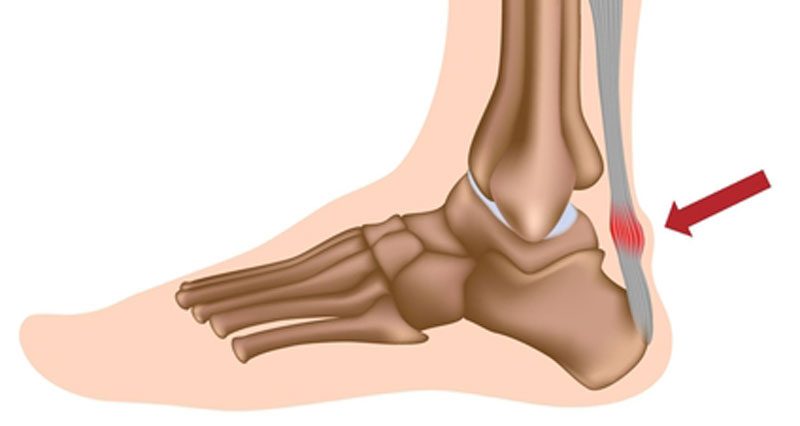
Achilles tendonitis is a common cause of pain at the back of the ankle, particularly in runners and active people. It develops when the Achilles tendon becomes overloaded during activity, causing pain, stiffness and reduced performance.
Early treatment and the right rehabilitation are essential. Without this, symptoms often become long-term and harder to resolve. Many chronic cases are better described as Achilles tendinopathy, where the tendon becomes weakened rather than inflamed.
This guide covers Achilles tendonitis symptoms, causes, treatment and rehabilitation. Learn how to manage pain, restore strength and return to activity safely.
What is Achilles tendonitis?
Achilles tendonitis, also known as Achilles tendinopathy, is an overuse injury affecting the tendon at the back of the ankle.
The Achilles tendon is the large, thick band of tissue at the back of the ankle. It connects the calf muscles to the back of the heel.
Tendonitis vs tendinopathy
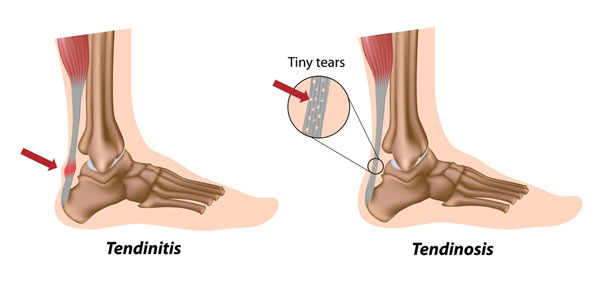
Tendonitis suggests inflammation of the tendon (‘itis’ means inflammation). However, most long-term Achilles injuries are not caused by ongoing inflammation.
In longer-term cases, the tendon shows changes in its structure rather than inflammation. This is why the term tendinopathy is now more commonly used. It better describes the range of tendon changes that lead to pain and reduced function.
Symptoms of Achilles tendonitis
Symptoms of Achilles tendonitis usually develop gradually and may worsen over time if not managed properly.
Common symptoms include:
- pain at the back of the ankle or lower calf
- stiffness, especially first thing in the morning
- pain that improves with movement but returns after activity
- tenderness when pressing or squeezing the tendon
- swelling or thickening in the tendon
- reduced strength when pushing off or running
In some cases, a small lump or thickened area may develop within the tendon. This is more common in longer-term Achilles tendinopathy.
If left untreated, symptoms can become persistent and may increase the risk of a more serious injury, such as an Achilles tendon rupture.
Causes of Achilles tendonitis
Achilles tendonitis usually develops when repeated strain is placed on the tendon without enough recovery.
Poor foot biomechanics
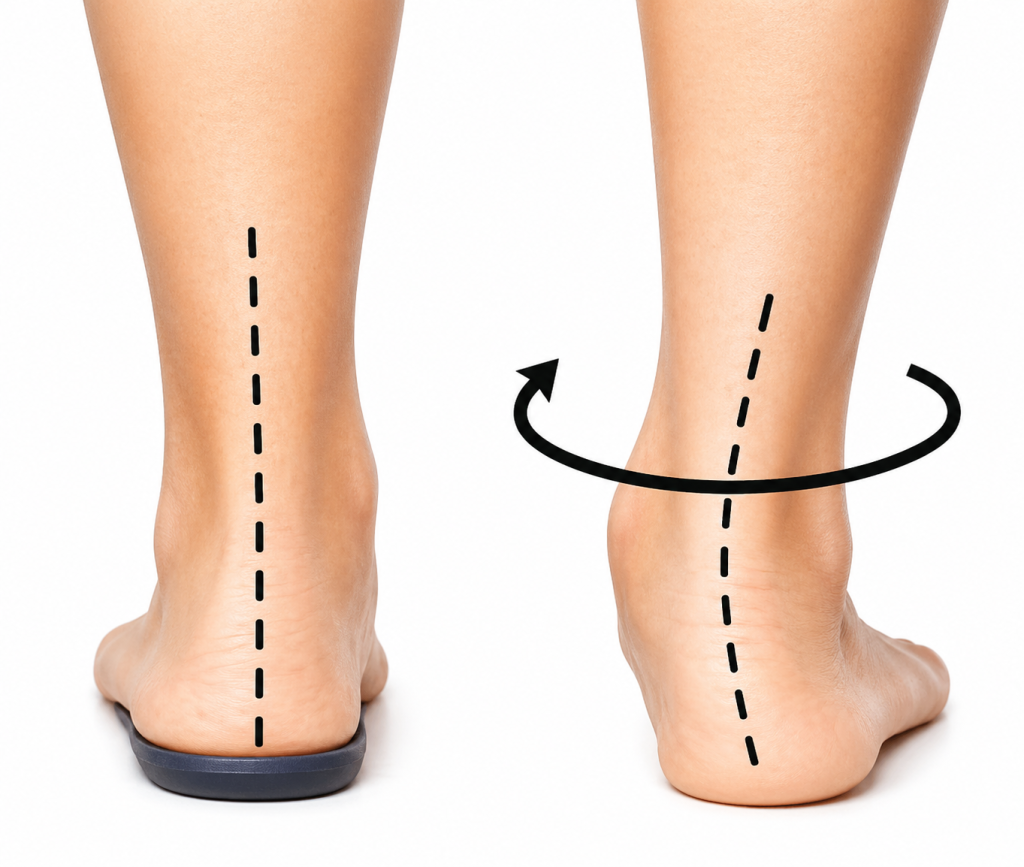
Overpronation is when your foot rolls in too much. This causes the lower leg to rotate, which increases strain through the Achilles tendon.
Incorrect footwear
Make sure you choose the right running shoes for your foot type and the sport. This is because worn-out or unsupportive shoes increase the load on your Achilles tendon and raise the risk of injury.
Wearing high heels
Regularly wearing high heels can shorten the calf muscles over time. This increases strain on the Achilles tendon when switching back to flat shoes.
Training errors
Increasing training load too quickly is a common cause. Aim to increase running distance gradually, typically no more than 10% per week.
Running on soft surfaces such as sand allows your heel to sink, increasing the stretch on the Achilles tendon.
Uphill/treadmill running
Frequent uphill or incline running increases the load through the Achilles tendon and raises the risk of irritation.
Achilles tendonitis treatment
Treatment for Achilles tendonitis focuses on reducing pain while gradually restoring strength and load through the tendon.
A structured exercise program is the most effective treatment for longer-term Achilles tendon pain. Recovery should be based on progressive loading, rather than complete rest, to rebuild strength safely and reduce the risk of recurrence.
Apply ice/cold therapy
For an acute injury, apply ice for 10 minutes every hour or so for the first 2 to 3 days. Reduce frequency as your symptoms improve.
Rest
This may mean complete rest or simply modifying your training activities.
Medication
Your doctor may prescribe anti-inflammatory medication. For instance, ibuprofen helps with acute inflammation. However, it is less effective for long-term tendon pain and does not address the underlying issue.
Electrotherapy
The application of Electrotherapy, such as ultrasound, reduces pain and inflammation.
Heel lift/heel pad
This helps reduce strain on your Achilles tendon by temporarily shortening the calf muscle.
Wear in both shoes, not just the bad leg. Also, use it only for a few days to avoid adaptive shortening of your tendon.
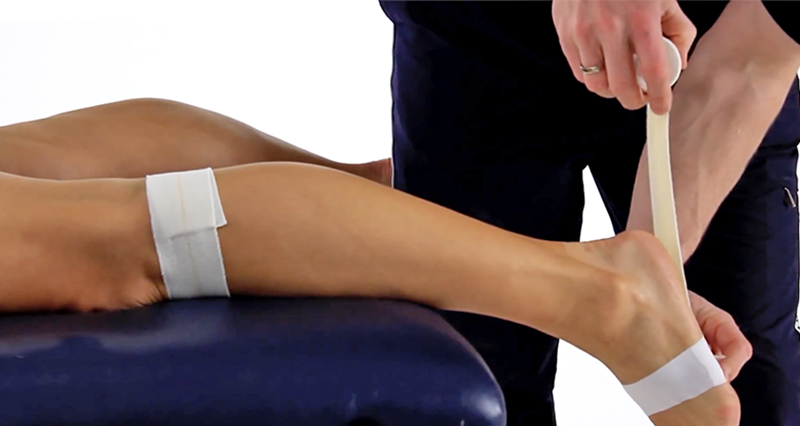
Achilles tendon taping

Taping can help reduce strain on the Achilles tendon and provide short-term support during activity. It may be useful if you need to stay on your feet, but it should not replace proper rehabilitation.
Heat
Long-term chronic injuries may respond better to the application of heat. Apply for 10 minutes every couple of hours as required.
Night splint/sock
A night splint or sock is a good product for Achilles tendonitis. It is more commonly known as a Plantar fasciitis night splint and improves calf muscle flexibility, preventing them from tightening up overnight.
Massage
Massage can help reduce tension in the calf muscles and improve mobility around the Achilles tendon. Tight or overloaded calf muscles increase the strain placed on the tendon, particularly during running and jumping activities.
If your pain is higher up in the calf rather than directly on the tendon, it may indicate a calf strain.
Achilles tendonitis exercises and rehabilitation
Exercise-based rehabilitation is the most effective treatment for Achilles tendon pain. Exercises should be introduced gradually and progressed based on your tendon’s response.

Eccentric heel drop exercises are one of the most effective treatments for Achilles tendinopathy.
Achilles tendonitis heel drop exercises are effective for treating chronic Achilles tendon pain. Hakan Alfredson’s heel drop protocol involves performing heel-drop repetitions twice daily for 12 weeks.
Read more about Achilles tendon heel drop exercises.
Stretching exercises
Gentle calf stretching can help improve flexibility and reduce tension through the Achilles tendon. However, stretching alone is not enough and should be combined with strengthening exercises.
A structured rehabilitation program ensures exercises are progressed safely and at the right time. Our Achilles Tendonitis Rehab Program guides you through each stage with video exercises, daily plans and criteria-based progression to help you recover fully and reduce the risk of re-injury.
Scans and diagnosis
An MRI or ultrasound scan can help assess the extent of the injury and confirm the diagnosis.
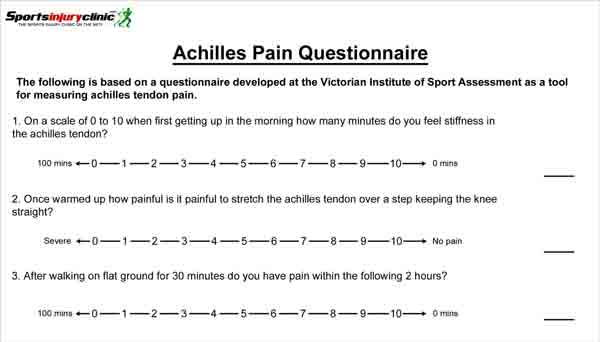
How severe is your Achilles tendon pain?
VISA A questionnaire (download PDF) is a simple way to measure how severe your Achilles tendon pain is. It provides a score out of 100 and is useful for tracking progress during rehabilitation.

Tenosynovitis is another condition that can cause pain around the Achilles tendon. It involves inflammation of the sheath surrounding the tendon and may present with similar symptoms.
References
- Robinson JM, Cook JL, Purdam C et al. The VISA-A questionnaire: a valid and reliable index of the clinical severity of Achilles tendinopathy. BJSM 2001;35(5):335-41
- Alfredson H, Lorentzon R. Chronic Achilles Tendinosis – recommendations for treatment and prevention. Sports Med 2000;29(2):135-46
- Alfredson H, Piettila T., Jonsson P et al. Heavy-load eccentric calf muscle training for the treatment of chronic Achilles tendinosis. American Journal of Sports Medicine 1998;26(3):360-6