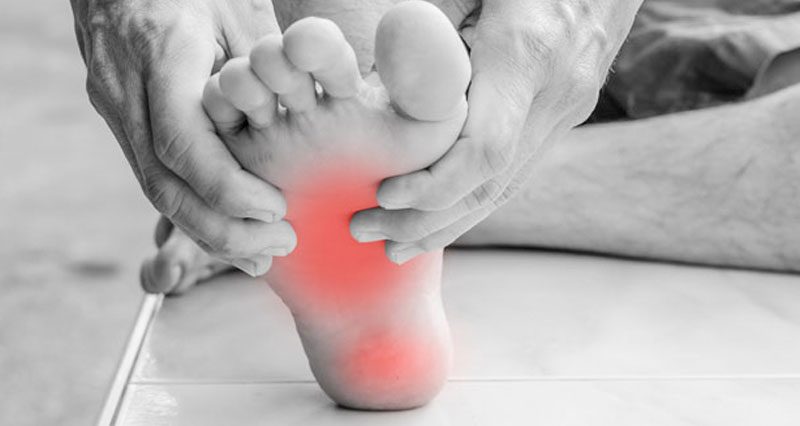
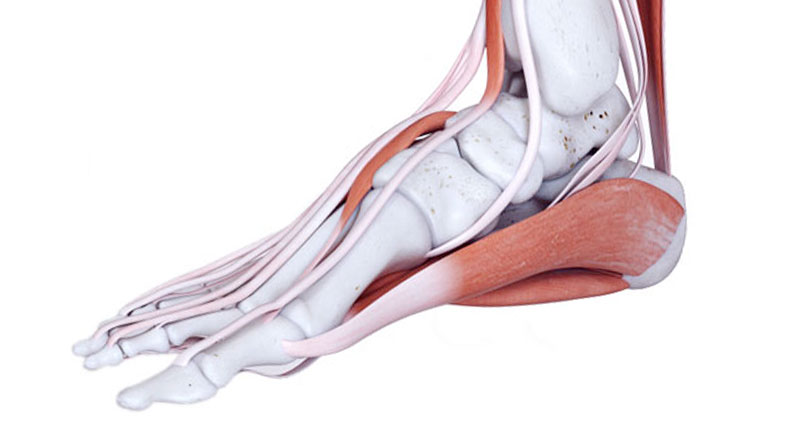
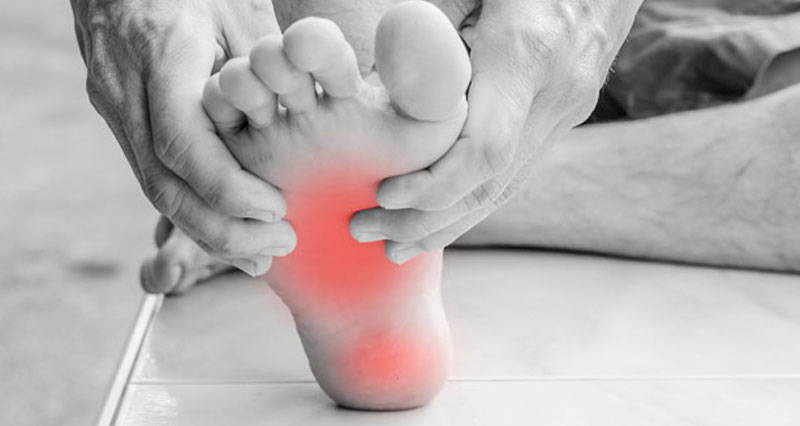
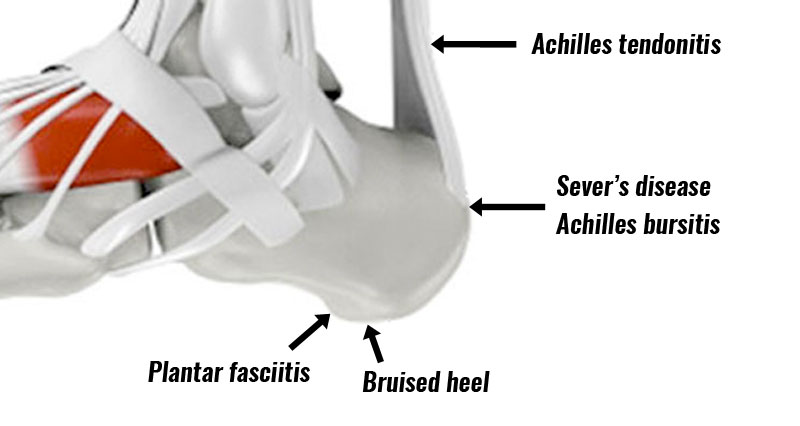
Here we explain the causes of midfoot pain. Pain in the middle of the foot can develop gradually through overuse, or suddenly following direct trauma such as a sprained ankle.
Medically reviewed by Dr. Chaminda Goonetilleke, 4th Jan. 2022
Sudden onset/acute midfoot pain
Acute midfoot pain occurs suddenly. You will most likely know the exact point in time when your injury occurred.
Midtarsal Joint Sprain
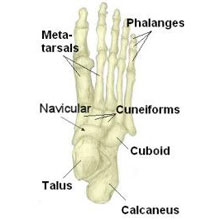
A midtarsal joint sprain is an injury to the ligaments which hold the tarsal bones in the middle of the foot together.
- Symptoms include pain on the outside middle of the foot, but the exact location will depend on which particular ligament is injured.
- You may have swelling on the top of your foot.
- It is relatively rare but can occur in gymnasts, footballers, and jumpers.
More on Midtarsal joint sprain
Tarsal Fracture
The term ‘Tarsal fracture’ specifically refers to the rare occurrence when one of the Tarsal bones in the rear of the foot is fractured.
- Tarsal fractures can be sudden onset acute fractures or stress fractures caused by overuse.
- The tarsal bones are rarely fractured in isolation but may occur after a hard impact or from repetitive forces.
More on Tarsal fractures
Plantar Fascia Strain
The plantar fascia, or arch ligament, is a band that runs from under the heel to the front of the foot. A strain or rupture to this ligament may cause a small lump to appear, and the area will be painful and tender. The injury might be caused by one single traumatic incident, resulting in sudden pain, or may gradually develop over time.
More on Plantar fascia strain
Abductor Hallucis Strain
The abductor hallucis muscle lies along the inside of the foot and runs from the heel bone inserting onto the side of the big toe. The muscle supports the arch of the foot so when it is strained it causes pain in the area. The sole of the foot may be tender and the affected foot may overpronate. Resting to allow the muscle to heal is key to recovery and easing the pain.
More on Abductor hallucis strain
Peroneus brevis tendon injury
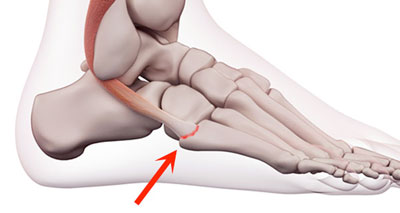
The Peroneus Brevis tendon inserts into the 5th metatarsal bone on the outside of the foot. This foot injury is normally caused by a sudden force or movement of the ankle, which creates midfoot pain on the outside of the foot. Bruising and swelling may also show, with the foot being painful to walk on.
More on Peroneus brevis tendon injury
Lisfranc Injury
Lisfranc injury is a dislocation or fracture in the midfoot area, specifically in the joint where the tarsal bones meet the long metatarsal bones in the foot The main symptoms are swelling on the top of the foot and pain when weight is placed on the foot. There may be some deformity in a few cases.
More on Lisfranc injury
Gradual onset/chronic causes of midfoot pain
Chronic midfoot pain develops over time, often becoming progressively worse.
Cuboid syndrome
Cuboid syndrome occurs when the peroneus longus muscle in the lower leg applies excess traction onto the cuboid bone causing it to partially dislocate.
The exact mechanism of this injury is unclear but is thought to occur when there is forceful eversion of the cuboid bone when the calcaneum is inverted. The peroneus longus muscle may play a role in this injury as this muscle causes the cuboid to evert.
- Symptoms are similar to an ankle sprain.
- Weight-bearing will be painful.
- It often occurs alongside an ankle inversion sprain, although not in every case.
More on Cuboid syndrome
Stress Fractures of the Foot
A stress fracture can occur from continuous and repeated loads on the legs. Long-distance runners are susceptible to this injury. A stress fracture in athletes occurs mainly in the lower leg and foot (in the calcaneus, navicular and metatarsal bones), with the affected area, aching and showing tenderness.
- More on foot stress fractures
Flexor Tendonitis/Tendinopathy
Flexor tendonitis occurs when the flexor tendons in the foot become inflamed. A more accurate term is tendinopathy because most cases are thought to be degeneration of the tendon rather than acute inflammation.
The tendons run down the inside of the ankle and under the foot to the toes. When they are injured, it can cause foot pain, particularly in the arch of the foot and the inside ankle. Bending the big toe back against resistance may also hurt.
- More on Flexor tendonitis
Extensor Tendonitis/Tendinopathy
Extensor tendonitis/tendinopathy is inflammation or more likely degenerative damage of the extensor tendons resulting in pain on top of the foot. The tendons run along the top of the foot and straighten the toes. Symptoms are worse during activity. It is brought on by overuse, or even fitted or too tight shoes.
- More on Extensor tendonitis
Navicular Stress Fracture
A navicular stress fracture is one of the most common stress fractures affecting athletes, especially those in explosive events such as sprinting and jumping.
Poor technique may increase the risk of a navicular stress fracture. The injury is often caused by overuse and repetitive stress. It may cause pain in the arch of the foot, which intensifies during activity and eases with rest.
- More on Navicular stress fracture
Tarsal Coalition
Tarsal coalition is when the tarsal bones in the foot fuse, or stick together. The tarsals are 7 bones located at the back of the foot. It is a congenital disease meaning you are born with it. Midfoot pain may appear in adolescents, especially after hard activity. However, symptoms may not develop until later in some people.
- More on Tarsal coalition
Tibialis Posterior Tendinopathy
The tibialis posterior tendon passes down the back of the leg, inside of the ankle, and under the foot. Overuse can cause the tendon to degenerate where it inserts into the foot bones, which can make the inside of the foot painful. This pain may radiate along the tendon and may worsen when the foot is turned inwards or outwards.
- More on Tibialis posterior tendinopathy
References
- Karas MA, Hoy DJ. Compensatory midfoot dorsiflexion in the individual with heelcord tightness: implications for orthotic device designs. J Prosthet Orthot 2002;14:82–93.
- Khan KM, Fuller PJ, Brukner PD et al. Outcome of conservative and surgical management of navicular stress fracture in athletes. Eighty-six cases proven with computerized tomography. Am J Sports Med 1992;20(6):657–66.