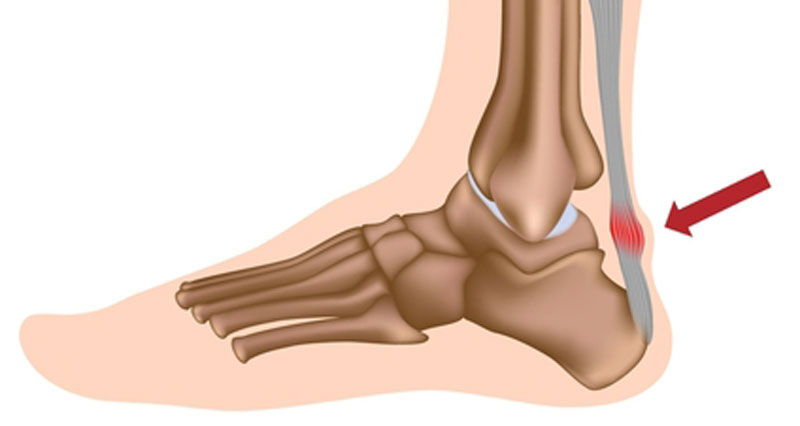
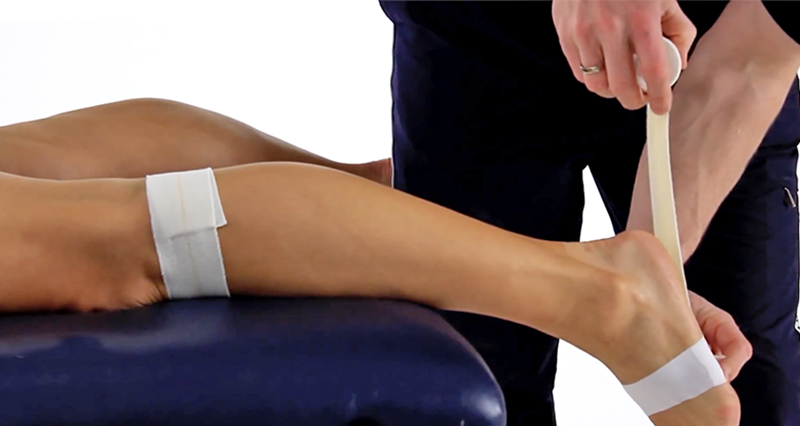
Achilles tendonitis heel drop exercises are effective in treating chronic Achilles tendon pain. Hakan Alfredson’s heel drop protocol involves twice-daily exercises for 12 weeks.
What is Hakan Alfredson’s heel drop protocol?
Alfredson created an Achilles rehabilitation program based on eccentric exercises, but made three innovations:
- If your Achilles pain gets worse, this is not necessarily a bad thing. It could just be part of the normal healing process.
- Heel drop exercises should be performed both with the leg straight and bent.
- A total of 180 repetitions should be done every day for 12 weeks. This is a lot more than most Achilles rehab programs would advocate.
Studies have shown Hakan Alfredson’s heel drop protocol to be one of the most effective treatments for chronic Achilles tendon pain.
Heel drop exercises
Eccentric exercises involve dropping the heel horizontally in a slow and controlled manner. An eccentric muscle contraction is one where the muscle gets longer as it contracts.
With heel drop exercises, the calf muscles at the back of the lower leg contract as they lengthen. Also, it is important to stretch these muscles regularly.
You must perform exercises daily for 12 weeks without fail. Some discomfort is likely. You may feel your injury is getting worse before you see improvement.
Why does Hakan Alfredson’s protocol work?
If you complete the two exercises strictly each day, this totals 180 repetitions per day for 12 weeks. In the short term, exercise:
- Increases tendon volume
- Stimulates collagen production
The tensile strength of the tendon will increase over time, making it able to cope better with the loads expected of it in day-to-day activities and sports training.
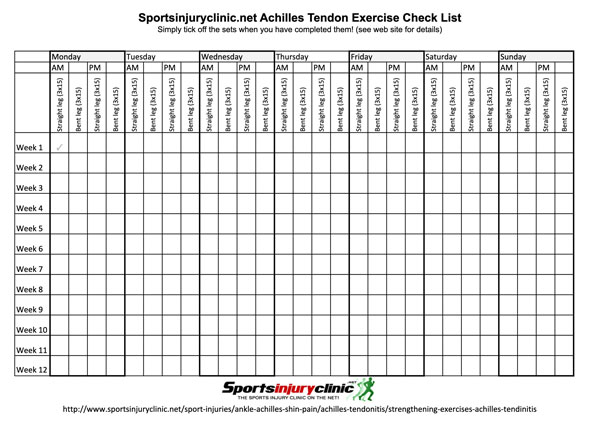
Keep a record of your exercises
It is important to keep a record of the exercises you do. Downloaded our 12-week exercise record sheet.
Heel drop eccentric strengthening exercises

For Achilles tendonitis, heel drop exercises are performed with the knee both straight and bent. This helps target the gastrocnemius and soleus muscles.
The gastrocnemius is the larger calf muscle. It originates from the femur (thigh bone), so it is best trained with the knee straight. Bending the knee reduces the involvement of the gastrocnemius. This places more load on the soleus muscle.
Teaching point:
- Begin standing with one foot on a step, heel raised.
- Slowly lower your heel in a controlled movement, keeping your leg straight.
- Lower until your foot is level with the step, but no further.
- Use your uninjured leg to help return to the starting position.
- Perform 3 x 15 repetitions, twice a day, every day for 12 weeks.
Some discomfort is normal. Symptoms may feel worse before they improve. Once the exercise becomes pain-free, increase the load gradually. You can do this by wearing a weighted vest or using a rucksack.
Soleus heel drop
You can do this in the same way as the heel drop exercises. Keep your knee bent at about 45 degrees (half squat position)
Stretching exercises for Achilles tendonitis
Achilles stretches don’t actually stretch the tendon much. It is the calf muscles that need stretching. Stretching is an important part of the treatment and rehabilitation of Achilles tendinitis. Tight or shortened calf muscles may increase the strain on the Achilles tendon, making it work harder.
Gastrocnemius stretch
- Place the leg to be stretched behind and lean forward, ensuring the heel is kept in contact with the floor at all times.
- Hold the stretch for 20 to 30 seconds and repeat it 3 times. This can be repeated several times a day and should not be painful.
- A stretch should be felt at the back of the lower leg. If not, then move the back leg further back.
- A more advanced version of a calf stretch is to use a step and drop the heel down off it.
Soleus stretch
- Keep the back leg bent to stretch the soleus muscle
- Place the leg to be stretched behind and lean against a wall, keeping the heel down
- A stretch should be felt lower down, nearer the ankle, at the back of the leg
- If this stretch is not felt, then a more advanced version is to place the forefoot of the front leg against the wall with the heel on the floor and push the knee towards the wall
Stretching on a step
- This stretch can be performed to stretch the calf muscles and Achilles tendon further. Stand on a step with the toes on the step and the heels off the back.
- Carefully lower the heels down below the level of the step until you feel a stretch – make sure you have something to hold on to!
- Hold for 15-20 seconds. This should be performed with the knee straight and then repeated with the knee bent to make sure you are stretching both muscles.
References
- Alfredson H, Lorentzon R. Chronic Achilles Tendinosis – recommendations for treatment and prevention. Sports Med 2000;29(2):135-46
- Alfredson H, Piettila T., Jonsson P et al. Heavy-load eccentric calf muscle training for the treatment of chronic Achilles tendinosis. American Journal of Sports Medicine 1998;26(3):360-6