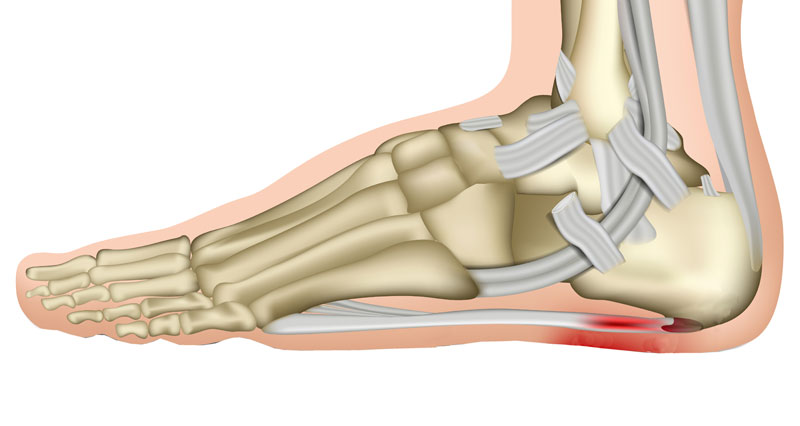
Plantar fasciitis is the most common cause of pain under the heel. It involves inflammation or degeneration of the plantar fascia, a thick band of tissue supporting the arch of your foot. Pain under the heel can radiate into the arch and is typically worse first thing in the morning.
Advert
Symptoms
Symptoms of Plantar fasciitis usually develop gradually over time and include:
- Pain under the heel.
- Sometimes the pain radiates into the arch of your foot.
- Tenderness when pressing in under your heel.
- Pain is usually worse first thing in the morning.
- Symptoms improve as your foot warms up, but return later.
Symptoms are typically worse after periods of rest, such as sleeping or sitting for long periods.
Diagnosis
Plantar fasciitis is usually diagnosed based on your symptoms and a physical examination.
Your physio or doctor may:
- Press on the heel to identify the point of maximum tenderness
- Check for tightness in the calf muscles and plantar fascia
- Assess foot posture and biomechanics
- Look for pain when stretching the plantar fascia
Imaging such as X-rays or MRI scans is not normally required but may be used to rule out other conditions if symptoms are severe or do not improve.
Similar injuries: What else might it be?
Injuries with similar symptoms include:
What is Plantar fasciitis?
Plantar fasciitis is inflammation (or degeneration) of the Plantar fascia at the point it attaches to the heel.
Anatomy
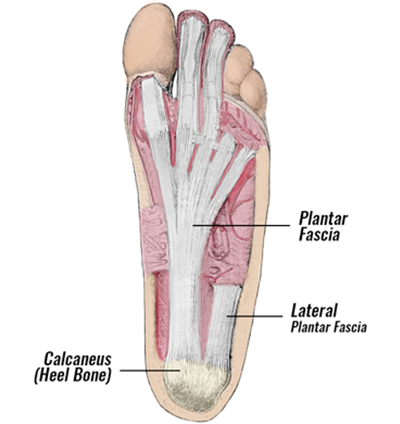
The Plantar Fascia (or plantar aponeurosis) is a broad, thick band of tissue under the foot. It runs from under the heel bone (calcaneus), to the ball of the foot. It provides support to your foot when standing and shock absorption when running.
Advert
Plantar fasciitis or Plantar fasciopathy?
The term Plantar fasciitis describes inflammation (‘itis’ means inflammation). Traditionally people thought inflammation was the problem. However, studies now show inflammatory cells are not present in most cases.
Therefore, degeneration of the tissues is a more likely cause. In this case, the term Plantar fasciopathy is probably more accurate because it describes degeneration/wear and tear.
What causes Plantar fasciitis?
Overuse is the main cause of Plantar fasciits. However, there are a number of factors which increase your chances of developing it. These include poor foot biomechanics, for example, overpronation, or if you have a rigid, high-arched foot. Inappropriate footwear is another factor. For example, wearing very flat or unsupportive shoes. Or wearing the wrong running shoes for your foot type.
If you are heavy or overweight then this increases the load on your foot. Or if you have tight calf muscles or plantar fascia then you are also at a higher risk of injury.
Plantar fasciitis treatment
The following treatment methods form part of our full rehabilitation program. The aim of treatment is to protect your foot, and reduce pain and inflammation.
Cold therapy
Apply ice or cold therapy every couple of hours for 10 to 15 minutes in order to reduce pain and inflammation. Reduce this to 3 times a day as your symptoms improve.
Taping
Applying Plantar fasciitis taping often instantly relieves symptoms. It works by supporting the arch of the foot and as a result, reduces the strain on the plantar fascia. Therefore, allowing tissues to heal.
Footwear & Insoles
Wear comfortable shoes or supportive trainers and avoid hard or flat-soled shoes. Cushioning heel pads or insoles help relieve pain. However, if your overpronate (your foot rolls in or flattens) then orthotic-type insoles are more appropriate.
Plantar fasciitis night splint
The night splint or sock is worn overnight and helps prevent the fascia and calf muscles from tightening up.
Massage
Deep tissue massage to the arch of the foot helps stretch and relax the plantar fascia. Avoid the painful area near the heel, especially if it is acutely painful.
Electrotherapy
Your physiotherapist may use Extracorporeal shock wave therapy or Ultrasound therapy.
Medication
Your doctor may prescribe anti-inflammatory medication such as ibuprofen. This is effective in the early stages to reduce pain and inflammation. However, studies show long-term use may actually inhibit healing. Also, check with a doctor or pharmacist before taking medication.
Gait analysis
Gait analysis involves analysing your feet and how you walk and run. If you overpronate, or your feet flatten then orthotic inserts may be prescribed to correct biomechanical issues
Platelet-rich plasma injections
For more stubborn injuries a doctor may try a corticosteroid injection. Platelet-rich plasma injections have also been shown to be effective. If symptoms do not resolve then surgery is an option but this is rare.
Read more on treatment.
Plantar fasciitis exercises
Exercises to stretch the plantar fascia and the calf muscles are particularly important. Rest alone reduces pain and inflammation, however, if fascia tension is a cause then your pain is likely to recur.
Our full Plantar fasciitis rehab program includes stretching, strengthening, activation, movement control and functional exercises.
- Stretching for the plantar fascia and calf muscles including foot rolling.
- Strengthening of the foot and plantar fascia as well as the posterior chain (legs and hips).
- Activation exercises to keep the hip muscles firing and in good condition.
- Movement control to maintain balance and proprioception.
- Functional exercises to bridge the gap between basic rehab and sports-specific training.
Learn more about specific Plantar fasciitis exercises or go direct to our Plantar fasciitis rehabilitation program.
Plantar fasciitis surgery
Surgery is indicated for around 5% of people, in particular, whose symptoms do not improve after a minimum of nine months of continuous treatment. However, the success rate is still only estimated at around 70-80%.
In most cases, your surgeon performs a procedure called a plantar fascia release. This releases (cuts) between 30 and 50% of the fascia’s fibres. As a result, stress on the fascia is reduced. However, possible complications include nerve damage, fallen arches, infection, and ongoing symptoms. Recovery after surgery, if successful, is around 9 to12 weeks before the patient returns to work.
Rehabilitation program
Our Plantar fasciitis rehabilitation program is criteria-based, guiding you from early-stage recovery through to full performance. Progress through five phases at your own pace, meeting specific targets before moving on. This program is suitable for anyone suffering from acute (recent) or chronic (long-term) heel pain from Plantar fasciitis.
External Links
Buy Plantar Fasciitis insoles at 1000mile.co.uk
References & Research
- Lemont H, Ammirati KM, Ulsen N. Plantar fasciitis: a degenerative process (fasciosis) without inflammation. J Am Podiatr Med Assoc 2003;93(3):234-37
- Riddle DL, Pulisic M, Pidcoe P et al. Risk factors for PF: a matched case-control study. J Bone Joint Surg Br 2003;85-A(5):872-7
- Gonnade N1, Bajpayee A2 et al Regenerative efficacy of therapeutic quality platelet-rich plasma injections versus phonophoresis with kinesiotaping for the treatment of chronic PF: A prospective randomized pilot study. Asian J Transfus Sci. 2018 Jul-Dec;12(2):105-111
- Malahias MA, Cantiller EB, Kadu VV, Müller S. The clinical outcome of endoscopic plantar fascia release: A current concept review. Foot Ankle Surg. 2018 Dec 23. pii: S1268-7731(18)30233-9
Medically reviewed by Dr Chaminda Goonetilleke, 20th Jan. 2022