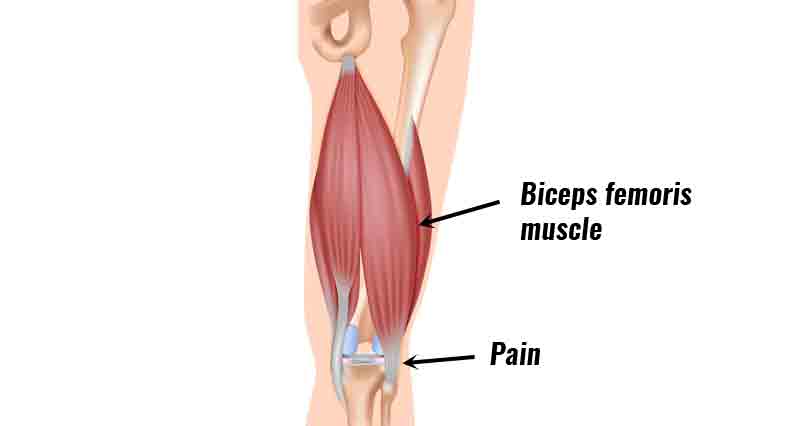
Posterolateral corner injury causes pain in the back and outside of the knee. They are not particularly common injuries, although around half of the cases occur due to sporting injuries, with road traffic accidents being another common cause.
Medically reviewed by Dr Chaminda Goonetilleke, 31st Dec. 2021
Symptoms of a posterolateral corner injury
The symptoms vary depending on how bad your injury is:
- Pain and swelling at the back and outside of the knee.
- Tenderness over the head of the fibula (outside of the knee).
- Knee instability.
- Hyperextension or over-straightening the knee.
- Walking with the knee continually bent to avoid hyperextension.
Imaging
An MRI is a useful investigation to do to identify all the damaged structures. Failure to recognise and repair other associated injuries (like an ACL sprain or PCL injury) could be a cause of treatment failure.
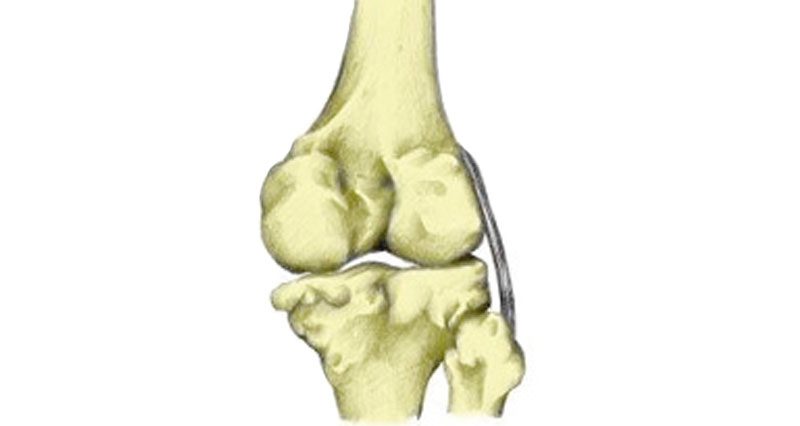
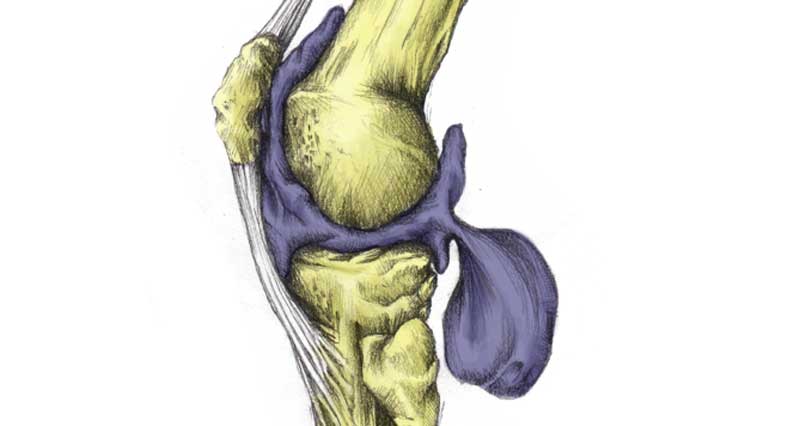
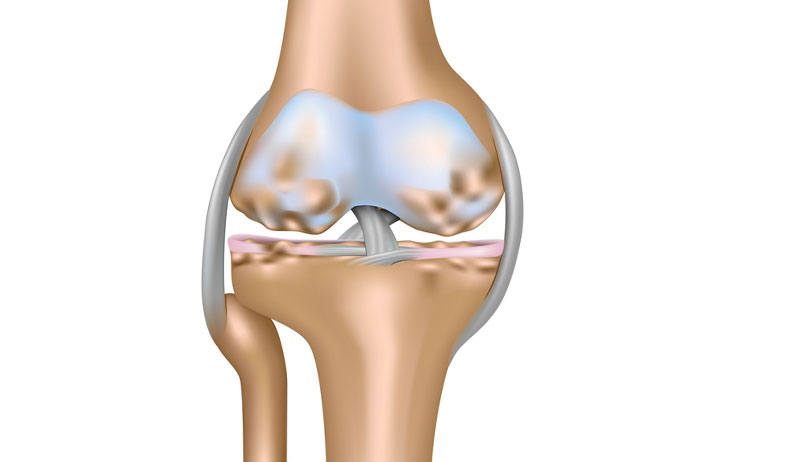
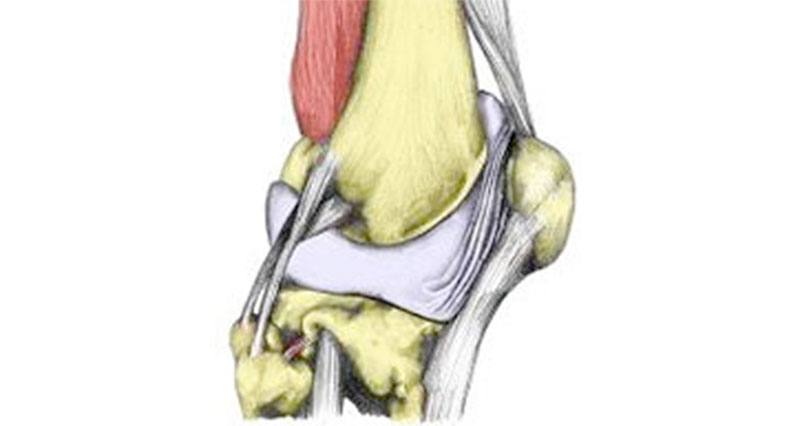
What is the posterolateral corner?
The posterolateral corner (PLC) consists of the following structures:
- Lateral collateral ligament
- Popliteo-fibula ligament
- Popliteus tendon
- The IT band
- Biceps Femoris tendon
- Peroneal nerve
- Patella retinaculum and lateral fascia
- Patellofemoral ligament
Together these structures help to stabilise the knee joint against backward and external (outward) rotation forces on the knee.
Causes and classifications
Hyperextension (over-straightening) of the knee is a common cause of this injury. For example, a force from the front and inside of the knee.
What commonly happens in sports injuries is soft tissue structures are pulled away from their bony attachments. PLC injuries often occur in conjunction with other knee injuries, particularly to the anterior cruciate ligament, posterior cruciate ligament, as well as tibial plateau fractures.
PLC injuries are graded 1, 2, or 3 depending on the extent of the injury.
Classification is based on the amount of ‘joint gapping’. This is assessed when your therapist stresses the outside (lateral) joint. They also determine the ‘end feel’.
They are classified depending on the degree of joint gapping when the therapist manually stresses the lateral joint, as well as the end, feel when performing this movement.
- Grade 1 injuries demonstrate a 3-5 mm gap with a clear endpoint.
- A 5-10mm gap, still with a clear endpoint for grade 2 injuries.
- Grade 3 injuries demonstrate more than a 10mm gap, with a very soft or even nonexistent end-feel.
Treatment
Treatment of PLC injuries depends on the severity of your injury.
Grade 1 and mild grade 2
Treat grade 1 and lesser grade 2 injuries conservatively. This means without surgery.
- Wear a hinged knee brace.
- Controlled weight-bearing for 2-4 weeks. Use a crutch or walking stick.
Then, a full rehabilitation program. The aims of which are to regain full range of motion and build strength, in the quads in particular.
Severe grades 2 and 3
More severe grade 2 and grade 3 injuries require surgical treatment.
Your surgeon can usually repair an acute injury if it is less than 3 weeks old. More chronic injuries require surgical reconstruction.
Repair is not possible after the acute period has passed. This is due to the development of scar tissue as well as joint misalignment. Your surgeon takes a graft from elsewhere in the body, For example, the Achilles tendon, IT band, patella tendon, semitendinosus tendon (one of the hamstring muscles), or the anterior or posterior tibialis tendon. This is used to recreate the ruptured structures.