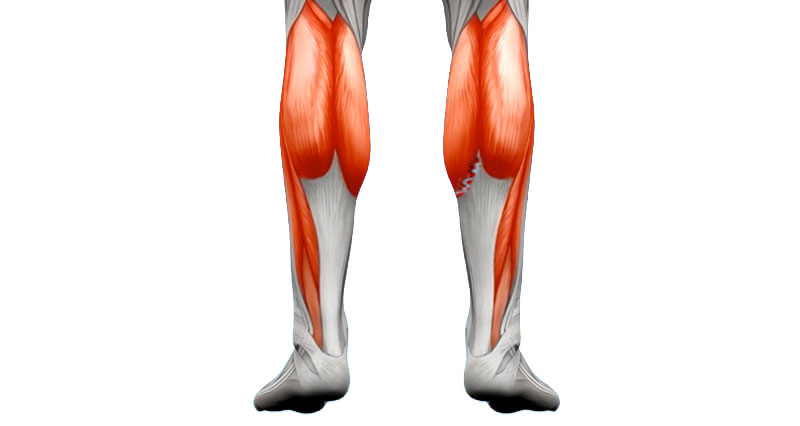
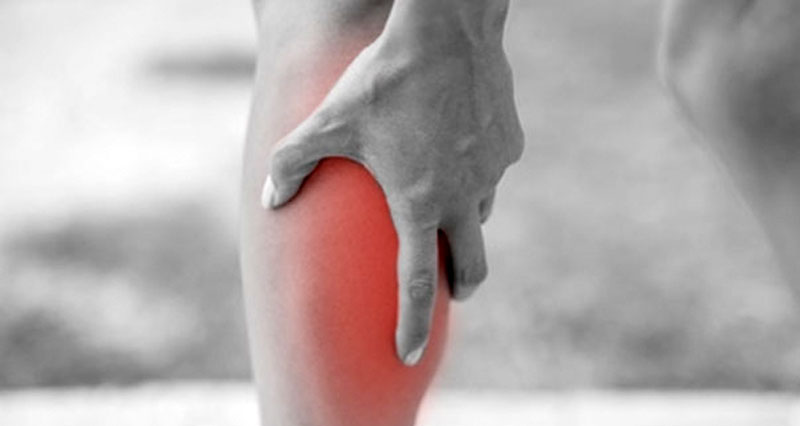
How bad is my Calf strain? Injuries are categorised into grades 1, 2, or 3 depending on severity.
Grade 1 | Grade 2 | Grade 3 | Calf Strain Rehabilitation Programs
Mild Grade 1 injuries
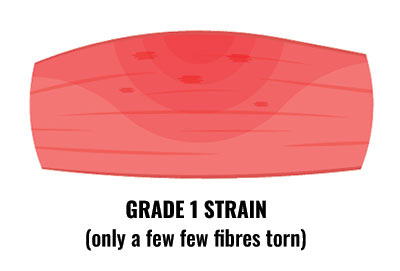
A Grade 1 strain is a minor tear of the muscle with less than 25% of the muscle fibres affected. Symptoms consist of:
- A twinge in the back of the lower leg, or simply a feeling of tightness.
- You may be able to carry on playing or competing with minimal pain.
- However, more tension or aching in the calf muscle is likely after. This may take up to 24 hours to develop.
Grade 1 strains easily turn into grade 2 strains if not treated properly.
Moderate Grade 2 injuries
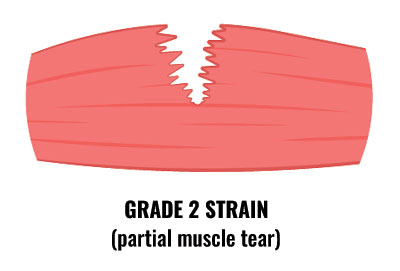
Grade 2 strains are more severe, with between 25% and 90% of the muscle fibres torn. Symptoms include:
- Sudden sharp pain at the back of the lower leg, with swelling likely.
- Bruising may develop over the following couple of days.
- Pushing up onto your toes is painful.
- Significant muscle weakness.
Severe Grade 3 injuries
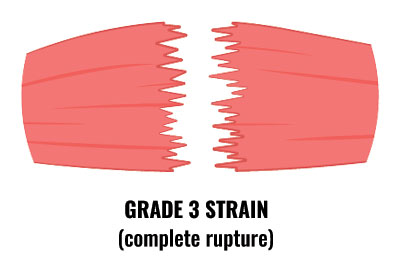
Grade 3 injuries are the most severe and involve 90 to 100% of the muscle fibres. Another name for a
complete tear is a rupture. Symptoms include:
- Severe and immediate pain in the back of the lower leg.
- A ‘pop’ sensation at the time of injury.
- You will be unable to walk or will walk with a significant limp.
- Swelling develops rapidly within an hour or so and bruising is also likely to be visible.
- This is a result of the torn muscle fibres and associated blood vessels.
- A gap or deformity in the muscle may be visible as the torn fibres bunch up towards the knee.
Calf tear tests
Your physio or doctor will perform a number of tests to help identify if you have a torn calf muscle.
Active ankle mobility
You may be asked to move your up and down by yourself without any resistance. This stretches your calf muscle when you pull your foot up (dorsiflexion) and contracts it when you point your foot down (plantar flexion).
If you have calf pain doing this then it may indicate a calf strain, probably a severe one.
Resisted plantar flexion
This involves trying to point your foot downwards against resistance. This may be from your therapist resisting the movement with their hands. Or if you have a particularly mild calf strain then you may need to perform a single leg calf raise whilst standing to reproduce painful symptoms.
More on Calf strains
- Calf strain overview – anatomy, causes & treatment
- Massage – how to apply sports massage techniques
- Rehabilitation program – full Calf strain rehabilitation program