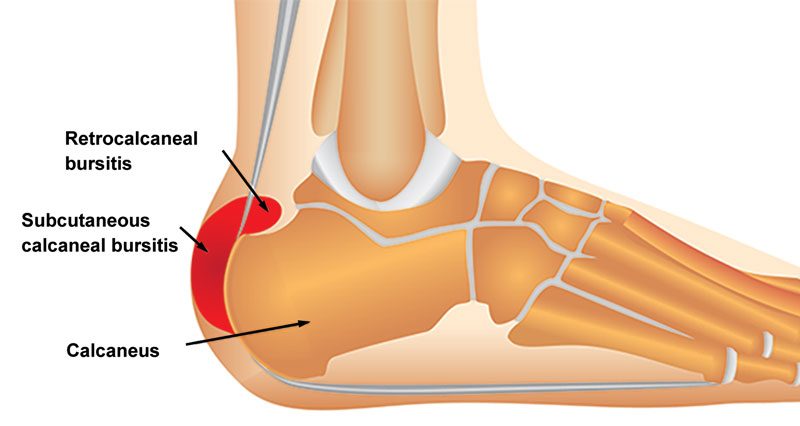
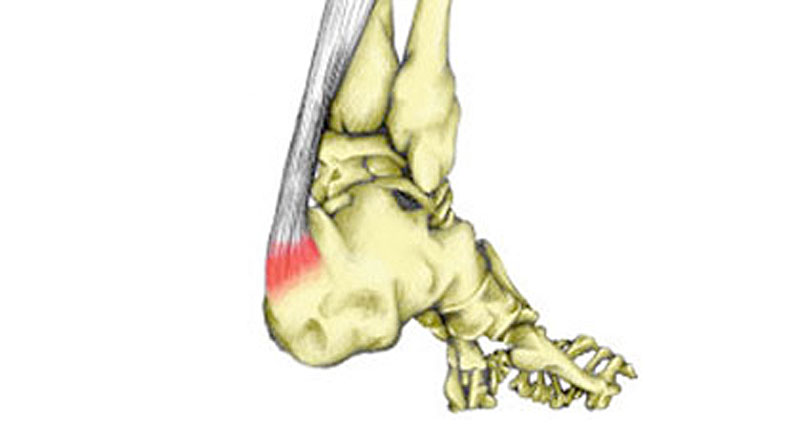
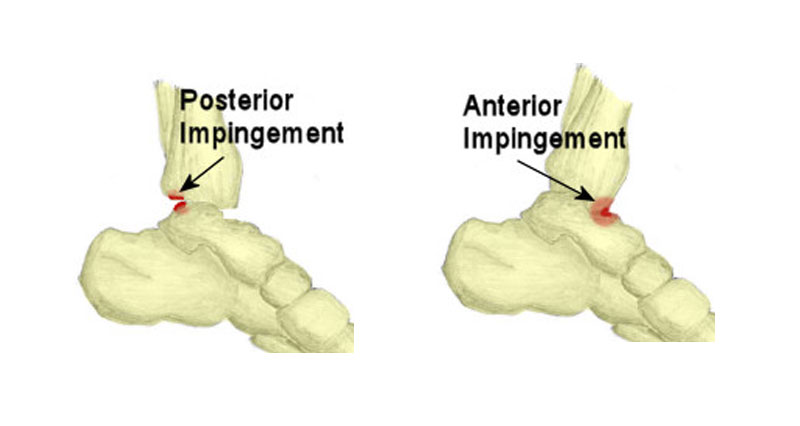
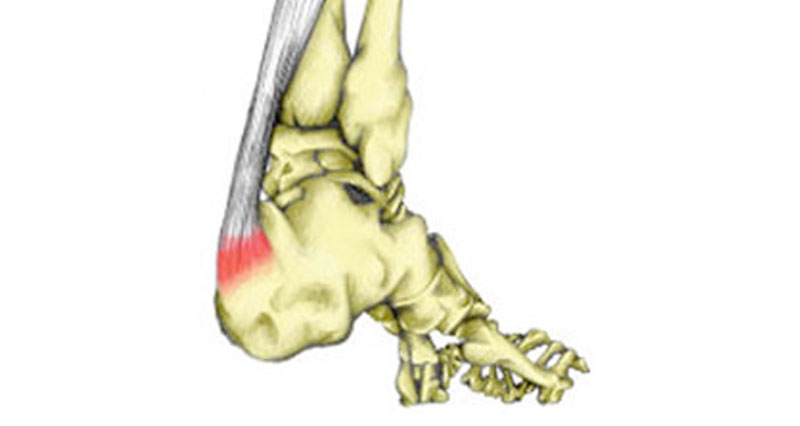
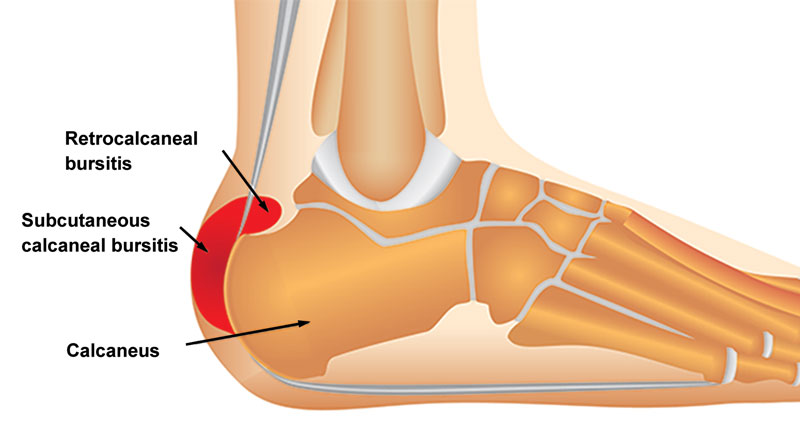
Achilles bursitis is also known as Retrocalcaneal bursitis. It is inflammation and swelling of a bursa at the back of the heel. Here we explain the symptoms, causes, and treatment of Achilles bursitis.
Symptoms
Symptoms of Achilles bursitis usually develop gradually over time and include:
- Pain at the back of the heel, especially when running uphill or on soft surfaces.
- Tenderness and swelling.
- Spongy resistance feeling when pressing in on both sides at the back of your heel.
Injuries with similar symptoms:
Be aware of the following which have similar symptoms:
- Sever’s disease – affects children and adolescents causing pain at the back of the heel.
- Insertional Achilles tendonitis – occurs in adults and is inflammation of the tendon at the point it inserts into the back of the heel.
- Achilles tendonitis – inflammation of the Achilles tendon, usually higher up in the ‘belly’ of the tendon.
- Haglund’s syndrome – is the term used when you have both Achilles tendonitis and Achilles bursitis at the same time.
What is Achilles bursitis?
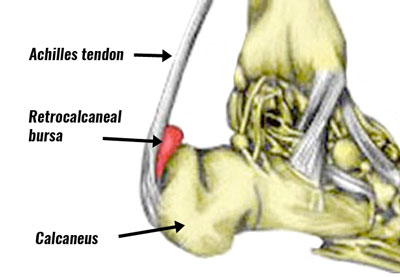
A bursa is a small sack of fluid that sits between a tendon and a bone. Its purpose is to help the tendon move smoothly over the bone.
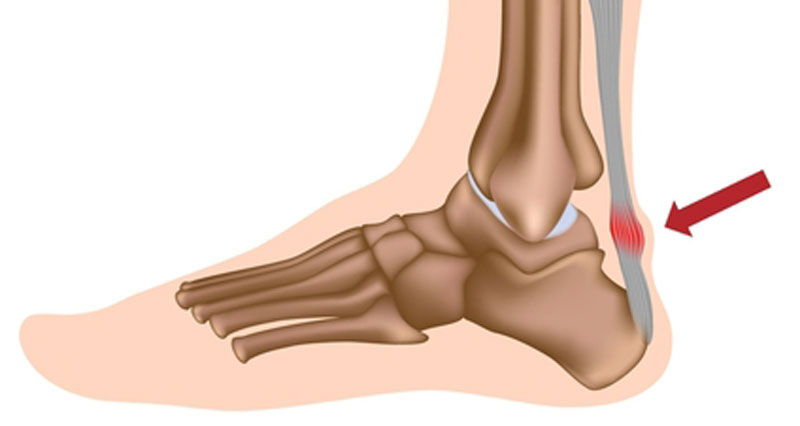
The retrocalcaneal bursa sits between the calcaneus (heel bone) and the Achilles tendon. Repeated trauma through overuse may cause the bursa to become inflamed.
What causes Achilles bursitis?
Friction or pressure over the back of your heel is the main cause. However, there are a number of things that can increase your chances of getting this injury:
- Common causes of Achilles injuries include tight calf muscles and overpronation. Both of these are easily correctable.
- Stretching the calf muscles should be performed regularly, every day, in order to increase their flexibility. Both the Gastrocnemius and the Soleus muscles need stretching. Read more on how to identify tight calf muscles.
- Overpronation – is where your foot rolls in or flattens too much as you walk or run. This will cause your Achilles tendon to twist. Orthotic insoles are worn in shoes to correct this, therefore reducing the strain on your Achilles tendon.
- Poor footwear – wearing the correct running shoes is also very important. If you are unsure, visit a podiatrist, or a specialist running a shop for a gait analysis.
Treatment for Achilles bursitis
Treatment and rehabilitation of Achilles bursitis (retrocalcaneal bursitis) are based on reducing pain and inflammation, identifying possible causes, and gradually returning to full fitness.
What can the athlete do?
Rest – from activities that aggravate it. If running makes it worse then refrain from running until such time as pain allows. You may be able to swim or cycle. It is important to try to maintain some kind of fitness. This stage may take anything from a couple of days to a couple of weeks.
Ice – apply cold therapy or ice. Ice should not be applied directly to the skin as it may cause ice burns but wrapped in a wet tea towel. Commercially available hot and cold packs are often more convenient than using ice.
Taping the bursa with a doughnut-shaped pad to take some of the pressure from footwear may help.
Shoes – wear shoes without backs to them. Or cut out part of the back of an old pair. This relieves pressure on the back of your heel. A foam ring cut to fit around the bursa to protect it from rubbing on the shoe may take the pressure off the bursa and allow it to heal faster.
Professional treatment
Medication – a doctor may prescribe anti-inflammatory medication e.g. ibuprofen to reduce the pain and inflammation. You should check with a doctor before taking any medication. Ibuprofen should not be taken by anyone with asthma.
Electrotherapy – such as ultrasound may reduce inflammation and swelling.
Steroid injection – followed by 48 hours of rest may be given for persistent cases.
Surgery – if the bursitis is particularly bad and does not respond to conservative treatment then surgery is also an option.
Exercises

Stretching exercises, in particular for the calf muscles should be done when recovering from Achilles-related injuries.
The calf muscles consist of the larger gastrocnemius muscle and the lower soleus muscle. If these muscles are more flexible then they will put less strain on the bursa at the back of the heel. Stretching should only be done if you are pain-free.
Calf stretches should be done with the knee both straight and bent in order to properly stretch both the Gastrocnemius and Soleus muscles.
View all calf stretching exercises.
Returning to full fitness
When the pain has gone, slowly build back to your original level of exercise. Aim to start back at 50% of your original workload, although this may be less depending on your fitness and the amount of time you have spent resting.
It is important to remove any irritation to the bursa. Check that the shoes are not rubbing on the bursa or cut away any material that might cause irritation of the bursa.
If you have looked after yourself you should be back to full training within two to three weeks. Be patient and allow about a week of active rest for the bursa.
Running
The following is a basic guideline for returning to training. This will vary depending on previous fitness and the extent of the injury.
| Day | Activity |
| 1 | Walk 4 minutes, jog 2 minutes, repeat four times |
| 2 | Rest |
| 3 | Walk 4 minutes, jog 3 minutes, repeat three times |
| 4 | Rest |
| 5 | Walk 3 minutes, jog 4 minutes, repeat four times |
| 6 | Rest |
| 7 | Walk 2 minutes, jog 6 minutes, repeat four times |
Continue this gradual progression until you can confidently run and resume normal training.