Adhesive capsulitis is the medical term for a frozen shoulder. It causes pain and restricted movement in the shoulder joint. A Frozen shoulder passes through three phases; a freezing phase, a stiff phase and a thawing phase.
Symptoms
Symptoms of a Frozen shoulder depend on the particular phase you are at:
Painful (freezing) phase
The freezing phase of frozen shoulder symptoms starts with a gradual onset of aching in the shoulder. The pain will often become more widespread and much worse at night making lying on the affected side difficult. This phase can last between 2 and 9 months.
Stiffening (frozen) phase
Symptoms during the frozen phase can last between 4 and 12 months. During this phase, the shoulder joint begins to stiffen up but is still likely to be painful. Normal daily tasks such as dressing or carrying bags become more difficult. You may notice your shoulder muscles start to waste away due to lack of use.
Thawing phase
During the thawing phase, frozen shoulder symptoms begin to improve. Range of movement increases and pain gradually decreases. However, pain may re-appear as stiffness eases for a time. The thawing phase can last 5 to 12 months.
What is a frozen shoulder?
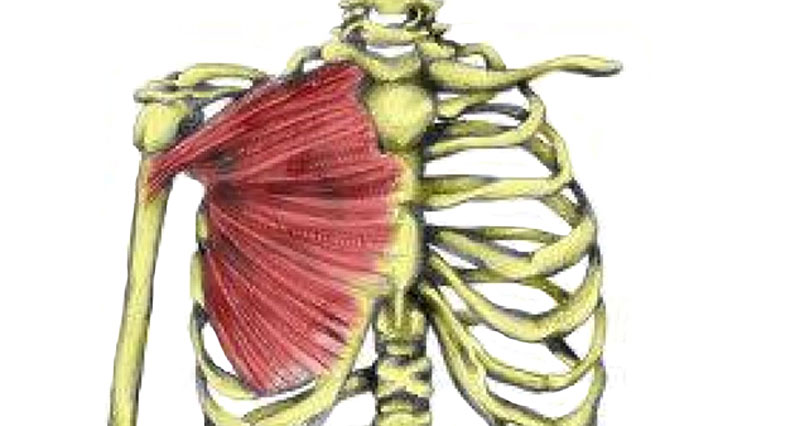
Frozen shoulder or adhesive capsulitis affects your ability to move the shoulder. It usually only occurs on one side, although it spreads to both shoulders in approximately one person in five.
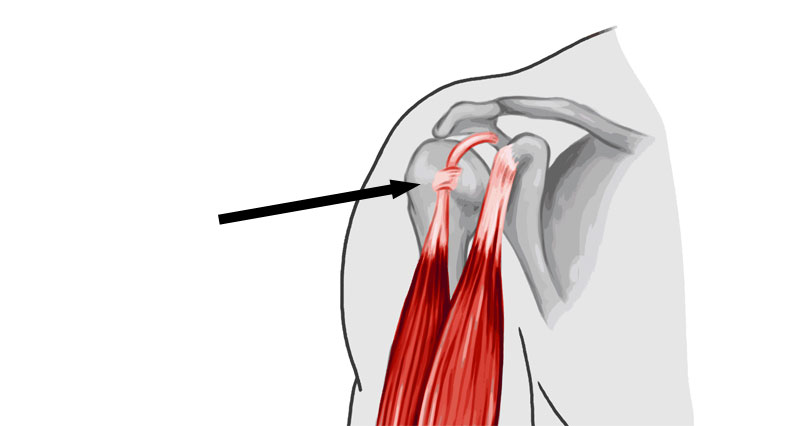
The medical term adhesive capsulitis literally describes the condition where adhesive means sticky and capsulitis means inflammation of the joint capsule. Symptoms may be because the joint capsule becomes inflamed and sticks. As a result, the whole joint becomes stiff and difficult to move.
This is not the same as arthritis, and it doesn’t affect other joints.
It is extremely uncommon in young people but almost always affects the 40 + age group, usually in the 40-70 age range. Frozen shoulder affects approximately 3% of the population with a slightly higher incidence amongst women. Also, Diabetics are five times more likely to suffer a Frozen shoulder.
Primary and secondary adhesive capsulitis
There are two classifications of adhesive capsulitis. Primary adhesive capsulitis occurs with no significant reason for pain or stiffness. Secondary follows as a result of an event such as trauma, surgery or illness.
What causes a Frozen shoulder?
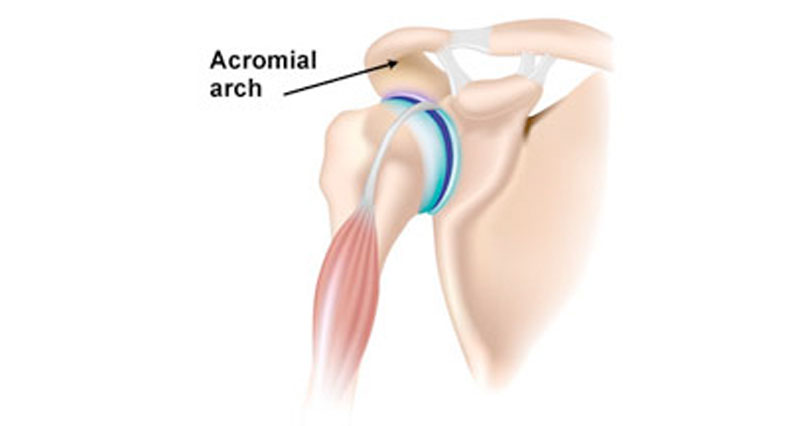
Exactly what causes a frozen shoulder is unknown. However, one theory is that the joint lining (capsule) becomes inflamed causing scar tissue. This leaves less room for the humerus or arm bone to move, hence restricting the movement of the joint.
Diabetics
The increased prevalence among diabetics (particularly insulin-dependent diabetics) may be due to glucose molecules sticking to the collagen fibres in the joint capsule, which causes stiffness. For this reason, diabetics are more likely to have both shoulders affected. Hormonal changes may be responsible for the higher incidence among women, particularly due to the increased prevalence around the menopausal period.
Some studies have shown that poor posture, particularly rounded shoulders, can cause shortening of one of the ligaments of the shoulder, which may also contribute to this condition. Also, prolonged immobility (such as after a fracture) may cause this condition to develop.
Frozen shoulder treatment
What can the athlete do?
Seek medical advice if you think you may have this condition, as early treatment can help prevent really severe stiffness from setting in. Follow any advice given by medical professionals, particularly with regard to a rehabilitation program.
Try to keep the shoulder moving even if it is just small pendular movements. If movement is very painful this should only be done under the guidance of a qualified therapist. Mobility exercises can help keep the shoulder mobile and should be done regularly if pain allows.
What can a Sports injury professional do?
Frozen shoulder is usually managed conservatively, with surgery as a last measure if all other attempts fail. Arrange a course of physiotherapy and exercises which will help maintain mobility and flexibility in the shoulder as best as possible.
A doctor may prescribe oral steroids or anti-inflammatory medication to reduce inflammation in the shoulder joint. Or a direct injection of steroid medication into the joint will also reduce inflammation. If conservative treatment fails to bring about any significant improvement then surgery may be recommended.
Rehabilitation program
The exercises and other treatment methods are dependent on which phase of rehabilitation the patient is at. We recommend seeking professional advice before attempting any rehabilitation.
Go to Frozen shoulder rehabilitation program.
Surgery
Surgery is a last resort if normal treatment has failed. An arthroscopic capsular release is the technique most often used and is done via keyhole surgery. The technique involves dividing the thickened shoulder capsule to release it. It is important that surgery is followed by an aggressive rehabilitation program and that the patient sticks to it.
Recovery time
Most cases will resolve on their own or with physiotherapy over a 1-3 year period, however, it is a slow recovery process. Some studies have reported positive results following arthroscopic surgery to release the tight capsule, however, this is currently only offered to patients who have not improved with conservative treatment. Many patients have reported persevering with mobility exercises as best they can but the condition just has to work its way through the three phases.