Calf strain treatment and recovery depend on the severity of the injury. A mild calf strain may settle within 2 to 3 weeks, while more serious injuries can take several months and require structured rehabilitation.
A calf strain is a tear in one or more of the muscles at the back of the lower leg. It often happens during sprinting, pushing off, or sudden changes in direction. You may feel anything from a tightness or pulling sensation to a sudden sharp pain or even a ‘pop’ in more severe cases.
This guide explains the key symptoms, causes, treatment, and rehabilitation strategies to help you recover fully and return to sport safely.
Medically reviewed by Dr Chaminda Goonetilleke, 10th Jan. 2022.
Calf strain symptoms
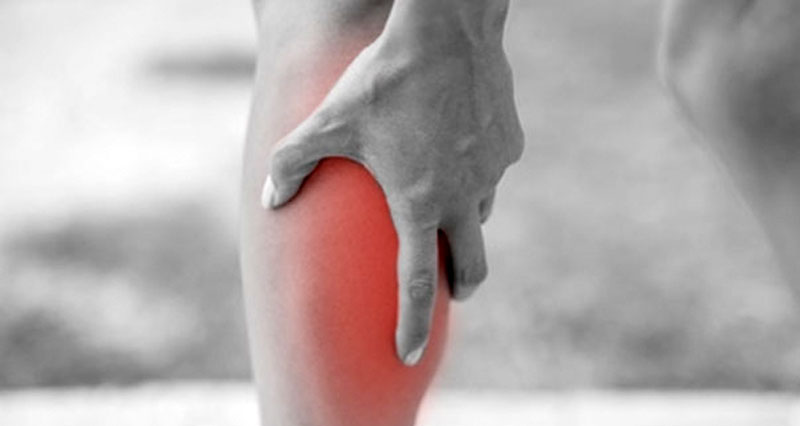
Symptoms of a calf strain vary depending on the severity of the injury. Mild strains may feel like a tightness or dull ache, often during or after exercise. More severe strains cause a sudden, sharp pain at the back of the lower leg.
Calf strains are graded from 1 to 3, with grade 3 being the most severe. Understanding the severity of your injury is important for choosing the right treatment and rehabilitation approach.
Grade 1
Grade 1 is a minor calf strain involving a small number of muscle fibres. You may feel a slight twinge or tightness in the back of the lower leg.
You can often continue activity, although discomfort usually increases afterwards. Symptoms may take up to 24 hours to fully develop. Without proper management, a mild strain can progress to a more serious injury.
Grade 2
Grade 2 calf strains involve a more significant tear of the muscle fibres. You typically feel a sudden, sharp pain in the back of the lower leg.
Swelling and bruising often develop, and walking or pushing up onto your toes is painful. You are usually unable to continue activity.
Grade 3
Grade 3 is a complete or near-complete rupture of the muscle. Severe pain occurs immediately, often with a noticeable ‘pop’ at the time of injury.
Swelling develops quickly, followed by bruising. In some cases, you may feel or see a gap in the muscle, and walking is extremely difficult.
If you suspect a grade 2 or 3 injury, we advise seeking professional advice.
Calf strain causes
Calf strains usually occur during sudden, explosive movements such as sprinting, pushing off, or changing direction quickly. They can also happen when the muscle is overstretched under load.
Several factors increase your risk of developing a calf strain:
- Poor warm-up – tight or unprepared muscles are more likely to strain during activity.
- Tight calf muscles – reduced flexibility increases stress on the muscle, especially during running and sprinting.
- Previous calf injury – weak or poorly rehabilitated muscles are more prone to re-injury.
- Sudden increase in training load – doing too much too soon, or returning to sport too quickly.
- Wearing high heels regularly – this shortens the calf muscles over time, increasing strain when switching to flat shoes or running.
Preventing these risk factors is an important part of long-term recovery and reducing the chance of re-injury.
Calf strain treatment
Early treatment focuses on protecting the muscle, reducing pain and swelling, and gradually restoring movement. Acting quickly can help speed up recovery and reduce the risk of long-term problems.
In the early stages, the P.R.I.C.E. principles (protection, rest, ice, compression, and elevation) can be used to manage symptoms.
Cold Therapy
Apply cold therapy for 10 to 15 minutes every 1 to 2 hours during the early stages. Reduce frequency as pain and swelling improve.
Always protect the skin by wrapping ice in a towel or using a compression wrap.
Rest
Rest is important in the early stage, especially if walking is painful. However, complete rest should be short-term.
As pain settles, gentle movement and controlled loading help the muscle heal more effectively. Avoid pushing through pain.
Compression & support
Compression can help reduce swelling and provide support. Use a calf support or compression bandage during the early stages.
As you return to activity, a supportive sleeve can help keep the muscle warm and improve confidence when moving.
A trained therapist may apply a compression bandage immediately after injury to help limit bleeding and swelling.
Medication
Anti-inflammatory medication such as ibuprofen may help reduce pain in the first few days. However, prolonged use may interfere with muscle healing.
Always follow medical advice and check with a pharmacist or doctor before taking medication.
Wear a heel lift
Using a small heel lift can reduce strain on the calf muscle by slightly shortening it. This may help in the early stages of recovery. Use them in both shoes to avoid imbalance.
As your symptoms improve, treatment should shift from protection and rest towards gradual loading and rehabilitation.
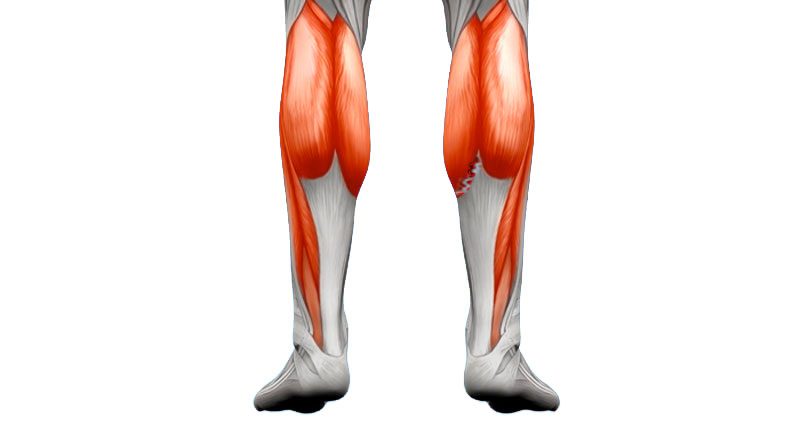
Calf strain anatomy
A calf strain involves a tear in one of the muscles at the back of the lower leg, most commonly the gastrocnemius.
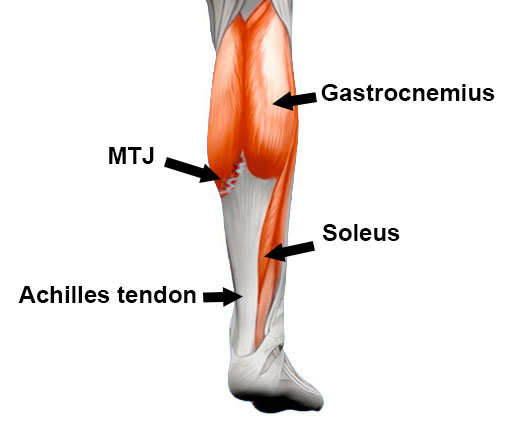
The calf muscle group consists of two main muscles: the gastrocnemius and the soleus. The gastrocnemius is the larger, more powerful muscle used during sprinting and explosive movements.
The soleus sits underneath and works more during steady activities such as walking and running. Both muscles help point the foot downward (plantar flexion), which is the movement used when pushing off or standing on your toes.
Most calf strains occur in the medial (inside) part of the gastrocnemius, often at the musculotendinous junction where the muscle joins the tendon. This type of injury is sometimes referred to as ‘tennis leg’.
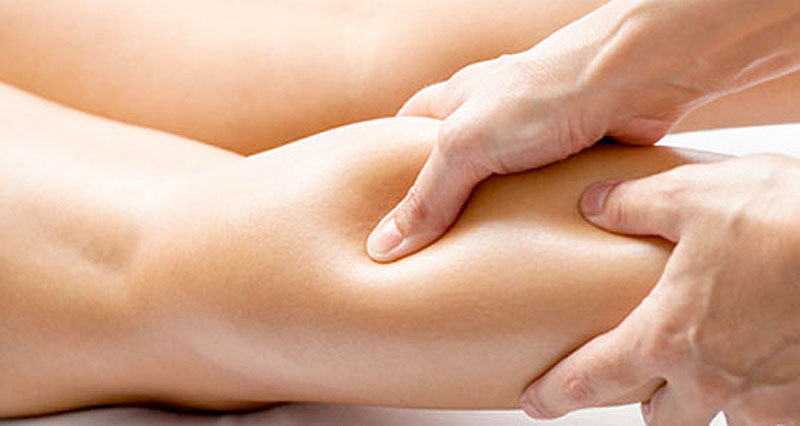
Massage

Sports massage can be useful once the early acute phase has settled. Avoid massage in the first few days after injury, as it may increase bleeding and disrupt healing tissue.
As recovery progresses, massage can help improve blood flow, reduce stiffness, and loosen tight areas within the muscle.
- Learn how to apply massage for calf strains
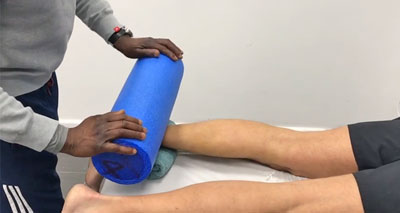
Foam roller for pulled calf muscles
A foam roller can be used as an alternative to massage in the later stages of rehabilitation.
Roll slowly along the length of the calf for 1 to 2 minutes. This can help improve mobility and reduce muscle tightness.
- Learn how to use a foam roller for calf injuries
Electrotherapy
A physiotherapist may use ultrasound therapy to support healing in the early stages. It can help increase blood flow and promote tissue repair.
Massage should be used alongside a structured rehabilitation programme, not as a replacement for it.
- View phase 1 of our full Calf strain treatment program
When to start rehabilitation exercises
Rehabilitation should begin once you can walk without significant pain and swelling has started to settle.
Start with gentle mobility and light activation exercises. As your symptoms improve, you can gradually progress to strengthening, loading, and eventually running.
Progressing too quickly can delay recovery, but doing too little can also slow healing. Following a structured, step-by-step approach helps ensure you return to full activity safely and reduces the risk of re-injury.
Calf strain rehabilitation & exercises
Rehabilitation is essential for a full recovery from a calf strain. Without the right progression, symptoms often return when you try to run or train again.
A structured programme should begin with gentle mobility and activation exercises, before progressing to strength, loading, and eventually running.
Our calf strain rehabilitation program has been designed by England & British Lions Rugby Sports Physiotherapist Phil Pask. It follows a step-by-step, criteria-based approach so you only progress when your calf is ready.
This helps you recover safely and reduces the risk of re-injury.
Return to running and sport
Returning to running too soon is a common cause of re-injury. You should only progress once you can walk, jog, and perform strength exercises without pain.
A gradual return to running, combined with ongoing strengthening, helps ensure a safe and complete recovery.
Calf strain references & research
- Koulouris G, Ting AYI, Jhamb A et al. Magnetic resonance imaging findings of injuries to the calf muscle complex. Keletal Radiol 2007;36:921-7
- Orchard J, Alcott E, James T, et al. Exact moment of a gastrocnemius muscle strain was captured on video. Br Journal Sports Med 2002;36:222-3
- Kwak HS, Han YM, Lee SY, et al. Diagnosis and follow-up US evaluation of ruptures of the medial head of the gastrocnemius (‘tennis leg’). korean J radiol 2007;7(3):193-8