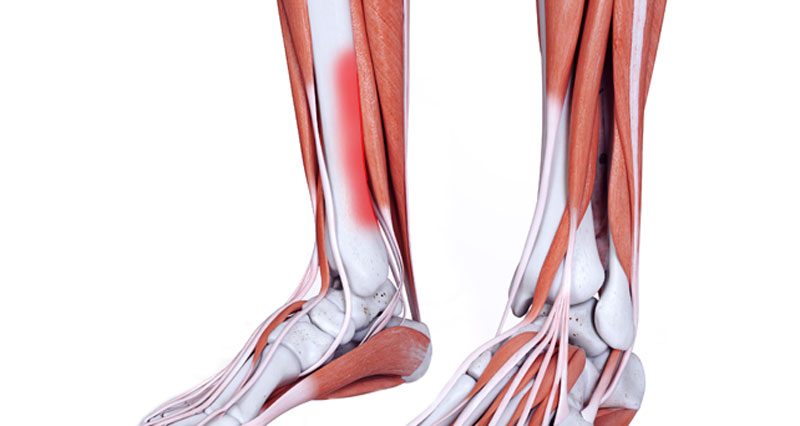
Shin splints are not a specific injury itself, but a general term often used to describe pain on the inside of the shin. Medial tibial stress syndrome is a common cause of shin splint-type pain.
Medically reviewed by Dr Chaminda Goonetilleke, 10th Jan. 2022.
Shin splints symptoms
The main symptoms of ‘shin splints’ or medial tibial stress syndrome include:
- Pain on the lower inside of the shin
- Symptoms usually develop gradually over time
- Pressing in (palpating) along the inside of your shin feels painful and tender
- You may feel lumps, and bumps along the inside of the tibia bone.
- Reddening of the skin over the inside of the leg due to acute inflammation
The lumps and bumps along the bone are because new bone grows in response to repeated trauma. Pain is often worse at the beginning of a training session, eases as the session progresses only to return later in the session, or the following day.
It is important to get an accurate diagnosis so the right treatment can be applied. Other injuries which may also cause shin pain include:
- Tibia stress fracture
- Compartment syndromes
- Popliteal artery entrapment
What are shin splints?
Shin splints are not a specific injury, but a term used to describe pain on the lower, inside of the shin. A number of specific injuries cause ‘shin splints’ type pain, but medial tibial stress syndrome is probably the most common.
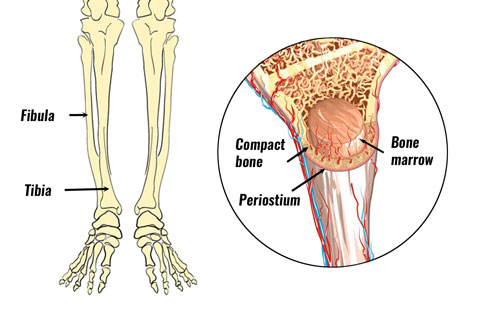
Medial tibial stress syndrome
Medial tibial stress syndrome occurs when the lower leg muscles repeatedly pull on the tibia (shin bone). The tibia is surrounded by a sheath called the periosteum. it is the periosteum surrounding the bone that becomes painful and inflamed. This is a result of the traction forces repeatedly applied by the soft tissues (muscles and tendons).
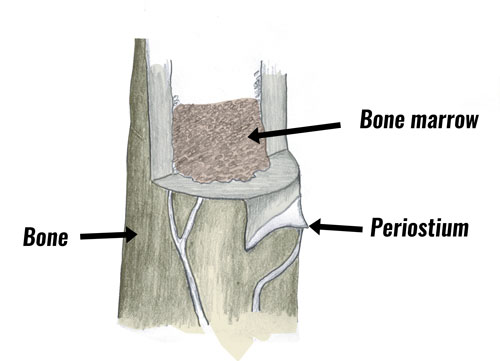
The lumps and bumps sometimes felt along the inside of the lower shin in chronic cases are from new bone growth as the tibia attempts to repair itself.
What causes shin splints?
Overuse is the primary cause, however, the following significantly increases your risk of shin splints:
- Training errors such as overtraining or insufficient recovery
- Overpronation, where your foot rolls in or flattens when running
- Over supination, where your foot rolls outwards too much
- Incorrect or poor-quality footwear
- Poor flexibility, particularly in the calf muscles
- Learn more about what causes shin splints
Shin splints treatment
Shin splint treatment involves reducing pain and inflammation, identifying and correcting training errors and biomechanical problems, and restoring muscles to their original condition through stretching, exercises, and massage. The full rehabilitation process may take anywhere from 3 weeks to 12 weeks.
Ice/cold therapy
Apply the PRICE principles of protection, rest, ice, compression, and elevation to reduce initial pain and inflammation.
Apply a cold therapy and compression wrap for 10 minutes every hour initially for the first 24 to 48 hours, reducing frequency to 3 or 4 times a day as symptoms improve.
Do not apply ice directly to the skin as it may burn. Either wrap ice in a wet tea towel or use a commercially available cold pack.
Rest
Rest is very important and often overlooked. This may mean ‘active rest’, where you reduce your normal training volume or replace running and jumping type activities with non-weight bearing activities such as cycling or swimming.
Or for more server injuries a period of complete rest for a few days may be appropriate. Use the shin taping technique to reduce load.
Medication
A doctor may prescribe anti-inflammatory medication e.g. ibuprofen to help reduce pain and inflammation. Although this should not be relied on as a long-term solution or excuse not to rest. Asthmatics should not take Ibuprofen.
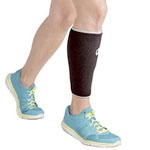
Wear a shin/calf support
Protect and support the area with a shin splint sleeve or compression support. This helps keep the muscles warm and supple and supports inflamed soft tissues.
Neoprene-type supports are best for retaining heat. Elastic-type supports provide good compression support.
Insoles
Wear shock-absorbing insoles in your shoes to help reduce the stresses on the lower leg, or wear softer training shoes/sneakers all the time until your symptoms have gone.
If you overpronate (where your foot rolls in/flattens) then you may benefit more from Orthotic inserts which provide more structural support to your foot.
Keep a training diary so you can look back and assess if the training load is too high.
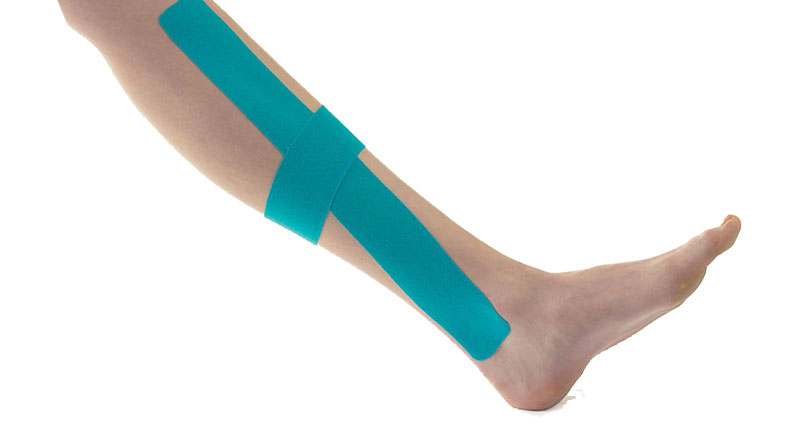
Shin splints taping

A simple taping technique can often instantly relieve symptoms by supporting the muscles of the lower leg.
- Tape is applied in a spiral pattern up and around the shin.
- It works by pulling muscle towards the bone.
- This reduces traction forces on the shin and allows the tissues to heal.
- Learn how to apply Shin splints taping
See a sports injury professional about shin splints
A professional therapist diagnoses your injury and identifies possible causes of your shin pain. Often patients rest until their pain is gone, only for it to return once normal training resumes. This is because the underlying causes are not addressed. A full biomechanical assessment identifies problems such as overpronation.
Massage
Sports massage may be beneficial after the first 3 days or so, once the initial acute stage has passed. Massage will reduce tension in the muscles which may be causing excessive traction forces on the bone. It will also increase blood flow aiding the healing process.
Exercises & rehabilitation for Shin splints

Exercises to stretch the muscles of the lower leg, in particular, the tibialis posterior (which is often associated with shin pain) are important. Stretching exercises should be done both with the knee straight and bent to target both the gastrocnemius muscle and the deeper soleus muscle.
Keep a training diary so you can look back and assess if the training load is too high. Although strengthening exercises may be required, this is an overuse injury, so a gradual increase in load and return to full fitness is important.
When can I start training again?
- When the walking has been pain-free for 2 weeks, you can begin running, but build up gradually.
- Apply tape to the shin to support it for the first few runs and ice afterwards to prevent/reduce inflammation.
- Stretch properly before and after each training session.
- More on Shin splints exercises
- Go to Shin splints rehabilitation program
References & Research
- Detmer DE. Chronic shin splints. Classification and management of medial tibial stress syndrome. Sports Med 1986;3(6):436-46
- Moen MH, Tol JL, Weir A et al. Medial tibial stress syndrome: a critical review. Sports Med 2009;39(7):523-46
- Tweed JL, Avil SJ, Campbell JA et al. Etiological factors in the development of medial tibial stress syndrome: a review of the literature, J Am Podiatr Med Assoc 2008;98(2):107-11
- Bennett JE, Reinking MF, Pluemer B et al. Factors contributing to the development of medial tibial stress syndrome in high school runners. J Orthop Sports Phys Ther 2001;31(9):504-10
- Griebert MC, Needle AR et al. Lower-leg Kinesio tape reduces the rate of loading in participants with medial tibial stress syndrome. Phys Ther Sport. 2016 Mar;18:62-67