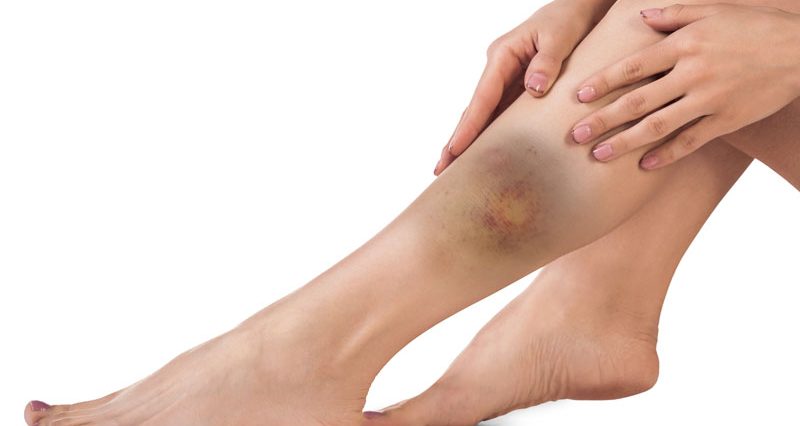
A calf contusion is caused by a direct impact or trauma to the muscle. Immediate first aid is important to avoid long term complications.
Symptoms of a calf contusion
Symptoms of a Calf contusion include:
- Instant pain following a direct blow or impact
- Pain varies in severity from a niggle to severe, disabling pain
- Loss of function and unable to walk or run properly
- Pain stretching the muscles
- Bruising may appear but not always
What is a contusion?
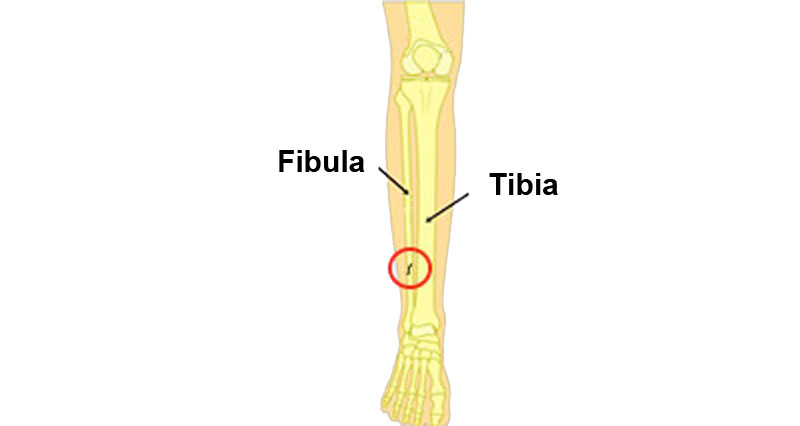
A contusion is an injury to a muscle caused by direct impact or trauma.
This can be from a piece of equipment such as a baseball or hockey stick, or from direct impact to an opponent’s knee in contact sports.
It is unlike a calf strain which occurs with no external contact.
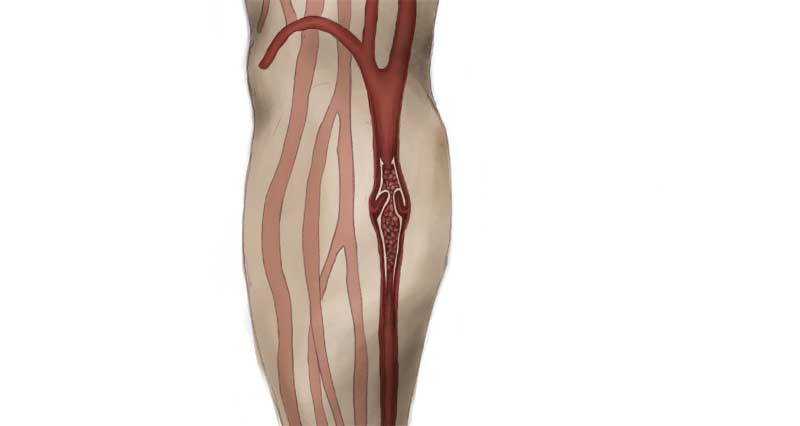
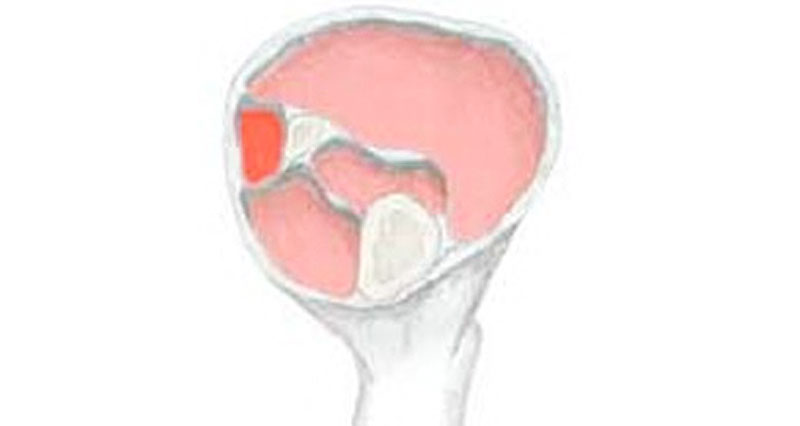
The muscle is crushed against the bone. This results in bleeding within the muscle. There are two types of muscle contusion.
Intermuscular contusions
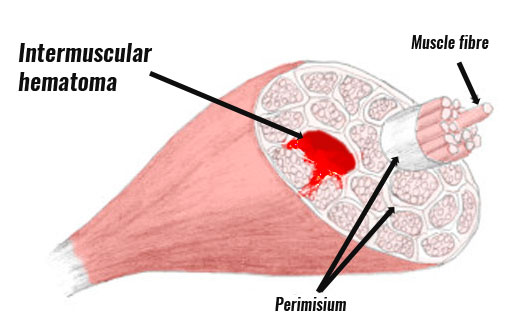
Muscles consist of bunches of muscle fibres surrounded by a muscle sheath. If the muscle sheath (fascia) is also damaged and bleeding can spread throughout the muscle then you are likely to see bruising develop. This is an Intermuscular contusion.
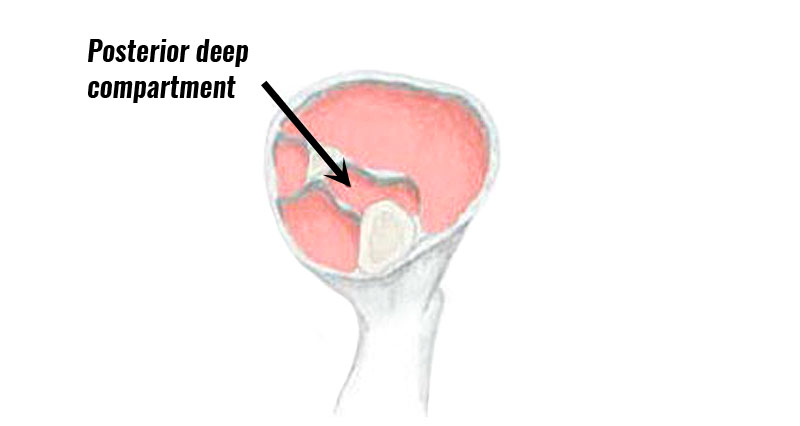
Intramuscular contusions
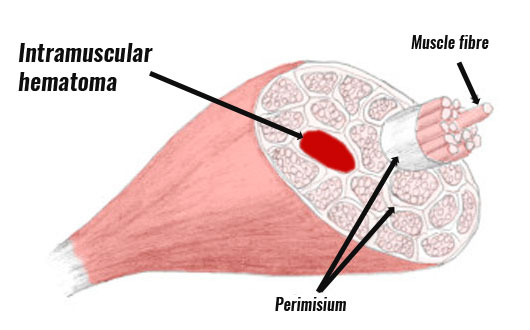
If the blood is contained within the sheath then it cannot disperse so easily. Although you are likely to have swelling and restricted movement, visible bruising will not occur.
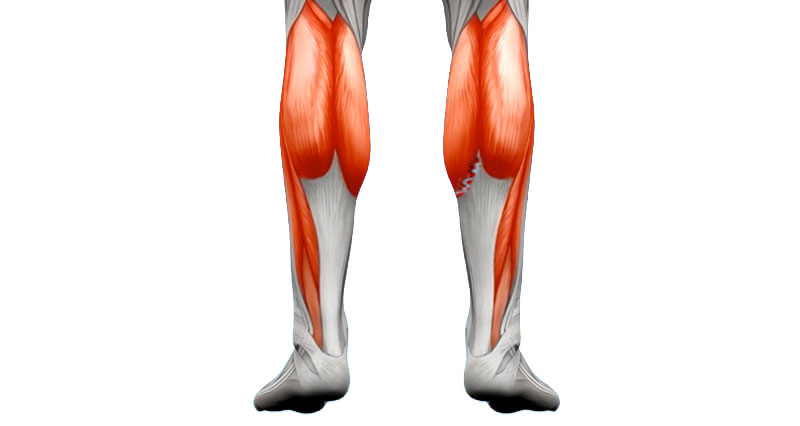
Structure of skeletal muscle
Complications of calf contusions
If you fail to treat a contusion properly then it may develop into something far more serious.
Myositis ossificans
If you do not apply ice, fail to rest, or massage the calf muscles too soon, then you run the risk of Myositis ossificans. This is where bone growth occurs within the muscle and can be very difficult to treat.
Myositis ossificans occurs because the muscle is crushed against the bone. As a result, your body mistakenly sends new bone repair cells to the site of injury. If left, a small lump of bone can form within the calf muscle.
- More on Myositis ossificans
Treatment for a Calf contusion
As soon as possible apply the PRICE principles (rest, ice, compression, and elevation).
Cold therapy/ice

Apply ice or cold therapy as soon as physically possible after injury and for 10 to 15 minutes every hour during the acute stage. This is usually the first 24 to 48 hours depending on how bad the injury is.
Do not apply ice directly to the skin as ice burns can occur. Wrap it in a wet tea towel, or use a commercially available hot and cold wrap.
Compression
Wear a compression bandage or support. This will help reduce bleeding and swelling. Elevating the limb will help bruising and tissue fluids drain away from the site of injury.
Should I massage my Calf contusion?
Only ever use sports massage after the acute stage has passed and any internal bleeding has stopped. This is usually a minimum of 3 days. Massage helps relax the muscles and disperses waste products from surrounding tissues.
However, if you apply massage to a muscle too soon after a contusion then myositis ossificans may occur.
- More on Calf massage
Rehabilitation & exercises
When comfortable to do so, begin gentle stretching exercises for the calf muscles.
The length of time you need to wait before beginning strengthening exercises will depend on how severe your contusion is.
- Read more on Calf contusion rehabilitation