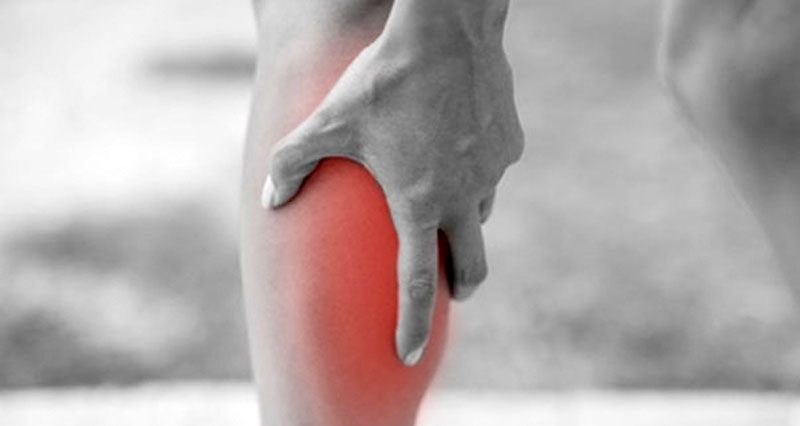
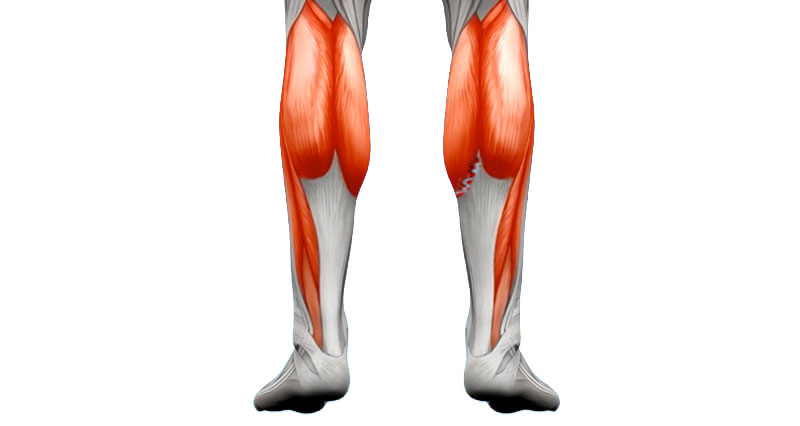
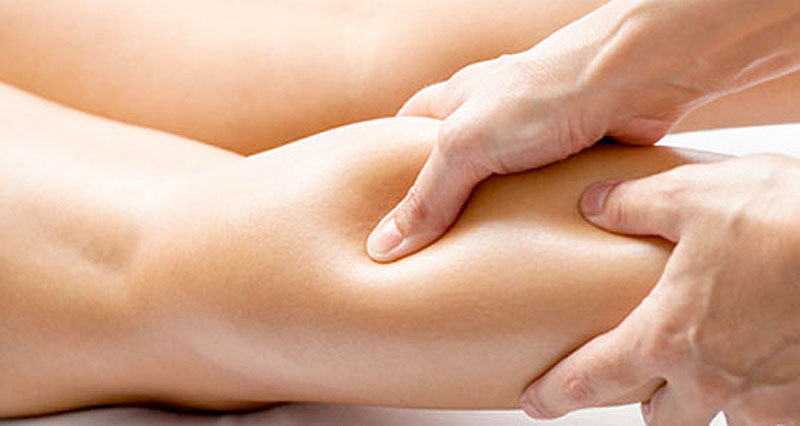
Calf pain is pain at the back of the lower leg. It either occurs suddenly, for example a calf muscle strain. Or develops gradually over time as in the case of a compartment syndrome. Here we explain the common causes of calf pain as well as more serious conditions you need to be aware of such as a deep vein thrombosis.
Select the type of calf pain:
Sudden onset (acute) calf pain
The following injuries are common causes of sudden onset or acute calf pain:
Calf strain
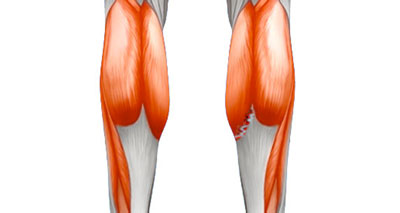
Probably the most common cause of sudden onset pain at the back of the lower leg. Symptoms consist of:
- Sudden sharp pain at the back of the lower leg
- Tenderness pressing in over the area
- Swelling and/or bruising (but not always)
- Read more on a Calf strain
Calf contusion
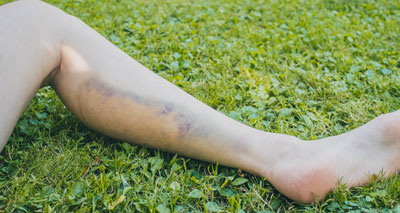
A contusion occurs following a direct impact or trauma to the calf muscles. Symptoms include:
- Sudden calf pain at the point of impact
- Pain may be mild, or so severe you are unable to walk
- Tenderness or pain when palpating (feeling) the area
- Bruising and or swelling (but not always)
- More on calf contusion
Cramp

Cramp in the calf muscles is a powerful and painful involuntary contraction. It usually occurs towards the end of a particularly hard training session, or possibly a few hours later. Symptoms consist of:
- A sudden, involuntary muscle contraction
- Stretching the muscles often releases the muscle spasm
- More on Cramp
Gradual onset (chronic) calf pain
The following are common causes of gradual onset or chronic calf pain:
Posterior compartment syndrome
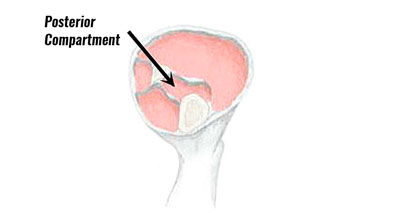
Posterior compartment syndrome occurs when the muscle swells up too big for the sheath surrounding it. Compartment syndromes can be acute, which occur suddenly, or chronic, which have developed gradually over time.
Acute symptoms:
- Occur suddenly following a contusion or direct trauma to the muscle
- Pain becomes progressively worse until severe
An acute compartment syndrome is a medical emergency, especially if the pain becomes progressively worse because it can result in long-term damage.
Chronic symptoms:
- Deep aching pain or tightness in the back of the lower leg
- Pain develops gradually during a run but eases with rest
- Experienced runners find the pain comes on at consistently the same point in a run
- More on Posterior compartment syndrome
Lateral compartment syndrome
- Lateral compartment syndrome can be acute or chronic the same as posterior compartment syndrome, only the pain is over the outside of the calf muscles.
- It is probably more common as a chronic injury in long-distance runners.
- More on Lateral compartment syndrome
Tight calf muscles
Although not a specific injury, tight muscles at the back of the lower leg are a widely seen problem among athletes and can lead to other related injuries. Tight calf muscles may be caused by:
- Poor foot biomechanics
- Lack of stretching
- Wearing high-heeled shoes.
If your calf muscles are partially contracted, or in spasm, the blood and nutrients cannot flow so easily, which may cause discomfort and pain. If left untreated, this can increase the risk of suffering from a more severe and acute injury.
- More on Tight calf muscles
Deep vein thrombosis
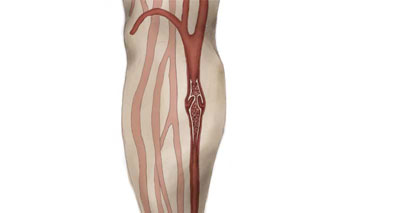
Deep vein thrombosis (DVT) is a possible cause of calf pain that should always be considered. It is a blood clot in the veins and is most likely to happen in the calf area, especially after long flights and surgery.
Although it is not as likely as the injuries above, it is a condition that should not be missed or overlooked. This is a serious condition and medical help is needed if this is suspected.
- More on Deep vein thrombosis
Fibula stress fracture
The calf muscles attach to the fibula bone, so the traction and twisting forces of the muscles can cause a stress fracture. Symptoms consist of:
- Pain at the back of the lower leg, towards the outside
- Difficulty weight bearing
- Pain increases with exercise
- More on Fibula stress fracture
Other causes of calf pain:
Calf pain may be referred from other body parts and produce pain in the calf.
It may originate from injuries to the spine, the knee (including Baker’s cyst and PCL injuries), and myofascial tissue structures (particularly in the gluteal muscles).
Trapped arteries or vessels, such as the popliteal artery also cause pain in calf muscles.
Trapped tibial and sural nerves in the calf may also make the lower leg area painful.
Immediate first aid for calf pain
Calf pain should be treated using the P.R.I.C.E. principles (protection, rest, ice, compression & elevation).
- Protection – Stop training or playing immediately to prevent the calf injury from getting worse.
- Rest – Resting the calf is important and vital for recovery. Try to reduce the demands of your daily activity and stop doing any sports that exacerbate the pain. Continuing to train with a calf injury and not allowing it time to heal can result in a more serious injury.
- Ice – Apply ice or cold therapy to the calf to help reduce the symptoms of pain and inflammation. Apply for 10 minutes every hour for the first 24 to 48 hours after injury, reducing to 3 or 4 times a day as symptoms improve. Do not apply ice directly to the skin as it may burn. Use a commercially available cold pack or wrap ice in a wet tea towel.
- Compression – Wearing compression support or compression bandages on the calf can reduce swelling.
- Elevation – Keeping the lower leg elevated above heart level can help to reduce swelling, due to the effects of gravity.
Read more on PRICE principles.
Rehabilitation programs
We have the following step-by-step rehabilitation programs available:
- Calf strain rehabilitation – a step-by-step rehab program for torn calf muscles.
Sports & activities
References & further reading
- Ekstrand J, Hägglund M, Walden M. Epidemiology of muscle injuries in professional football (soccer). Am J Sports Med 2011;39(6):1226–32.