the shin or top of the foot.
- L3/L4 herniations often produce pain on the outer hip and round onto the front of the thigh.
Neural symptoms
- Neural symptoms are those produced b a nerve and include tingling, numbness, and weakness. These symptoms are common in those with a slipped disc and tend to be in the areas described above, in line with areas of pain.
- Weakness in the foot is especially common, with difficulty lifting the foot (known as foot drop) often reported in those with L4/L5 herniation.
Pain patterns
- Pain often occurs after a relatively simple movement, such as bending over to pick up something light off the floor.
- It is often aggravated by sitting, bending, lifting and coughing or sneezing.
- It is often eased by lying down, especially on the unaffected side and maybe at its best first thing in the morning.
Bladder/Bowel Symptoms
- If there are any symptoms of a loss of bladder or bowel control then this should be treated as a medical emergency.
- It could be a condition known as Cauda Equina Syndrome which is a serious condition as it may result in permanent loss of bladder or bowel control and paralysis in the lower body.
- Seek medical attention immediately.
How is a Slipped Disc Diagnosed?
If you think you may have a slipped disc the best course of action is to visit your Doctor. He/she will be able to make an assessment and determine what treatment or investigations are needed.
Your doctor may refer you for physical therapy with a Physiotherapist or Chiropractor. They may also refer you to the hospital for a scan such as an X-ray, MRI scan, or CT scan.
Treatment of Slipped disc
- In many cases, a slipped disc in the lower back will heal with conservative treatment. Initially, this should involve rest and the use of anti-inflammatory medications or NSAIDs such as Ibuprofen.
- Physical therapy may help, with the use of gentle mobilizations and extension exercises. A corticosteroid injection may be given in severe cases which show no signs of improvement naturally.
- Traction is often helpful for patients with a disc herniation, although in some cases the initial pain relief was followed by an increase in pain after treatment.
Surgery
in cases where the symptoms do not improve or the individual suffers repeated bouts of pain, surgery may be an option. There are two procedures that may be carried out:
- A microdiscectomy involves removing only the portion of the disc which has herniated, leaving the rest of the disc intact. In most cases, this is successful although patients may be prone to further episodes. The surgery is usually performed on an outpatient basis and the individual can be back to full work duties within 1-3 weeks.
- For substantial or repeated herniations a full discectomy may be performed. In this case, the entire disc is removed and the vertebrae above and below are fused.
Expert Interview
Chiropractor Dr Maria Madge talks about a so-called slipped disc or prolapsed disc.
The SI joints are two very large joints that attach the sacrum to the two other parts of the pelvis. They can cause a lot of localised pain, both in the groin area and lower back.
It is surprising how much pain these joints can cause. They can give pain in the hip area and buttocks but also referred pain in the thigh and even down to the heel.
The joints generally will get stiff from a fall or some types of activity such as bending, digging, or sitting. The muscles then get irritated and there is inflammation in that area. Because the joint is not working properly, the whole pelvic complex doesn’t work properly and pain may occur on the other side too.
The pain is felt really low in the back, around the pant line. Pain may also refer up the back.
A chiropractor can help to increase the mobility of the joint using mobilization techniques and adjustments, as well as loosening the gluteal and lower back muscles.